Review Of Traditional Chinese Medicine In The Treatment Of Benign Prostatic Hyperplasia
May 14, 2026
Abstract
This paper reviews and analyzes the literature on traditional Chinese medicine (TCM) for benign prostatic hyperplasia (BPH) over the past decade. TCM therapies-including oral herbal decoctions, acupuncture, moxibustion, tuina massage, and comprehensive interventions-show definite clinical efficacy. They significantly relieve patients' clinical symptoms and improve objective laboratory indices. This review summarizes therapeutic effects, identifies limitations in recent TCM research for BPH, and proposes future research priorities and directions.
Keywords: urinary retention; benign prostatic hyperplasia; acupuncture; moxibustion; tuina massage; TCM herb for prostate health

1. Introduction
Benign prostatic hyperplasia (BPH), commonly called prostate enlargement, involves abnormal overgrowth of prostate tissue leading to increased prostate volume. An enlarged prostate does not always cause symptoms; however, when it compresses the urethra and bladder neck and restricts urinary flow, it triggers difficult urination, frequent nighttime urination and other discomforts. In severe cases, it can lead to urinary retention, hydronephrosis, urinary tract infection, and renal impairment, severely reducing quality of life.
BPH affects more than 50% of middle‑aged men, and prevalence rises with age: approximately 70% in men aged 60–70 and up to 90% in those over 80.
Modern management of BPH relies mainly on surgery and pharmaceuticals, but outcomes vary widely and have clear limitations:
Surgical treatment carries high risk, multiple contraindications, and a notable recurrence rate.
Oral medications show inconsistent efficacy and frequent adverse reactions.
By contrast, TCM offers diverse, well‑tolerated, and clinically effective approaches for BPH and is widely used in clinical practice. This retrospective analysis of TCM for BPH aims to provide new strategies and research insights for clinical diagnosis and treatment.
2. TCM Disease Classification of BPH
BPH is a modern medical term and not directly named in ancient TCM texts, but its clinical manifestations match descriptions of long bi (urinary retention), lin syndrome (stranguria), and jing long (prostatic stagnation) in classical Chinese medical literature.
The earliest record appears in Huangdi Neijing (The Yellow Emperor's Internal Classic):
"One with long bi urinates dozens of times a day; this is due to deficiency."
"When middle qi is insufficient, urinary and bowel functions change."
Later scholars further clarified:
Bi: gradual onset, dribbling urine, frequent voiding
Long: acute anuria, complete urinary blockage
In TCM, BPH is treated mainly as long bi, with core patterns including:
damp‑heat accumulation
blood stasis obstruction
liver qi stagnation
spleen‑kidney qi deficiency
kidney‑yang insufficiency
TCM treatment follows the principle: formula follows pattern, method follows pathogenesis-rooted in clear understanding of etiology and mechanism.
3. TCM Etiology and Pathogenesis of BPH
BPH occurs mostly in men over 50. Its location is the genital chamber (prostate), closely related to the kidney, sanjiao, and bladder.
Classical TCM states:
"Disease of long bi is due to evil damaging the kidney."
"Sanjiao: excess causes long bi; deficiency causes enuresis."
"Bladder disease leads to urinary blockage; unsmooth bladder causes bi; uncontrolled bladder causes enuresis."
The core pathogenesis of BPH is:
Root deficiency: aging‑related spleen‑kidney depletion, kidney qi insufficiency, sanjiao qi transformation failure, bladder opening‑closing dysfunction
Excess in the branch: concurrent damp‑heat, blood stasis, and qi stagnation
Thus, BPH is a typical root‑deficiency and branch‑excess disorder.
