AKI Diagnosis, What Can Urine Formed Component Testing Give?
Jul 12, 2023
Acute kidney injury (AKI) is one of the disease states affecting the structure and function of the kidney, characterized by an acute decline in renal function. AKI is a clinical syndrome caused by a variety of different etiologies, including acute tubular necrosis (ATN), acute interstitial nephritis, acute glomerular and vascular nephropathy, prerenal azotemia, and acute postrenal Obstructive nephropathy [1]. Currently, the criteria for the diagnosis and severity staging of AKI are based on changes in serum creatinine (SCr) and urine output, but in the absence of extensive clinical history, volume assessment, and/or knowledge of renal imaging, only these indicators AKI cannot be reliably distinguished. For example, in prerenal azotemia and acute tubular injury (ATI), a trial-and-error approach with intravenous fluids or diuretics is often used to further elucidate the etiology [2]. An early differential diagnosis of AKI will facilitate preventive measures to avoid further renal injury and potentially initiate early treatment to prevent renal failure. Studies have shown that urine-formed component detection can improve the accuracy of AKI diagnosis and the ability to differential diagnosis.
Click to cistanche deserticola vs tubulosa for kidney disease
Perazella et al[3] enrolled 267 patients with AKI and assessed the etiology of AKI at two-time points: (1) before urine microscopic diagnosis (initial diagnosis) and (2) patients were discharged or died (final diagnosis), patients were divided according to the evaluation Three categories: (1) ATN (2) prerenal AKI (3) others, and with the final diagnosis as the gold standard, a urinary sediment scoring system based on casts and renal tubular epithelial cells (RTEC) was established (Table 1). Differential diagnostic ability of this scoring system for AKI types.
The results of the study showed that: ATN OR value increased with the scoring system score (compared with score 0, score 1: OR 9.7, 95% CI 5.3-18.6; score ≥2: OR 74.0, 95% CI 16.6-329.1. In patients with a high probability of ATN before detection (initially diagnosed with ATN), any granular cast or RTEC (score ≥2) showed very high positive predictive value (PPV, 100%) and low negative predictive value for final diagnosis of ATN (NPV, 44%). Among patients with a low probability of ATN before detection (initial diagnosis of prerenal AKI), the absence of granular casts or RTEC had a sensitivity and specificity of 0.73 and 0.75 for the final diagnosis of ATN, respectively, with an NPV of 91 %.

Studies have shown that the urinary sediment scoring system has a high predictive value for the final diagnosis of ATN. When the constructed urine scoring system score ≥ 2 is a strong predictor of ATN.
Numerous studies have shown that low filtered sodium excretion fraction (FENa<1%) is considered consistent with prerenal azotemia and rules out acute tubular injury (ATI), however, these early studies ruled out chronic kidney disease (CKD), acute glomerular disease, urinary tract obstruction, or those receiving diuretic therapy [4,5]. And some studies have shown that FENa is not ideal in distinguishing prerenal azotemia from ATI [6]. Studies have shown that the appearance of mud brown casts (MBGC) is highly suggestive of ATI[7,8]. In clinical practice, there is often a discrepancy between the results of urine sediment testing and FENa, so is there a lack of consistency between the presence of FENa and MBGC? What is the relationship between the two for the differential diagnosis ability of ATI?
