Minimal Change Disease Secondary To Graft-versus-Host Disease After Allogeneic Hematopoietic Cell Transplant For Myelodysplastic Syndrome
Jul 06, 2023
Abstract
Chronic graft-versus-host disease (cGVHD) is a leading cause of non-relapse mortality in allogeneic hematopoietic cell transplant (HCT) recipients. While the current standard of care is proactive in detecting cGVHD in the lungs, liver, and skin, cGVHD involving kidneys is an underrecognized and likely underdiagnosed cause of post-HCT renal dysfunction. Nephrotic syndrome (NS) is a very rare complication of HCT that is postulated to be a glomerular manifestation of cGVHD. Herein, we report 2 cases of post-HCT minimal change disease likely secondary to cGVHD. In both cases, the onset of NS coincided with the tapering of calcineurin inhibitors, and 1 patient had previously been diagnosed with cGVHD of the lungs. One patient was treated with corticosteroids alone and the other with corticosteroids and tacrolimus. Complete, sustained remission was achieved in both cases. Our cases illustrate the implications of the association between cGVHD and post-HCT NS for patient care, including the importance of obtaining a renal biopsy to establish an accurate histopathological diagnosis and guide-appropriate treatment.
Keywords
Nephrotic syndrome · Minimal change disease · Graft-versus-host disease · Kidney biopsy · Allogeneic hematopoietic cell transplant.

Click here to buy the Cistanche supplement
Introduction
Although advancements in hematopoietic cell transplants (HCTs) have significantly improved outcomes for patients with myelodysplastic syndrome (MDS) and acute leukemia, HCT still carries a substantial risk for severe posttransplant complications including relapse, opportunistic infection, and graft-versus-host disease (GVHD). While the current standard of care is proactive in recognizing the more common manifestations of GVHD in the lung, skin, and liver, atypical presentations involving other organ systems pose a greater diagnostic challenge. One example is GVHD of the kidney, an exceedingly rare and poorly understood manifestation of GVHD. Due to the paucity of reported cases, the full range of potential clinical manifestations remains to be seen, and there is no established standard of care. However, there is evidence indicating that chronic GVHD (cGVHD) may be an underdiagnosed cause of post-HCT renal dysfunction.
The list of potential causes for renal dysfunction in HCT recipients is long and includes hypovolemia, sepsis, tumor lysis syndrome, medication-induced nephrotoxicity, and GVHD. One particularly rare but potentially lethal cause of renal dysfunction in HCT recipients is nephrotic syndrome (NS). Among patients with post-HCT NS, membranous nephropathy (MN) and minimal change disease (MCD) are by far the most commonly identified histopathological subtypes; however, case reports of membranoproliferative glomerulonephritis, class III lupus nephritis, focal segmental glomerulosclerosis, and IgA nephropathy have also been published [1–4]. A growing body of evidence suggests that many cases of post-HCT NS may represent a glomerular manifestation of cGVHD. This assertion is supported by the observation that over 87% of cases of post-HCT NS occur in patients with cGVHD, along with the well-described temporal relationship between the tapering of immunosuppressive medications and the onset of NS [5, 6]. Further evidence was discovered through basic science research in murine models of cGVHD showing membranous changes, direct mesangial damage, and immune complex deposition [7–9].
The mechanism by which cGVHD leads to the development of post-HCT NS is poorly understood, and the full range of potential clinical manifestations remains to be seen. Due to the paucity of reported cases, there is no established standard of care for HCT recipients who present with signs and symptoms of NS. Herein, we present 2 cases of post-HCT MCD likely secondary to cGVHD of the kidney.