4. TCM Treatment Principles for BPH
TCM treats BPH based on pattern differentiation:
Deficiency: tonify
Excess: drain
Mixed deficiency‑excess: tonify the root and eliminate the branch
Main principles:
Tonify deficiency: focus on tonifying the kidney to balance yin and yang, restore bladder control
Expel excess: prioritize regulating drainage in line with the idea "six fu‑organs function by unobstruction"
For deficiency: tonify spleen and kidney, warm kidney yang, activate qi to unblock waterways
For excess: activate blood, resolve stasis, clear damp‑heat, warm and transform phlegm
5. TCM Clinical Therapies for BPH
5.1 Oral TCM Herbal Therapy
5.1.1 Spleen‑Kidney Qi Deficiency
Jianpi Bushen Huoxue Decoction (30 cases)
Ingredients: Huangqi, Dangshen, Baizhu, Shudihuang, Shanyao, Shanzhuyu, Yizhiren, Fuling, Chenpi, Tubiechong, Rougui, Zhebeimu, Chuanniuxi, Wangbuliuxing, Taoren
Result: total effective rate 90.00%
Yishen Tonglong Formula (61 cases)
Result: total effective rate 98.36%
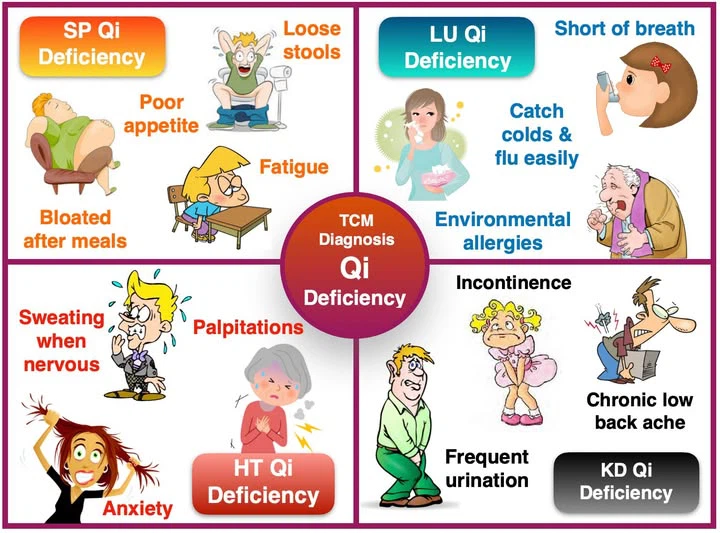
5.1.2 Kidney‑Yang Deficiency
Jinkui Shenqi Pill modified + acupoint application (50 cases)
Significantly improved IPSS, QOL, OABSS, Qmax, and residual urine volume
Remarkably higher response rate than Western medicine alone
Guifu Tongluo Decoction (38 cases)
Total effective rate 84.21%
Yanghe Sanleng Decoction (50 cases)
Total effective rate 94%
5.1.3 Kidney‑Yin Deficiency
Ziyin Tongbi Decoction (30 cases)
Improves symptoms, urinary flow rate, residual urine, and prostate volume
Total effective rate 86.67%
5.1.4 Damp‑Heat Accumulation
Shumitong Capsules (80 cases)
Total effective rate 87.5%, significantly better than the control
Qingli Tonglin Huayu Decoction (80 cases)
Total effective rate 81.5%
5.1.5 Kidney Deficiency with Blood Stasis
Guiyi Tonglong Formula (36 cases)
Superior to tamsulosin in improving urodynamic and inflammatory indices
Bushen Xiaolong Decoction (50 cases)
Significantly better IPSS, QOL, Qmax, residual urine, and TCM symptom scores
5.2 External TCM Therapies
5.2.1 Herbal Retention Enema
Custom herbal enema formulas (120 cases)
Clear damp‑heat, cool blood, resolve stasis, unblock the orifices
Total effective rate up to 94%
Special Spec Cistanche tubulosa Tablets | 500mg | 60 Count | Minimum 40% Echinacoside + 16% Acetoside (Verbascoside) | Improving Prostate Promote health| Physical Strength and Energy | Promotes Vitality

Supportive Service Of Wecistanche-For more details about cooperation
Email:wallence.suen@wecistanche.com
5.2.2 Moxibustion
Salt‑separated moxibustion (Shenque, Guanyuan, Zhongji, etc.): total effective rate 91.11%
Herbal cake moxibustion on Du meridian: superior to tamsulosin for kidney deficiency + blood stasis
Du moxibustion: total effective rate 91.4% for elderly kidney‑yang deficiency
Abdominal cake moxibustion: total effective rate 90.9%, low recurrence
5.2.3 Sitz Bath, Fumigation, and Massage
Herbal sitz bath + self‑designed Yixian Decoction: total effective rate 88.89%Local prostate massage + herbal sitz bath: total effective rate 97.5%
5.3 Comprehensive TCM Therapy
Herbs + acupuncture + anal lifting exercise: better efficacy than herbs alone
Warm acupuncture + Yishen Huayu Formula: total effective rate 91.9% vs. 70.3% in the control
All regimens improve:
IPSS (International Prostate Symptom Score)
QOL (Quality of Life)
Qmax (peak urinary flow rate)
Residual urine volume
Prostate volume
PSA and hormone balance
6. Cistanche tubulosa: A Premium TCM Herb for Prostate Health
Why Cistanche tubulosa Stands Out
We are Chengdu Wecistanche Bio‑Tech Co., Ltd., the world's largest manufacturer specializing in Cistanche tubulosa extract with a full industrial chain:

200,000‑mu standardized plantation base
GMP‑certified production workshop
15,000‑ton fresh herb storage capacity
Advanced ultrafiltration and nanofiltration purification technology
Our Cistanche tubulosa extract has far higher active content than ordinary Cistanche:
Echinacoside ≥ 25%–32%
Acteoside ≥ 9%–12%
Total phenylethanol glycosides ≥ 60%–75%
Cistanche Benefits for BPH & Male Health
Scientific research (PubMed‑supported) confirms:
Potent anti‑inflammatory & antioxidantInhibits TNF‑α, IL‑6, and oxidative stress; relieves prostate swelling and pelvic discomfort.→ TCM herb for frequent urination & pelvic pain
Improves urinary functionTonifies kidney qi, smoothes bladder function, reduces frequent nighttime urination, weak stream, and incomplete emptying.→ TCM herb for weak urine flow & nocturia
Supports male hormone balanceUpregulates StAR, CYP11A1, CYP17A1, and HSD17β3 to enhance testosterone synthesis.→ TCM herb for low energy & low libido
Enhances sperm quality & fertilityImproves sperm count, motility, and morphology; reduces abnormal forms.→ TCM herb for male fertility support
Safe for long‑term useGentle on digestion, no notable side effects-ideal for daily prostate maintenance.
