SEXUALITY AND THE OLDER ADULT
Mar 18, 2022
Shilpa Srinivasan, MD, DFAPA, Juliet Glover, MD, FAPA, Rajesh R. Tampi, MD, MS, DFAPA, Deena J. Tampa, MSN, MBA-HCA, RN, Daniel D. Sewell, MD
Abstract
This paper provides an overview of biopsychosocial components of sexuality in older adults, sexual expression in older LGBTQ and cognitively impaired adults, and inappropriate sexual behaviors (ISB) in dementia.
Recent findings:
The sexual expression of older adults is influenced by diverse psychosocial and biological determinants including ageist beliefs. Although the prevalence of sexual dysfunction increases with age, studies of sexual satisfaction reveal that only a minority experience significant distress. Stigma against sexual expression in LGBTQ older adults may cause concealment of sexual orientation from family or care providers due to fears of rejection. Cognitive impairment affects the frequency of and satisfaction with sexual activity, as well as capacity to consent. Staff biases about sexuality can negatively impact sexual expression in healthcare settings. Dementia-related inappropriate sexual behaviors (ISB) are common and distressing. Recent research has focused on early identification and prevention of ISB, in addition to management through non-pharmacologic and pharmacologic approaches.
Summary:
Sexuality remains integral to the quality of life for many older adults and informed consideration of their needs is critical to healthcare delivery and institutional service planning. A comprehensive understanding of older adults’ sexuality can enhance education, research, policy, and clinical care for this growing population.
For more information: ali.ma@wecistanche.com

Click to cistanche tubulosa dosage for sexuality
Introduction
Sexuality, intimacy, and sexual identity are integral components of personal life [1]. Until recently, research on determinants of sexuality in older adults has been limited in scope [2]. Societal constructs have perpetuated ageist notions of older adults aging out of sexuality [1,3]. Biomedical models of sexual activity have focused on a pathology-based approach to dysfunction [4]. Furthermore, most studies have been qualitative in nature and focused on heterosexual older adults, with only limited studies in older lesbians, gays, transgender, and queer (LGBTQ) adults [5,6].
While sexual activity in older adults is closely tied to physical health, barriers to discussing these issues in the healthcare setting (e.g. in primary care) are multi-directional [7]. Ageist stereotypes of older adults being asexual or less-than-sexual beings may cause personal embarrassment and stigma concerns for patients and providers [1]. Systemic barriers to addressing these concerns include sub-optimal formal education across health professional training curricula, limited inquiry about sexual history during clinical evaluations, and insufficient awareness of referral and treatment options [8,9]. Staff attitudes towards sexuality and sexual expression in long-term care settings are particularly salient when considering the needs of cognitively intact and impaired residents, with implications for decision-making capacity and consent [10, 11]. Dementia-related ISB impacts the individual, peers, family, and residential settings posing additional challenges while offering learning opportunities to further compassionate clinical care [12].
Sexuality and Aging
Sexuality is a multifaceted construct spanning sexual activity, behavior, function, attitudes, motivation, and partnership [13]. Studies have shown that older adults continue to be sexually active in later life, with moderators of sexual activity being influenced by diverse factors, including gender, availability of partners (including partner health and sexual interest), previous levels of sexual activity, and overall physical and mental health [7,14]. Heterogeneous studies have found sexual activity and intimacy are associated with positive outcomes in
interpersonal relationships, physical and mental health, and quality of life [7,15].
Until recently, most studies of sexuality in older adults have predominantly focused on the physiologic impact of aging or the medical model of older adult sexuality and age-related physiologic changes that may impact the sexual response cycle in men and women [16]. More recently, research has shifted from a purely medical or dysfunction paradigm, to a more comprehensive biopsychosocial and interpersonal approach to sexual well-being [4,17]. In this section, the biological, psychological, and social-environmental constructs will be reviewed.
- Sexual Behavior
Older adults remain sexually active, and engage in genital (sexual intercourse, oral sex) and non-genitally focused (for e.g. touching, kissing, hugging) activity, as well as solitary sexual activity (masturbation) [18]. In a classic study of a nationally representative sample (n=3005) of older adults in the United States (US), 53% of respondents between the ages of 65-74 years and 26% of respondents between the ages of 75 to 85 years reported engaging in sexual activity with a partner in the previous 12 months [19]. In the same study, vaginal intercourse was the most commonly reported sexual activity across all age cohorts, followed by oral sex, and masturbation. More recently, data from the National Survey on Sexual Health and Behavior in the US showed similar findings: 53% of men and 42% of women between 60 to 69 years of age, and 43% of men and 22% of women over age 70 reported engaging in vaginal intercourse [4]. Population research conducted in Spain, Great Britain, and Australia have revealed similar findings [20-22].
