Assessment Of Hearing And Vestibular Functions in A Post-COVID-19 Patient: A Clinical Case Study Part 1
Aug 17, 2023
Abstract: SARS-CoV-2 infection may cause such complications as post-COVID-19 syndrome, which includes chronic fatigue, myalgia, arthralgia, as well as a variety of neurological manifestations, e.g., neuropathy of small fibers, hearing and vestibular dysfunction, and cognitive impairment. This clinical case describes a 41-year-old patient suffering from post-COVID-19 syndrome and chronic fatigue syndrome. A detailed examination was performed, including an in-depth study of peripheral and central hearing and vestibular functions, as well as small nerve fiber length and density in the skin and cornea of the eye. Contrary to expectations, no peripheral nervous system dysfunction was detected, despite the presence of dizziness and gait instability in the patient. Hearing tests (gap detection test and dichotic test) showed central auditory processing disorders. The evaluated lesion in the processing of temporal and verbal auditory information can be a significant factor contributing to additional overload of neural activity and leading to chronic fatigue when performing daily activities in patients with CFS and post-COVID-19 complications.
Cistanche can act as an anti-fatigue and stamina enhancer, and experimental studies have shown that the decoction of Cistanche tubulosa could effectively protect the liver hepatocytes and endothelial cells damaged in weight-bearing swimming mice, upregulate the expression of NOS3, and promote hepatic glycogen synthesis, thus exerting anti-fatigue efficacy. Phenylethanoid glycoside-rich Cistanche tubulosa extract could significantly reduce the serum creatine kinase, lactate dehydrogenase, and lactate levels, and increase the hemoglobin (HB) and glucose levels in ICR mice, and this could play an anti-fatigue role by decreasing the muscle damage and delaying the lactic acid enrichment for energy storage in mice. Compound Cistanche Tubulosa Tablets significantly prolonged the weight-bearing swimming time, increased the hepatic glycogen reserve, and decreased the serum urea level after exercise in mice, showing its anti-fatigue effect. The decoction of Cistanchis can improve endurance and accelerate the elimination of fatigue in exercising mice, and can also reduce the elevation of serum creatine kinase after load exercise and keep the ultrastructure of skeletal muscle of mice normal after exercise, which indicates that it has the effects of enhancing physical strength and anti-fatigue. Cistanchis also significantly prolonged the survival time of nitrite-poisoned mice and enhanced the tolerance against hypoxia and fatigue.

Click on Fatigue Causes
【For more info:george.deng@wecistanche.com / WhatApp:8613632399501】
Keywords: post-COVID-19 syndrome; autoimmunity; hearing loss; hearing tests; vestibular tests; gap detection test; dichotic test
1. Introduction
In 2020, the world faced a pandemic of COVID-19 infection, which not only led to a dramatic increase in the number of patients suffering from viral pneumonia and respiratory failure but also to the evaluation of a significant number of complications, known as a post-covid syndrome [1,2]. In 2021, the World Health Organization introduced the Delphi consensus, where the criteria for this syndrome were described, allowing medical specialists to work with “post-COVID-19 condition” (U09.9) as a diagnosis [3]. The criteria for this syndrome specified the presence of symptoms for at least 2 months after the onset of the disease. The typical complaints included, among others, chronic fatigue, sub-febrile hyperthermia, cognitive impairment, arthralgia, and myalgia. Autonomic nervous system dysfunction was also frequently described. [1–4].
Many symptoms of post-COVID-19 syndrome reminded medical specialists of those in chronic fatigue syndrome (CFS/ME) [5,6]. CFS/ME is a disease of unknown etiology, characterized by an increase in physical and mental fatigue, which persists after rest and is accompanied by a variety of autonomic symptoms [7]. Up to 70% of CFS patients note the presence of infectious triggers, predominantly viral etiology, associated with SARS-CoV-2 and Herpesviridae spp., followed by the progression of immunologic and autonomic complications [8,9]. In the pathogenesis of CFS/ME, neuroimmune, endocrine, and metabolic disorders are also described, however, the exact pathophysiologic mechanisms remain sufficiently understudied [7–11].
The immunological profile of post-COVID-19 syndrome and CFS/ME includes impairment in the cytokine profile and immunoglobulin concentration, T- and B-cell activation, and a decrease in the cytotoxicity of the natural killer cells [12]. The presence of various autoantibodies has been described, in particular, antinuclear, antiphospholipid, antiganglioside antibodies, and antibodies to neurotransmitters and their receptors, mainly to β-1 and β-2 adrenergic receptors and M3 and M4 acetylcholine receptors [13–15]. A recent study has shown the immunologic response to the neural tissue autoantigens in post-COVID-19 patients as well as serological similarities between this condition and antiphospholipid syndrome [13].
One of the possible causes of the multiple and widespread symptoms in post-COVID-19 and CFS patients is considered to be small fiber neuropathy [16,17]. This polyneuropathy of autoimmune nature can lead to the development of dysautonomia, explaining the presence of autonomic manifestations, weakness, and cognitive impairment, along with cerebral perfusion dysfunction [18]. The evaluation of the peripheral nervous system dysfunction can lead to the objectification of diagnostic criteria for post-COVID-19 syndrome and CFS.