Varghese et al. [9] included 270 patients with AKI and determined the percentage of MBGC and FENa in low-power field of view (LPFs) for each sample. Calculate the Cohen K coefficient to evaluate the consistency of "the existence of MBGC" and "FENa≥1%" in diagnosing ATI, the number of detected cases of each MBGC abundance, and the number of detected cases of FENa<1% in MBGC patients with each abundance is shown in figure 1. Based on this, the estimated Cohen's K coefficient is 0.2 (0.08-0.3, 95% CI), so the ability of FENa and MBGC to diagnose ATI is comparable, but when the analysis is based on the presence of CKD in AKI, the MBGC abundance > 0%, ≥10% and ≥50% of patients, FENa<1% patients accounted for 38%, 33% and 46%, respectively, for these patients, the agreement between FENa and MBGC in diagnosing ATI was poor (the estimated Cohen K coefficient was - 0.11);
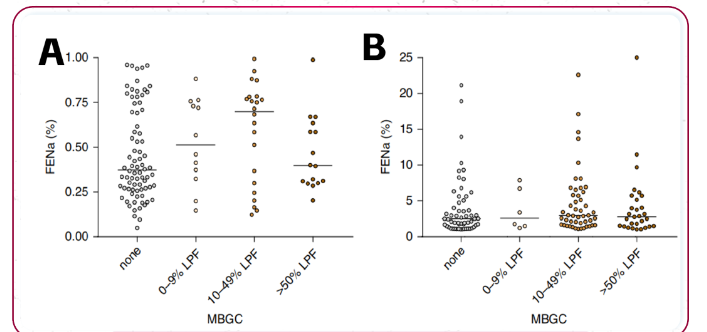
In addition, the study also conducted a one-way analysis of variance to test the relationship between MBGC abundance and 0% ≤ FENa < 1% and FENa ≥ 1%. There was no significant relationship between all and MBGC abundance (Fig. 2);
Using kidney biopsy as the gold standard, the performance of mud brown casts or FENa in the diagnosis of ATI was evaluated: sensitivity, specificity, positive predictive value (PPV), and negative predictive value (NPV). Renal biopsy was performed in 49 of the included cases, 28 of whom had MBGC, and all 28 (100%) MBGC patients were confirmed to be ATI by histopathology. Among patients without MBGC, eight (38%) had evidence of ATI on histopathology. Thus, the sensitivity, specificity, PPV, and NPV of MBGC for identification of biopsy-confirmed ATI were 78%, 100%, 100%, and 62%, respectively. Of the 28 patients with biopsies containing MBGC, 21 patients had FENa ≥ 1%, and 7 patients < 1%, so the sensitivity, specificity, PPV, and NPV of FENa for identifying ATI confirmed by renal biopsy were 90%, 71%, 90%, and 71%. The sensitivity, specificity, PPV, and NPV of combining FENa≥1% and MBGC to identify ATI were 94%, 100%, 100%, and 84%, respectively.

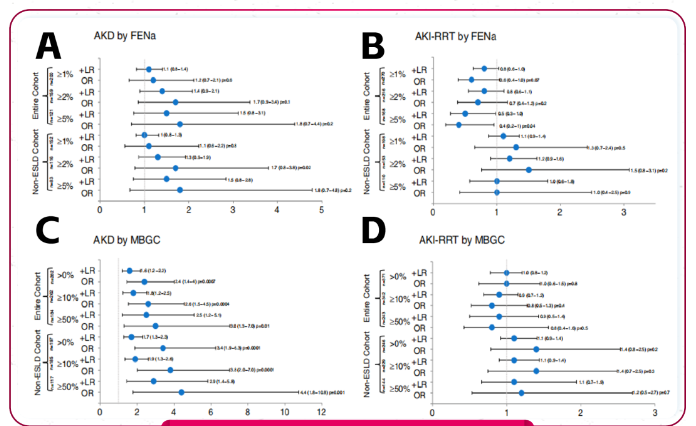
Two clinical prognostic values of MBGC were evaluated simultaneously: (1) 50% increase in serum creatinine (sCr) from baseline at discharge (acute kidney disease, AKD); (2) need for acute dialysis during hospitalization (AKI, need for renal replacement therapy[ AKI-RRT]). The evaluation was performed by calculating the odds ratio (OR) and positive likelihood ratio (+LR). For the evaluation of the prognostic predictive ability of MBGC, 371 patients were included, of which 68% had subsequent AKD and 37% required AKI-RRT. The presence of MBGC suggested a greater probability of AKD at discharge, whereas FENa ≥ 1% was not associated with the outcome. In addition, MBGC and FENa≥1% were not related to AKI-RRT. When ESLD patients were deleted, the OR value and positive likelihood ratio of MBGC for predicting AKD increased, while FENa≥1% was still uncorrelated (Figure 3). In terms of predicting AKI-RRT, MBGC and FENa≥1% were still unrelated. Combining FENa ≥ 5% and MBGC ≥ 50% LPFs compared with the above two single indicators, the ability to predict AKI-RRT is still not significant, and the ability to predict AKD is not as good as the single indicator MBGC.