- Psychosocial and Interpersonal Constructs
Various factors impact sexual expression in older adults. From a psychological perspective, these include knowledge and attitudes about sexuality, the importance of sexual activity, and cultural determinants. Western stereotypes have portrayed older adults as asexual, or alternately, older women and men as sexually predatory [23-25]. Positive attitudes about sexual expression and its importance, however, are associated with increased sexual activity [4]. The Midlife in the United States (MIDUS) project found that subjective age, positive views of sexuality, and good health status were positive predictors of interest in and quality of sex [26]. Relationship status also contributes significantly to sexual activity (and frequency) with a partner [4]. Studies have shown that older men and women with partners engage in sexual activity more frequently than those without partners [27]. The higher life expectancy of women further contributes to gender disparities in partner availability and sexual activity in older adults [27, 28].
- Aging and the Sexual Response Cycle
Changes in sexual function with aging must be correlated with the normal adult sexual response cycle. Consisting of desire, arousal/excitement, plateau, orgasm, and resolution/refractory period, these stages are physiologic and psychologic non-linear components and can be influenced by age-related changes [29] in the sexual response cycle occurring in both men and women. Menopause in women is associated with the most significant changes when declining estrogen levels lead to vaginal atrophy, reduced vaginal lubrication, and diminution insensitivity of the erogenous zones. In addition, decreased testosterone production in women also contributes to a reduction in libido and sensitivity of erogenous zones. Combined, the hormonal reductions may result in decreased desire, increased time to sexual arousal, discomfort during vaginal intercourse due to dryness, and decreased intensity of orgasm [30].
In older men, slowly declining testosterone levels are associated with diminished libido and sexual function but the impact is variable and less temporally correlated in comparison to the associations with hormone reduction in women [31]. Sexual arousal and time to orgasm is lengthened. Erections require more physical stimulation to achieve and are reduced in frequency and durability. Ejaculate volume during orgasm is reduced, and the refractory period is lengthened [4, 29, 30].
- Sexual dysfunction vs. difficulty
Whereas the majority of older adults continue to engage in intimacy and sexual activity, the prevalence of sexual dysfunction advances with age, which, in turn, has strongly driven recent developments of pharmacologic agents to treat sexual dysfunction [7, 32]. Lindau et al. found that half of 3005 older adults (ages 57-85 years) in the United States reported at least one sexual problem [19]. Low sexual desire (43%) was the most prevalent reported sexual difficulty in women, and erectile difficulties (37%) were most prevalent among male respondents [19]. Limitations of this and similar studies have been the self-reported nature of data and study participants limited to sexually active individuals who were predominantly white. Globally, studies have found mental disorders such as depression, medical conditions such as diabetes, and iatrogenic factors to be predictors of sexual dysfunction among older adults through direct (vascular) or indirect (pain, physical disability, and poor perceived health) mechanisms [33, 34].
Notably, however, distress about sexual difficulty has been less robustly quantified and studied. This represents a significant oversight, given that the presence of “clinically significant distress” is a Diagnostic and Statistical Manual (DSM) criterion for the diagnosis of sexual dysfunction [35]. Despite the prevalence of sexual difficulties in older adults, studies of sexual satisfaction have shown that only a minority experience significant distress. In a cross-sectional study of 297 adults ages 65 to 75 years, over 60% experienced at least one sexual difficulty, but only 25% reported distress related to that difficulty [36]. After controlling for sexual domains and partnership characteristics (quality and frequency of sexual activity), a prospective study of 6000+ older adults found that sexual quality of life increased with age, arguing against ageist stereotypes of sexual expression terminating in older adulthood [37, 38].

Sexuality in Older LGBTQ adults
Until recently, very few research efforts included questions about sexual orientation or gender identity. As a result, information about older LGBTQ adults and their sexual expression in later life remains limited. In this section, the diversity of the aging LGBTQ population and the impact of setting on sexual expression in older LGBTQ adults will be explored.
