What Can Cistanche Do in Elderly Acute Kidney Injury?
Mar 11, 2022
Acute Kidney Injury in the Elderly: Predisposition to Chronic Kidney Disease and Vice Versa
Fore information:ali.ma@wecistanche.com
Keywords: chronic kidney disease, acute kidney injury, end-stage renal disease, kidney
Abstract
There have been considerable advances in the past few years in our understanding of how chronic kidney disease predisposes to acute kidney injury and vice versa. This review shows, however, that few studies have focused on the elderly or conducted stratified analysis by age. It does appear that elderly patients with an estimated glomerular filtration rate (eGFR) 45–59 ml/min/1.73 m2 are at higher risk for acute kidney injury compared with their counterparts with eGFR 1 60 ml/min/1.73 m2. This is a similar relationship to that seen in younger patients, although the effect size appears smaller. As the incidence of acute kidney injury has been increasing over the past several years, the proportion of elderly patients surviving after acute kidney injury has also been increasing. Since acute kidney injury heightens the risk for the development and acceleration of chronic kidney disease, this implies significant public health concerns about the absolute number of elderly persons developing incident chronic kidney disease.

Click to Cistanche benefits and side effects to protect kidneys.
Introduction
Acute kidney injury is particularly common among the elderly [1]. Pre-existing chronic kidney disease is arguably the strongest risk factor for acute kidney injury [2]. Here, we review the recent literature on the relationship between acute kidney injury and chronic kidney disease in elderly patients.
chronic kidney disease and Predisposition to acute kidney injury
There has been considerable debate recently about the definition of ‘chronic kidney disease’ in elderly patients [see Winearls and Glassock, pp. c2–c4 this issue]. Doubts
have been raised whether an estimated glomerular filtration rate (eGFR) cutoff of 60 ml/min/1.73 m2 is appropriate to define chronic kidney disease in all segments of the population, especially among the elderly, since there is a natural age-associated decline in renal function [3]. To inform this debate, one major thrust of active research in the chronic kidney disease field is to better define the association between levels of eGFR and clinical outcomes [4]. To address the issue of chronic kidney disease classification in the elderly, numerous papers have examined outcomes such as cardiovascular disease events (e.g. myocardial infarction or congestive heart failure) and mortality in age-stratified analyses [5–7].
However, until recently, no published study examined acute kidney injury as an outcome, even though a strong argument can be made that acute kidney injury compared to cardiovascular disease is more directly linked pathophysiologically to chronic kidney disease. Therefore, any observed association between chronic kidney disease and acute kidney injury is less likely to be due to confounding than analogous associations between chronic kidney disease and cardiovascular disease [8].

A 2008 paper by Hsu et al. [2] quantified how the risk of dialysis-requiring acute kidney injury varied by the severity of preexisting chronic kidney disease among a large cohort of patients receiving usual medical care in a Northern California integrated health care delivery system. That study found that an increase in the risk of acute kidney injury becomes apparent starting below an eGFRof 60 ml/min/1.73 m2. Even subjects with an eGFR 45–59 ml/min/1.73 m2 have on average a two-fold increase in the adjusted odds ratio of acute kidney injury compared with subjects with an eGFR of 60 ml/min/1.73 m2 or above – with the risk being higher among subjects with diabetes than among those without ( fig. 1 ). These data support the National Kidney Foundation Chronic Kidney Disease Guidelines in which persons with eGFRs chronically below 60 ml/min/1.73 m2 are classified as having chronic kidney disease, regardless of other factors. Further age stratification analyses showed that the adjusted odds ratio was 2.73 (95% CI 2.12–3.51;p 0.0001) for those aged ^ 65 years, comparing patients with eGFR 45–59 ml/min/1.73 m2 with their counterparts with eGFR 6 60 ml/min/1.73 m2; for patients aged 1 65 years, the corresponding adjusted odds ratio was 1.33 (95% CI 1.08–1.64; p = 0.008) [unpubl. data].
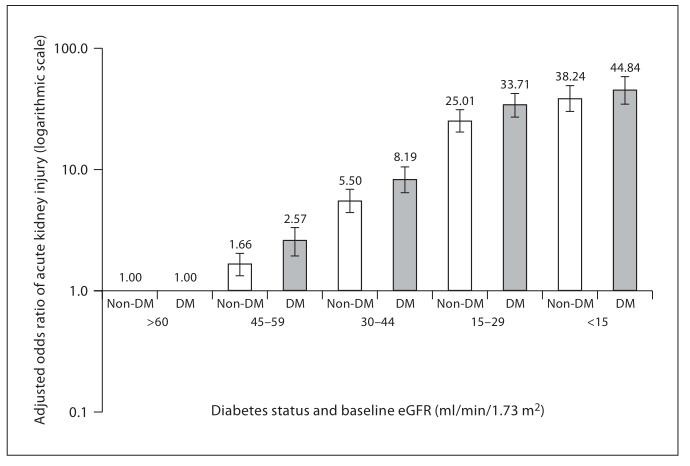