In conclusion, the presence of MBGC confirmed by renal biopsy was consistent with ATI and predictive of AKD. These data suggest that the diagnosis of exclusion for ATI cannot rely solely on low filtered sodium exclusion fraction FENa, and urine-formed component testing should be used for the diagnosis of AKI.
How does Cistanche treat kidney disease?
Cistanche is a traditional Chinese herbal medicine used for centuries to treat various health conditions, including kidney disease. It is derived from the dried stems of Cistanche deserticola, a plant native to the deserts of China and Mongolia. The main active components of cistanche are phenylethanoid glycosides, echinacoside, and acteoside, which have been found to have beneficial effects on kidney health.
Kidney disease, also known as renal disease, refers to a condition in which the kidneys are not functioning properly. This can result in a buildup of waste products and toxins in the body, leading to various symptoms and complications. Cistanche may help treat kidney disease ase through several mechanisms.
Firstly, cistanche has been found to have diuretic properties, meaning it can increase urine production and help eliminate waste products from the body. This can help relieve the burden on the kidneys and prevent the buildup of toxins. By promoting diuresis, cistanche may also help Reduce high blood pressure, a common complication of kidney disease.

Moreover, cistanche has been shown to have antioxidant effects. Oxidative stress, caused by an imbalance between the production of free radicals and the body's antioxidant defenses, plays a key role in the progression of kidney disease. ies help neutralize free radicals and reduce Oxidative stress, thereby protecting the kidneys from damage. The phenylethanoid glycosides found in cistanche have been particularly effective in scavenging free radicals and inhibiting lipid peroxidation.
Additionally, cistanche has been found to have anti-inflammatory effects. Inflammation is another key factor in the development and progression of kidney disease. Cistanche's anti-inflammatory properties help reduce the production of pro-inflammatory cytokines and inhibit the activation of inflammation mandatory pathways, thus alleviating inflammation in the kidneys.
Furthermore, cistanche has been shown to have immunomodulatory effects. In kidney disease, the immune system can be dysregulated, leading to excessive inflammation and tissue damage. Cistanche helps regulate the immune response by modulating the production and activity of immune cells, such as T cells and macrophages. This immune regulation helps reduce inflammation and prevent further damage to the kidneys.
Moreover, cistanche has been found to improve renal function by promoting the regeneration of renal tubes with cells. Renal tubular epithelial cells play a crucial role in the filtration and reabsorption of waste products and electrolytes. In kidney disease, these cells can be damaged, leading to damaged renal function. Cistanche's ability to promote the regeneration of these cells helps restore proper renal function and improve overall kidney health.

In addition to these direct effects on the kidneys, cistanche has been found to have beneficial effects on other organs and systems in the body. This holistic approach to health is particularly important in kidney disease, as the condition often affects multiple organs and systems. che has been shown to have protective effects on the liver, heart, and blood vessels, which are commonly affected by kidney disease. By promoting the health of these organs, cistanche helps improve overall kidney function and prevent further complications.
In conclusion, cistanche is a traditional Chinese herbal medicine used for centuries to treat kidney disease. Its active components have diuretic, antioxidant, anti-inflammatory, immunomodulatory, and regenerative effects, which help improve renal function and protect the kidneys from further damage. , cistanche has beneficial effects on other organs and systems, making it a holistic approach to treating kidney disease.