- Diversity within Diversity
Recognizing and adapting to the diversity within the population of older LGBTQ adults is a prerequisite for providing optimal care. Each letter in the LGBTQ acronym refers to a unique sexual or gender minority group with heterogeneous issues pertinent to each of these groups. In addition to ethnic, racial, religious, educational, and socio-economic differences, diversity within the LGBTQ community also relates to age. For example, the Aging and Health Report indicates that, among older LGBTQ adults, the rate of victimization due to LGBTQ identification increases with age, and the rate of internalized stigma for those 80 and older is higher than those 50-64 and 65-79 years. [39].
Although legal protections from discrimination and societal acceptance of members of LGBTQ communities have been increasing, many older LGBTQ individuals, especially those who came out when much younger, have experienced one or more forms of personal victimization directly attributable to their gender identity and/or sexual orientation. The legacy authored by these experiences includes internalized homophobia and negative impacts on sexual expression and sexual quality of life. Eighty-two percent of the older LGBTQ individuals who participated in the initial phase of the Caring and Aging Study reported experiencing at least one-lifetime episode of victimization because of actual or perceived sexual and/or gender identity discrimination, and 64% reported experiencing at least three or more episodes [39]. While many LGBTQ individuals suffer enduring negative impacts on the quality of their sexual lives, most have also found ways to cope or even thrive [39].
- The Impact of Living Arrangements on Sexual Intimacy of Older LGBTQ Adults
Where and with whom one life impacts sexual intimacy of older adults. This is especially true for older LGBTQ adults. Living arrangements for older individuals can be divided into five categories: living in one’s own home; moving in with family, renting a room or home; group housing such as residential care facilities or assisted living communities and nursing homes. Each of these options comes with benefits and challenges. Although the same spectrum of housing options for older heterosexual and cisgender individuals are theoretically available to older LGBTQ individuals, some of the possible options may be uniquely problematic for older LGBTQ individuals based on factors such as acceptance by family members, geographic location, cost, relationship status and the attitudes and training of those employed by home care agencies, assisted living communities and nursing homes.
Aging in place may be the best way to guarantee autonomy and privacy for both single and coupled members of the LGBTQ community and, in turn, avoid barriers to the expression of their gender and sexuality. A variety of factors, however, may place this option out of reach for many older LGBTQs including the costs and the lack of access to informal care. Although acceptance and support for those who are LGBTQ has been increasing, LGBTQ older adults continue to experience discrimination from professionals and organizations whose mission is to help with challenges associated with aging. This may undermine efforts to age in place and to continue freely expressing one’s gender and usual sexual practices. For example, fear of mistreatment or discrimination is believed to be a major contributing factor to the finding that LGBTQ older adults are 20% less likely than their heterosexual peers to access government services such as housing assistance, meal programs, food stamps, and senior centers, all of which may be essential for remaining at home as an individual age [40, 41].
LGBTQ older adults are also less likely than heterosexual adults to have children to help them and may also be estranged from family members or continue to conceal their sexual orientation due to fears of rejection [42]. For many older LGBTQ adults, living with a family member may either severely limit opportunities for sexual intimacy or not be an option.
With relatively few exceptions, residential care and nursing home environments severely limit the sexual and gender expression of older LGBTQ adults. The fear and anxiety that LGBT older adults experience regarding health care often intensify when circumstances require a move to a group living or nursing home [43, 44]. The majority of older LGBTQ adults believe health care providers in retirement communities would discriminate against them based on their sexual orientation [45]. Published research studies have documented incidents of conflict, abuse, and ostracism of LGBTQ older adults in residential living environments due to displays of same-sex affection or simply the recognition by other residents or staff that the individual belongs to gender and/or sexual minority [43, 44, 46]. These concerns lead older lesbians and gay men to delay moving to residential care [47]. A recent literature review of long-term care communities and LGBTQ residents suggests a comprehensive environmental assessment (assessing patient, staff, and community knowledge/attitudes) and staff training to promote optimal care of LGBTQ individuals [48]. Over the past decade, a number of low-income senior housing communities, such as Triangle Square in Los Angeles and the John C. Anderson Apartments in Philadelphia, have been established specifically for members of the LGBTQ community to address these concerns [49].