Hearing loss is a common manifestation in several systemic autoimmune diseases [19–21]. A primary autoimmune hearing loss is also described, with the involvement of several inner ear autoantigens (protein zero, tubulin, cochlea, inner ear supporting cell antigen, collagen type II, and, especially, heat shock protein 70) [22]. Considering the development of small fiber neuropathy in patients with CFS and post-COVID-19 syndrome, impairments of the auditory and vestibular functions are also possible and reviewed in the studies [23–25]. Taking into account that these complaints may be noted by patients themselves only when the auditory dysfunction is progressing to a mild or severe extent, hearing and vestibular studies may be an important part of the clinical investigation. Considering the frequent complaints of memory loss and attention deficit in patients with post-COVID-19 and CFS, the assessment of hearing seems to be a study that may clarify the pathophysiological mechanisms of the disease and allow the performance of a differential diagnosis. Assessment of vestibular disorders in this group of patients is required primarily to evaluate orthostatic dysfunction, which occurs in about 70% of cases [26].
2. Clinical Case Description
2.1. Patient’s Anamnesis
The patient, 41 years old, female, had complaints of constant weakness and fatigue, which did not allow her to fully perform daily routines and professional activity. She noted episodes of pyrexia up to 38.5 ◦C as a response to emotional events and stresses (average body temperature 36.9–37.3 ◦C), accompanied by flu-like symptoms. She also noted orthostatic intolerance, nausea, and vomiting, as well as sleep disturbance, attention difficulties, dizziness, and even falls in the dark and regular episodes of herpes virus infection. Those complaints intensified gradually and significantly after an episode of SARSCoV-2 infection in 2020. Given the presence of constant fatigue, as well as immunological, autonomic, and neurocognitive symptoms, the patient asked for medical help, suspecting CFS and post-COVID-19 syndrome.

Such complaints as constant fatigue and stress-associated pyrexia with flu-like symptoms the patient noted from childhood, but previously, they were episodic and had a mild severity. After COVID-19 infection and measle revaccination in December 2020, the symptoms became persistent and pronounced, worsening the patient’s daily activities. Over the past two years, she noted insomnia with early awakenings that were provoked by alcohol intake, overwork, and emotional stress. The patient also noted the presence of unsteadiness at night with periodic falls. In addition, after the SARS-CoV-2 infection, she began to notice autonomic dysregulation, manifesting with orthostatic intolerance and nausea and vomiting with an increase in systolic blood pressure above 110 mm Hg. Moreover, the recurring episodes of herpes virus infection over the last few years were evaluated. In childhood, she suffered chickenpox, mumps, frequently occurring otitis, tonsillitis, pharyngitis, as well as recurring episodes of herpes viral infection. In 2016, a papilloma of the mammary gland was evaluated. Also in 2016, she was diagnosed with hypothyroidism, and treatment with levothyroxine was prescribed. No other chronic diseases were evaluated.
2.2. Results of Clinical and Laboratory Examinations
DePaul Symptom Questionnaire (DSQ-2) [7]: CFS/ME
Immunologic studies: CMV-IgG+, VCA IgG+, EBNA IgG+.
ECG: no pathological signs revealed.
Ultrasonography of brachiocephalic vessels: signs of heterogenic influence at the extracranial level of the vertebral arteries.
Brain MRI: no pathology evaluated.
Complete blood count, blood chemistry test, urinalysis: no pathology evaluated.
Neurological consultation: Preserved cognitive functions. Cranial nerves without pathology. Muscle strength in the upper and lower extremities D = S, no pathology evaluated. Deep reflexes were symmetrical. Superficial and deep sensitivity was preserved. Stable in the Romberg position. No gait abnormalities.
2.3. Vestibular Examination
All standard neurological vestibular tests were performed with normal results.
2.4. Auditory Examination
The results of air and bone standard audiometry showed that tonal hearing was also within the normal range (Figure 1).