A recent publication by Grams et al. [9] using data from the Atherosclerosis Risk in Communities (ARIC) Study obtained similar results. For example, the adjusted risk of acute kidney injury approximately doubled going from an eGFR of 60 to 45 ml/min/1.73 m2. Interestingly, Grams et al., who used the chronic kidney disease-EPI equation [10] to explore higher eGFR levels, reported that compared with those with eGFR 75 ml/min/1.73 m2, relative hazards for acute kidney injury was nearly doubled in ARIC participants with eGFR of 60 ml/min/1.73 m2. This is a stronger and earlier signal than that seen in numerous studies of eGFR and death or cardiovascular disease – where in some instances risk may not rise appreciably until eGFR is below 45 ml/min/1.73 m2 [11–13]. This argues that the NKF threshold of an eGFR of 60 ml/min/1.73 m2 may be too conservative in some clinical settings such as acute kidney injury. No age-stratified eGFR analysis was presented by Grams et al. [9].In addition to a low eGFR, the other main manifestation of chronic kidney disease is proteinuria and the importance of proteinuria in the classification of chronic kidney disease has received much attention recently. Hsu et al. [2] first reported that proteinuria is an important independent risk factor for acute kidney injury. Patients with documented dipstick proteinuria appear to be 2–3 times as likely as patients without it to develop acute kidney injury, independent of eGFR. Grams et al. [9] further quantified a
graded relationship between the severity of proteinuria (albuminuria) and the risk of acute kidney injury. With participants who had urine albumin-to-creatinine ratios 10 mg/g as a reference, the adjusted hazards ratios of acute kidney injury were 1.9, 2.2, and 4.8 for urine albumin-to-creatinine ratio groups of 11–29, 30–299, and 6 300 mg/g, respectively. Age-stratified analysis showed that the associations between crude rates of acute kidney injury and severity of baseline albuminuria were similar in those above or below age 65 years ( fig. 2 ).

Several other recent studies have also concluded that proteinuria is a risk factor for acute kidney injury in the setting of cardiac catheterization [14], cardiac surgery [15], and the general population [16]. But no comparisons of older and younger patients were reported.
acute kidney injury and Predisposition to chronic kidney disease
A plethora of data over the past several years, both from experimental studies in animals and from human studies, indicates that acute kidney injury does not infrequently lead to chronic kidney disease.
In experimental animals, a robust fibrotic response in the kidney is apparent several days to weeks after a single episode of acute kidney injury induced by ischemia-reperfusion injury
[17, 18] . This fibrotic response is enhanced by older age [19]. The primary mediator of this relationship is multi-factorial, implicating microvascular damage [17], increased sensitivity to angiotensin II [20], and upregulation of genes associated with inflammation, remodeling, and fibrosis [21, 22]. In aged mice, the expression of zinc-2-glycoprotein may influence the exaggerated fibrotic response [19]. A significant manifestation of the post-acute kidney injury phenotype is salt-sensitive hypertension [23, 24].
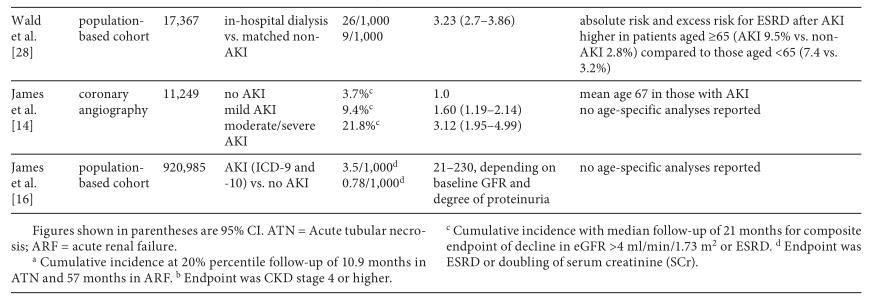
The preponderance of evidence from epidemiologic studies supports the notion that acute kidney injury leads to chronic kidney disease in elderly persons. First, older age is associated with a greater chance of nonrecovery of renal function back to baseline after acute kidney injury by the time of hospital discharge [25]. Second, several studies have demonstrated that even after adjustment for several important covariates, acute kidney injury is independently associated with an increased risk for both chronic kidney disease and end-stage renal disease ( table 1 ). In elderly patients, the risk for the end-stage renal disease after a single episode of acute kidney injury is elevated 2-fold in those with mild acute kidney injury [26], and elevated by 3- to 13-fold in those with more severe acute kidney injury [16, 26–28]. The annual absolute risk for developing the end-stage renal disease is approximately 0.6–1.2% after mild acute kidney injury [14, 26], but 1.7–2.9% after severe acute kidney injury [14, 26–28]. The annualized risk of end-stage renal disease increases to 7–9% if the acute kidney injury occurs in an individual with a preexisting history of chronic kidney disease [16, 27, 28]. The relative risk for end-stage renal disease may [28] or may not [27] be higher in those of older age (vs. younger age) after acute kidney injury. If the latter is true (lower relative risk of end-stage renal disease with older age vs. younger age), the effect is likely confounded by the competing risk of death.