In the future, a more detailed and accurate understanding of the sexuality of the LGBTQ population may be possible through developments such as 1) increasing inclusion of questions about sexual orientation and gender identity in future large scale surveys and 2) the anticipated increasing comfort among LGBTQ individuals, especially those who are older, with self-disclosure of sexual minority status and/or gender identity in various health care and research setting.

Sexuality in Older Adults with Cognitive Impairment
While sexual interest and activity persist across the lifespan, factors such as partner status, comorbid chronic medical illness, mental illness, physical or functional impairment, and cognitive impairment can affect sexual expression in older adults [50- 52]. This section examines the impact of cognitive impairment on sexuality in older adults.
Cognitive impairment may affect the frequency of and satisfaction with sexual activity. Less than 25% of married individuals with mild to moderate cognitive impairment continue to engage in sexual activity [53]. Up to 70% of caregivers of individuals with possible or probable Alzheimer’s disease report indifference to sexual activity in their partners [54]. The prefrontal cortex is involved in various aspects of sexual functioning including executive function, abstract thinking, sense of self and others, and judgment. Memory and emotional factors are also integral to intact sexual behavior [10]. A 2014 systematic review found an overall trend toward diminished sexual behavior with cognitive decline and impairment [10]. Cognitive functioning influences the perception of sexuality. Hartmans et al. examined cognitive domains including memory, fluid intelligence, processing speed, and general cognitive functioning as measured by the Mini-Mental State Examination. Results showed an association between perceiving sexuality as unimportant and lower general cognitive functioning and fluid intelligence [51]. Other outcome measures associated with cognitive impairment include perceiving sexual activity as unpleasant and disagreeing with a continued need for intimacy with aging [51]. Despite these findings, sexual interest remains for many cognitively impaired older adults, and healthcare providers should be aware of potential barriers to healthy sexual expression.
An issue encountered in cognitively impaired individuals is that of capacity to consent to sexual activity. Intact decision-making capacity involves four abilities: understanding of relevant information, appreciation of the situation, ability to reason and rationally manipulate the information, and communication of choice [55]. Different levels of capacity may be required based on the activity and severity of potential consequences, and some have argued that decisions about sexual activity or type of sexual activity may require less stringent adherence to the above criteria [56, 57]. Like other decisions, the capacity to consent to sexual activity can change over time, especially with progressive cognitive decline. Unlike some medical decisions, decisions regarding sexual activity are often made privately and can change in the spur of the moment, posing additional challenges for sexual capacity assessments [58].
An approach to assessing sexual consent capacity employs a three-step process utilizing an interdisciplinary treatment team including the patient, physicians, psychologists, social workers, physical and occupational therapists, nursing staff, and family members. The first step involves cognitive screening with follow-up cognitive testing as indicated, focusing particularly on executive functioning. Evidence of impairment on testing does not automatically imply a lack of capacity. A semi-structured interview follows to assess knowledge, reasoning, and voluntary nature of the choice to engage in sexual activity. Knowledge assessments evaluate the patient’s awareness of types of sexual activity and associated risks. Reasoning includes the patient’s ability to process and make decisions about sex, as well as awareness of how a partner might consent or decline sexual activity. The clinician should also ensure that the decision to engage in sexual activity is voluntary and free from coercion or exploitation [58]. If it is determined that the individual lacks sexual consent capacity but displays continued interest in sexual activity, a surrogate decision-maker may be necessary. In the event that the surrogate decision-maker is the spouse or potential sexual partner, conflict of interest may necessitate an alternative surrogate. Of note, some jurisdictions prohibit substituted judgment for sexual activity in incapacitated individuals [57, 59]. Lastly, once the patient assessment is complete, input from the treatment team is essential to evaluate for physical or functional limitations to sexual activity, as well as any behaviors suggestive of coercion. The overall goal is to balance the individual’s autonomy against a duty to protect based on cognitive vulnerabilities [58].