A slight decrease in hearing loss up to 25 dB for both ears was found only at 8 kHz stimulation. The Luscher’s test was performed at frequencies of 6 and 8 kHz, and the intensity modulation thresholds for the left and right ears were 0.8 and 1.0 dB, respectively. Since the test result was negative, no dysfunction of the suprathreshold sound was detected. Thus, the patient’s peripheral hearing condition could be assessed as an initial pathological process in the organ of Corti.
The auditory processing disorder or central auditory processing disorder was tested using several tests. The binaural fusion test-audiometry with alternating binaural speech (BNR), which, according to different authors, is highly sensitive to the lesions of the brainstem [27] and to disorders of the higher-level auditory processing centers [28], was performed by the patient successfully. She recognized 100% of monosyllabic words presented in silence to the left and right ears, and 95% of such words in binaural listening when the first half of a word was delivered to one of the ears and the second was contralateral. The obtained result was normal. During the auditory memory examination using the paced auditory serial addition test (PASAT) [29], the patient added 55 out of 60 pairs of digits heard without errors, which is equivalent to 83% correct answers. This result corresponds to the average values shown by adult subjects from the healthy controls [29].

The other two central auditory processing tests the patient performed with significant difficulties. The dichotic word listening test, which detects dysfunction in the interhemispheric connections and changes in the functioning of the corpus callosum [30], was passed by the patient with a large number of errors. There were 66% correct answers from the left ear and 81% from the right. The test revealed a significant predominance of the right ear. In the case of normal hearing, the number of correct answers in the dichotic test is not less than 90% [31]. The results of the dichotic test are shown in Figure 2. The patient was unable to reproduce all 6 words in any of the 30 auditions, and in 2 cases she did not reproduce any of the words presented to her left ear.
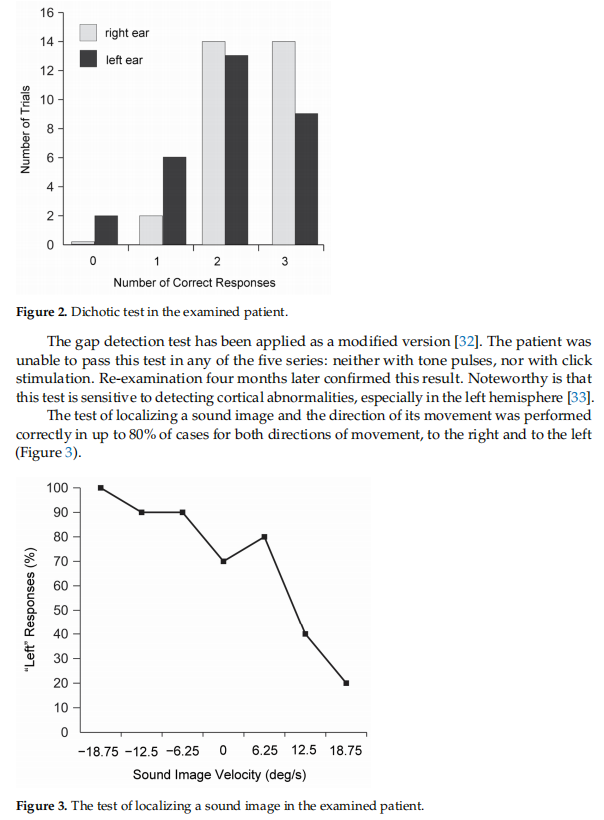
2.5. Small Fiber Neuropathy Evaluation
To study the possible presence of small fiber neuropathy in this patient, two tests were performed: a skin biopsy with the counting of the intraepidermal nerve fibers, and confocal microscopy of the cornea. The skin biopsy was taken from the lateral part of the thigh and prepared and fixed according to the standard protocol.
Intraepidermal small fiber density in the patient was 9.4 fibers per mm when the 5th percentile normal value for her age is considered to be 5.7 fibers per mm [34]. Therefore, no signs of small fiber neuropathy in the distal part of the extremity were evaluated.
To specify this result, corneal confocal microscopy was performed, where the images of the subbasal corneal plexus were obtained (Figure 4).

According to the obtained results, the density and length of the corneal nerve fibers in the patient were within normal values, though CNBD and CNFL were lower than gender- and age-corrected medians.
【For more info:george.deng@wecistanche.com / WhatApp:8613632399501】