End-stage renal disease only represents the most severe manifestation of chronic kidney disease. Less severe stages of chronic kidney disease are still associated with a markedly increased risk of cardiovascular disease, poorer quality of life, and increased health care costs [11]. The incidence rate of chronic kidney disease (stage 4 or worse) is approximately 120 per 1,000 person-years after non-dialysis-requiring acute kidney injury [29] and 479 per 1,000 person-years in those who required dialysis for acute kidney injury [30]. These absolute incidence rates are commensurate with adjusted hazard ratios of at least 4 for non-dialysis-requiring acute kidney injury and 28 for dialysis-requiring acute kidney injury (compared to no acute kidney injury, respectively) [29, 30].
In a recent study examining the rate of eGFR decline in patients undergoing cardiac catheterization, James et al. [14] demonstrated that the rate of decline in eGFR was 1.0 ml/min/1.73 m2 per year after mild acute kidney injury and 2.8 ml/min/1.73 m2 per year after moderate or severe acute kidney injury (compared with 0.1 ml/min/1.73 m2 per year in those without acute kidney injury). Although these rates were adjusted for age (along with proteinuria and comorbidities), it is unclear whether older age was associated with a more rapid decline of eGFR, as would be hypothesized based on data from experimental animals. Factors that modify the effects of the relationship between acute kidney injury and progressive chronic kidney disease are the level of baseline renal function and degree of proteinuria [16]. The risk for progressive chronic kidney disease attributable to acute kidney injury is attenuated with lower levels of baseline eGFR and higher levels of proteinuria.

About public health, approximately 40 million people in the US are aged 6 65 in 2010. Since the incidence of acute kidney injury in this elderly population is approximately 3,000 per 100,000 person-years [1] and 75% will survive to discharge after acute kidney injury, and the incidence of stage 4 or worse chronic kidney disease after acute kidney injury is approximately 120 per 1,000 person-years [estimated from Kaplan-Meier curve in figure 3 of reference 29] then approximately 100,000 elderly persons per year in the United States are developing new chronic kidney disease after an episode of acute kidney injury. The challenges for the nephrology community are to find strategies to either prevent acute kidney injury or prevent the transition from acute kidney injury to chronic kidney disease. Until these strategies are developed and proven to be effective, chronic kidney disease and end-stage renal disease after acute kidney injury in elderly patients represent a substantial public health burden.
Conclusion
In summary, elderly patients with eGFR 45–59 ml/min/1.73 m2 are at higher risk for acute kidney injury compared with their counterparts with eGFR 1 60 ml/min/1.73 m2. This is a similar relationship to that seen in younger patients, although the effect size appears smaller. As the incidence of acute kidney injury has been increasing over the past several years [1], the proportion of elderly patients surviving after acute kidney injury has also been increasing [31–33]. Since acute kidney injury heightens the risk for the development and acceleration of chronic kidney disease, this implies significant public health concerns about the absolute number of elderly persons developing incident chronic kidney disease.

Cistanche can improve kidney functions and avoid acute kidney injury, chronic kidney disease,end-stage renal disease.
References
The source is by Steven G. Coca et al, accessible online at: www.karger.com/nec