Similar to older LGBTQ individuals, long-term care communities are another potential barrier to sexual activity in older cognitively impaired adults. Two significant barriers in this setting are lack of privacy and staff bias against sexual expression [60]. A 2016 survey found that more than half of nursing home residents engage in sexual activity [61]. Lack of privacy can arise from factors including shared rooms, policies requiring doors to be unlocked, and staff failing to knock or await approval prior to entering a resident’s room [62]. Policies requiring family or physician approval for sexual activity can further heighten feelings of privacy loss and embarrassment for the nursing home resident. Lester et al. found more than half of nursing homes surveyed required approval from family or another designated representative for a cognitively impaired resident to engage in sexual activity (versus 12% requiring approval for cognitively intact residents). Approximately 10% of nursing homes surveyed required a physician order to approve or restrict sexual activity [62]. Privacy can improve with the use of “Do Not Disturb” signs and careful scheduling to increase access to activities outside of the room for roommates [61]. Patriot’s Place, a memory care unit in the Veteran’s Affairs Maine Healthcare System Community Living Center, makes use of a guest suite for family members called the “Family Room.” This room can be reserved by a resident’s significant other and allows for private intimate time with loved ones [63].
Staff biases and negative attitudes about sexuality in older adults impact sexual expression in long-term care settings. A 2015 literature review found almost one-third of clinicians and two-thirds of nursing home administrators espoused discouraging genital contact between cognitively impaired residents [64]. Once made aware of sexual contact, another study found that almost 70% of staff indicated that they would report the incident to a supervisor, 32% would respond with disgust, 27% would ignore the incident, and 20% would panic. Almost all survey respondents indicated that they would notify family
members of sexual activity [62]. These negative and often paternalistic attitudes can be combated with increased staff training. The Staff Attitudes about Intimacy and Dementia (SAID) survey is a 20-item instrument that can help identify staff knowledge and attitudes about intimacy, sexuality, and decision-making capacity in cognitively impaired residents. Utilization of such tools can help identify areas for further training to increase staff sensitivity, promote knowledge on healthy sexual expression, and distinguish inappropriate behaviors that may require additional clinical interventions [52].

Inappropriate Sexual Behaviors in Dementia
ISB can cause significant distress to an individual with dementia, their caregivers, their family members, and their victims and families [12]. These behaviors lead to embarrassment and social isolation of the individual with dementia. Additionally, the individual may be admitted to a psychiatric hospital or be moved from their residence to a supervised setting like an assisted living facility or skilled nursing facility. Furthermore, these behaviors can result in emotional or physical trauma and medical complications such as infections to the victim, the perpetrator of ISB, or both individuals. These behaviors can often result in legal charges and a significant financial burden to the perpetrator of the behaviors and their families.
Available evidence indicates that ISB is seen in 7% to 25% of individuals with dementia [12]. Although the exact sex ratios are not available, it is estimated that these behaviors are more common among men when compared to women with dementia. Among individuals with dementia, the common ISB noted include sexual talk, sexual acts, and implied sexual acts [65].
The neurobiology of ISB involves four areas of the brain, which in turn influence the type of ISB exhibited by an individual with dementia [66]. These areas include the frontal lobes, the temporal-limbic system, the striatum, and the hypothalamus.
Assessment of individuals with ISB starts with a thorough history that is obtained from the individual, their caregivers, and also their medical providers [12, 67, 68]. A targeted physical examination is then done to rule out underlying medical or neurological conditions that cause or aggravate the ISB. This is usually followed by appropriate laboratory workup to rule out medical or neurological conditions and medication
review to identify agents that may cause or worsen ISB. Additionally, standardized rating scales and/or a neuropsychological examination is completed to rule out the extent and severity of cognitive impairment, the underlying psychopathology, and personality structure that may be causing the ISB.
Despite the lack of availability of high-quality evidence, available data indicates efficacy for both pharmacological and non-pharmacological treatment modalities in the management of ISBs [12, 66-69]. In addition, combining the two treatment modalities appears to have a synergistic effect in the management of ISBs.
Useful non-pharmacological treatment strategies include the provision of supportive psychotherapy for individuals with ISB and their significant others, behavioral modification strategies including redirection, distraction, and minimizing environmental cues that may precipitate ISB [12, 66, 68]. For those who tend to expose themselves or masturbate in public, clothing modifications such as jumpsuits or clothing with zippers in the back have been found to be helpful. For those who misinterpret environmental cues as being sexual in nature and exhibit ISB, providing easily understandable explanations and gentle reminders that their responses are inappropriate and unacceptable may be helpful.