Suitable For
Men 35+ with BPH‑related urinary discomforts
Those with frequent nighttime urination, slow flow, dribbling
Men concerned about prostate health, energy, and vitality
7. Summary and Outlook
BPH prevalence is rising with global aging. TCM has recognized and treated this condition for more than 2,000 years with stable efficacy, good safety, and diverse modalities.
Current limitations:
Insufficient basic research
Small sample sizes
Lack of large‑scale multi‑center trials
No unified TCM protocol
Future directions:
High‑quality evidence‑based research
Standardized TCM herbal formulas
Precision pattern differentiation
Development of high‑potency botanical extracts such as Cistanche tubulosa
Premium Cistanche tubulosa extract-with its high echinacoside and acteoside content-represents a modern, science‑backed evolution of TCM for prostate health, male vitality, and urinary comfort.
References
[1] Chen ZX. Practical Andrology. 2nd ed. Beijing: People's Military Medical Press, 2013:65
[2] Chtourou M, Ben Younes A, Binous MY, et al. J Endourol, 2001,15(8):851‑853.
[3] Zhang CH, Yang HZ. Journal of Yunnan College of Traditional Chinese Medicine, 2011,34(4):55‑57.
[4] Zhang CD, Wang ZL. Hunan Journal of Traditional Chinese Medicine, 2020,36(10):46‑48.
[5] He YM, Sheng T, Shao H, et al. Zhejiang Journal of Traditional Chinese Medicine, 2023,58(11):800‑802.
[6] He GH, Zheng J, Lai XX. Journal of Chinese Medicinal Materials, 2021,44(10):2460‑2463.
[7] Gao B, Xiao YY, Wang SJ. Inner Mongolia Journal of Traditional Chinese Medicine, 2010,29(10):6‑7.
[8] Liu TY, Li J, Shen YB, et al. Shaanxi Journal of Traditional Chinese Medicine, 2018,39(12):1712‑1714.
[9] Zhang T, Song CS. Shaanxi Journal of Traditional Chinese Medicine, 2009,30(5):570‑571.
[10] Liu JB, Yuan WD. Gansu Journal of Traditional Chinese Medicine, 2003,16(9):25‑26.
[11] Zhang CH, Bai QM, Li YF, et al. Yunnan Journal of Traditional Chinese Medicine and Materia Medica, 2020,41(4):46‑50.
[12] Ye AN, Xu JN. Hunan Guiding Journal of Traditional Chinese Medicine and Pharmacy, 1999,5(8):25‑26.
[13] Guo J, Wang F, Yang JT, et al. Chinese Journal of Integrated Traditional and Western Medicine, 2023,43(4):429‑434.
[14] Han L, Zhang XR, Liu QY, et al. Modern Journal of Integrated Traditional Chinese and Western Medicine, 2019,28(30):3362‑3365.
[15] Tao ZL, Huang XR, Duan LY. Xinjiang Journal of Traditional Chinese Medicine, 2012,30(2):34‑35.
[16] Feng JM. Inner Mongolia Journal of Traditional Chinese Medicine, 2018,37(2):90‑91.
[17] Chen XL. Heilongjiang Medical Journal, 2023,36(4):968‑971.
[18] Cao YM, Liang JZ, Li XY, et al. Hebei Journal of Traditional Chinese Medicine, 2023,38(3):25‑28.
[19] Dong Y, Xue L, Wu RZ, et al. Hebei Journal of Traditional Chinese Medicine, 2021,36(3):28‑32.
[20] Wang N, Fang JL, Zhang CY. Chinese Acupuncture & Moxibustion, 2022,42(1):83‑84.
[21] Guo Q, Li MC, Li X, et al. Journal of Practical Traditional Chinese Medicine, 2016,32(9):865‑866.
[22] Wang LX, Zhou J, Shi MX. Henan Traditional Chinese Medicine, 2015,35(11):2803‑2805.
[23] Liu YC, Zhao HX, Liu GW. Shanghai Journal of Acupuncture and Moxibustion, 2022,41(1):5‑9
[24] Zhang LZ, Lv C. Shanghai Journal of Acupuncture and Moxibustion, 2019,38(7):762‑766.