Educating caregivers is an important tool in reducing the occurrence of ISB [12, 66]. Caregivers are often in a dilemma as they want to provide appropriate care of individuals with ISBs but want to feel safe while providing care. Suitable sex-education programs for caregivers can enable them to foster appropriate outlets for normal sexual expression while preventing ISB, thus promoting a sense of safety for the patient and caregiver alike.
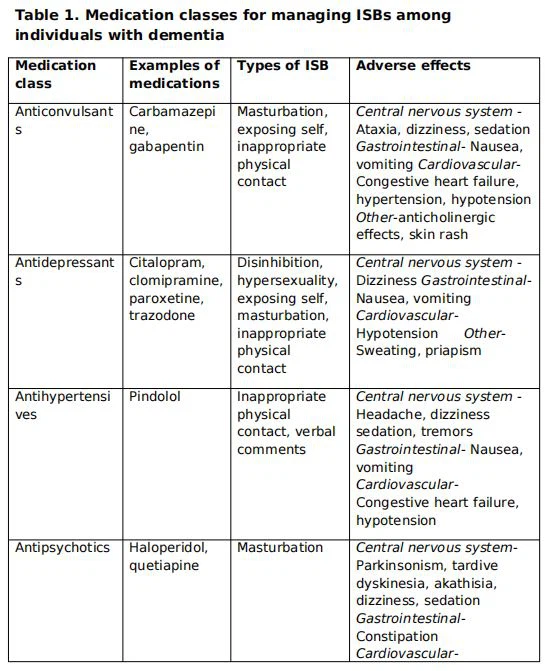
Pharmacological management strategies that have shown benefit in the treatment of ISB among individuals with dementia include anticonvulsants, antidepressants, antihypertensives, antipsychotics, cognition sparing agents, H2 receptor blockers,s and hormonal agents [12, 66-69]. There are no double-blind placebo-controlled trials for any of these medication classes for ISB. As a general rule, medications should only be used if non-pharmacologic interventions are initiated and are unsuccessful. It is prudent to follow the general rule of “start low and go slow” when prescribing psychotropic agents to older adults especially to individuals with dementia. Treatment-emergent adverse effects should be carefully monitored. Medications that can precipitate or exacerbate ISBs should be minimized or discontinued. Table 1 lists medication classes that have shown benefit in managing ISB among individuals with dementia [12, 66-69].
The use of hormonal agents for the management of ISB among individuals with dementia is a very sensitive issue [12]. The potential inability of an individual with dementia-related ISB to provide informed consent for the use of hormonal agents is a contentious topic. In addition, the side-effect profile of the hormonal agents and social stigma associated with using these drugs as their use is deemed as “chemical castration” must be handled with sensitivity and openness. Frank's discussion with an individual’s caregivers and family members about the possible benefits and risks of hormonal agents is a good first step in resolving contentious issues. The use of hormonal agents should be reserved for the management of ISB that have failed to respond to other treatment modalities.
In summary, ISB is a group of fairly common and extremely distressing behaviors that are seen among individuals with dementia. Although limited, there is emerging data on the epidemiology, neurobiology, assessment, and treatments for ISB in dementia. New research on ISB is focused not only on the appropriate management of these behaviors but also on early identification and prevention.

Conclusion
Although physiologic and psychosocial factors impact sexual expression, sexuality remains integral to the quality of life for many older adults. Healthcare providers must consider sex and gender diversity as well as multifactorial sexuality constructs with aging to become better equipped to address components such as sexual expression, sexual dysfunction, sexual identity and stigma, cognitive impairment, and capacity to consent, and at times, sexually inappropriate behaviors. Recognizing and ameliorating potential barriers to healthy sexual expression can improve the quality of life for older adults and their loved ones.
References:
1. Gewirtz-Meydan A, Hafford-Litchfield T, Benyamini Y, Phelan A, Jackson J, Ayalon L. Ageism and Sexuality. In: Ayalon L., Tesch- Römer C. (editors) Contemporary Perspectives on Ageism. International Perspectives on Aging, vol 19. Springer, Cham; 2018
2. Koh S, Sewell DD. Sexual functions in older adults. Am J Geriatr Psychiatry. 2015:23(3):223-6. doi: 10.1016/j.jagp.2014.12.002
3. Wada M, Clarke LH, Rozanova J. Constructions of sexuality in later life: Analyses of Canadian magazine and newspaper portrayals of online dating. J Aging Stud. 2015: 1(32):40-9. doi: 10.1016/j.jaging.2014.12.002
4.ll DeLamater J, Koepsel E. Relationships and sexual expression in later life: a biopsychosocial perspective. Sexual and Relationship Therapy. 2015:30(1):37-59. DOI: 10.1080/14681994.2014.939506 This article reviews biopsychosocial constructs of sexuality in older adults.
5. l Sinkovic M, Towler L. Sexual aging: a systematic review of qualitative research on the sexuality and sexual health of older adults. Qual Health Res. 2018:1049732318819834. DOI: 10.1177/1049732318819834 This article provides a systematic review of qualitative research on sexuality in older adults.
6. Hafford-Letchfield, T. What’s love got to do with it? Developing supportive practices for the expression of sexuality, sexual identity, and the intimacy needs of older people. Journal of Care ServicesnManagement 2008:2(4): 389–405. doi.org/10.1179/csm.2008.2.4.389
7. Lindau ST, Gavrilova N. Sex, health, and years of sexually active life gained due to good health: evidence from two US population-based cross-sectional surveys of aging. BMJ. 2010:10;340:c810. doi: 10.1136/BMJ.c810
8.Lochlainn MN, Kenney RA. Sexual activity and aging. J Am Med Dir Association
9.Gott M, Hinchliff S, Galena E. General practitioner attitudes to discussing sexual health issues with older people. Soc Sci Med 2004:58: 2093e2103
10. Hartmans C, Comijs H, Jonker C. Cognitive functioning and its influence on sexual behavior in normal aging and dementia. Int J Geriatr Psychiatry. 2014:29: 441-446. •• This literature review examines the association between cognitive status and sexual activity.
11. Hajjar RR, Kamel HK. Sexuality in the nursing home, part 1: attitudes and barriers to sexual expression. J Am Med Dir Assoc 2003:4(3):152-6.
12.llBlack B, Muralee S, Tampi RR. Inappropriate sexual behaviors in dementia. J Geriatr Psychiatry Neurol. 2005:18(3):155-62. This article provides an in-depth review of ISBs in dementia.
13.Lindau ST, Laumann EO, Levinson W, Waite LJ. Synthesis of scientific disciplines in pursuit of health: The interactive biopsychosocial model. Perspect Biol Med. 2003:46(3 Suppl): S74.
14. Wang V, Depp CA, Ceglowski J, Thompson WK, Rock D, Jeste DV. Sexual health and function in later life: a population-based study of 606 older adults with a partner. Am J Geriatr Psychiatry. 2015:23(3):227-33. doi: 10.1016/j.jagp.2014.03.006
15. Bell S, Reissuing ED, Henry LA, VanZuylen H. Sexual activity after 60: A systematic review of associated factors. Sex Med Rev. 2017:5(1):52-80.
16.Gledhill S, Schweitzer RD. Sexual desire, erectile dysfunction and the biomedicalization of sex in older heterosexual men. J Adv Nurs. 2014:70(4):894-903. doi: 10.1111/Jan.12256
17. Byers ES, Rehman US. Sexual well-being. In Tolman DL, Diamond LM, Bauermeister JA, George WH, Pflaus JG, Ward LM, editors. APA handbook of sexuality and psychology. Washington, DC, US: American Psychological Association; 2014.
18.Schwartz P, Velotta N. Gender and Sexuality in Aging. In Risman BJ, Froyum CM, Scarborough WJ, editors. Handbook of the Sociology of Gender. Springer, Cham.; 2018 doi.org/10.1007/978-3-319- 76333-0
19.ll Lindau ST, Schumm LP, Laumann EO, Levinson W, O'muircheartaigh CA, Waite LJ. A study of sexuality and health among older adults in the United States. New Engl J Med. 2007:357(8):762-74. This classic study examines sexual activities, behavior, and sexual problems among US community-dwelling older adults using data from NSHAP.
20.Palacios‐Ceña D, Carrasco‐Garrido P, Hernández‐Barrera V, Alonso‐Blanco C, Jiménez‐García R, Fernández‐de‐las‐Peñas C. Sexual behaviors among older adults in Spain: Results from a population‐based national sexual health survey. J Sex Med. 2012:9(1):121-9. doi: 10.1111/j.1743-6109.2011.02511