Cistanche tubulosa
Case Report/Case Presentation
Case 1
A 64-year-old male with a history of T-cell large granular lymphocyte disorder and gout was referred to the clinic for chronic leukopenia and recurrent granuloma annulare nodules on the trunk, arms, and face. Bone marrow biopsy revealed mild erythroid and megakaryocytic dysplasia with a slightly elevated blast percentage (5%) suggestive of MDS with an intermediate-risk IPSS-R score of 3.5. The patient completed three cycles of azacitidine without major adverse effects, and he subsequently underwent reduced-intensity allogeneic HCT from a matched, unrelated, female donor with a minor ABO incompatibility (O+ donor to A+ recipient). He received standard posttransplant GVDH prophylaxis with tacrolimus and methotrexate.
Seventy-three days posttransplant, the patient presented with a 1-week history of generalized weakness, fatigue, dyspnea, nonfocal abdominal pain, and nonspecific arthralgias, most prominent in the knees and ankles. Shortly thereafter, he experienced acute onset of altered mental status and aphasia, prompting CT and MRI of the brain, which showed no evidence of acute intracranial pathology. Due to concern for encephalitis, the patient was treated empirically with cefepime, azithromycin, acyclovir, and ampicillin. Three days later, he developed acute hypoxic respiratory failure which, considering his immunocompromised state, raised concern for atypical pneumonia; however, infectious pathogen panels were negative. Ultimately, a lung biopsy revealed diffuse alveolar injury consisting of an idiopathic pulmonary syndrome consistent with cGVHD. He was treated with etanercept and high-dose steroids and maintained on tacrolimus until day 211 posttransplant.
244 days posttransplant, the patient presented to the emergency department with a 1-week history of dyspnea, chills, anorexia, cough, light-headedness, and fatigue. Initial blood work was notable for profound anemia (hemoglobin 4.1 g/dL), reticulocyte count of 10%, total serum bilirubin of 3.3 g/dL, and elevated serum creatinine of 2.0 mg/dL, along with spherocytosis on peripheral blood smear. Autoagglutination and antiglobulin studies were performed due to concern for hemolysis, and the results were consistent with cold agglutinin syndrome. The patient responded well to treatment with corticosteroids, IVIG, and transfusion of 2 units of packed red blood cells, and by the day of his discharge, his hemoglobin was stable at 7.0 g/dL. After discharge, he completed an oral prednisone taper and received a total of four doses of rituximab.
280 days posttransplant, the patient again presented to the emergency department with hypertension, fatigue, and peripheral edema that were initially attributed to his glucocorticoid therapy, but quickly progressed to frank NS with anasarca, frothy urine, worsening hypertension, and a 50-lb weight gain. Serum studies revealed a creatinine of 3.3 mg/dL, blood urea nitrogen of 86 mg/dL, and serum albumin of 2.2 g/dL. Urine studies showed massive proteinuria with a spot urine protein-to-creatinine ratio of 26.13 g/g, moderate hyaline casts, and specific gravity of 1.017. Renal ultrasound showed diffuse bladder wall thickening, increased echogenicity without hydronephrosis, and a mildly enlarged prostate. A kidney biopsy was performed (Fig. 1), and electron microscopy revealed severe effacement of the podocyte foot processes with no pathologic abnormality in the proximal tubules and peritubular capillaries. Light microscopy showed normal-appearing glomeruli and no evidence of immune complex deposition on immunofluorescence staining, leading to a diagnosis of MCD.
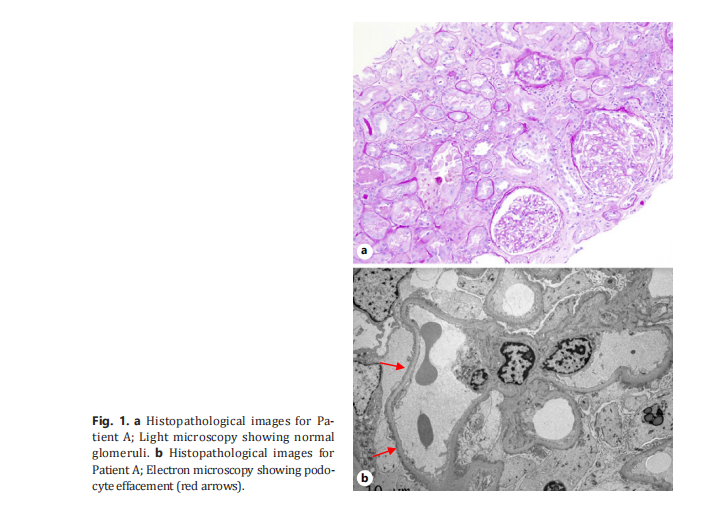
The patient was treated with diuresis and oral prednisone 1 mg/kg and restarted on tacrolimus with marked improvement in his edema. Prednisone was tapered rapidly over 3 months, per patient preference, and tacrolimus was continued for a total of 9 months. Within 3 months of starting treatment, the urine protein-to-creatinine ratio had decreased to <1 g/g. Kidney function continued to improve over the subsequent 6 months, reaching a new serum creatinine baseline of 1.6–1.9 mg/dL (estimated glomerular filtration rate 36–44 mL/ min/1.73 m2), consistent with chronic kidney disease stage III. Since the last office visit on day 680 posttransplant, the patient has experienced no further complications.

Cistanche pills
Case 2
A 65-year-old female with a history of hypertension and heart palpitations was referred to the clinic for evaluation of possible MDS discovered on a bone marrow biopsy performed as part of a workup for anemia. A review of the biopsy revealed an increased blast percentage (12%) consistent with MDS subtype EB-2 with an intermediate-risk IPSS-R score of 4. The patient tolerated 6 cycles of azacitidine without major side effects and subsequently underwent reduced-intensity conditioning allogeneic HCT from a matched, unrelated, ABO-compatible donor (R-A-/D + A+). She received standard post-transplant GVHD prophylaxis with cyclosporine and methotrexate. Her hospital course was complicated by newly diagnosed atrial fibrillation that resolved with metoprolol, and she was discharged on appropriate prophylaxis. The cyclosporine taper was started on day 135 posttransplant.
268 days posttransplant, the patient presented to the hospital with oliguria and anasarca. At the time of admission, her cyclosporine had been tapered down to 25 mg every other day, and she was on prophylaxis with TMP-SMX 160 mg 3 times a week. Laboratory on admission was notable for elevated serum creatinine (6.0 mg/dL from a baseline of 1.0 mg/dL) and massive proteinuria (spot urine protein-to-creatinine ratio 13.65 g/g). A kidney biopsy was performed (Fig. 2), and electron microscopy showed severe effacement of the podocyte foot processes with normal-appearing glomeruli on light microscopy and no complement or immunoglobulin deposits on immunofluorescence, consistent with MCD.
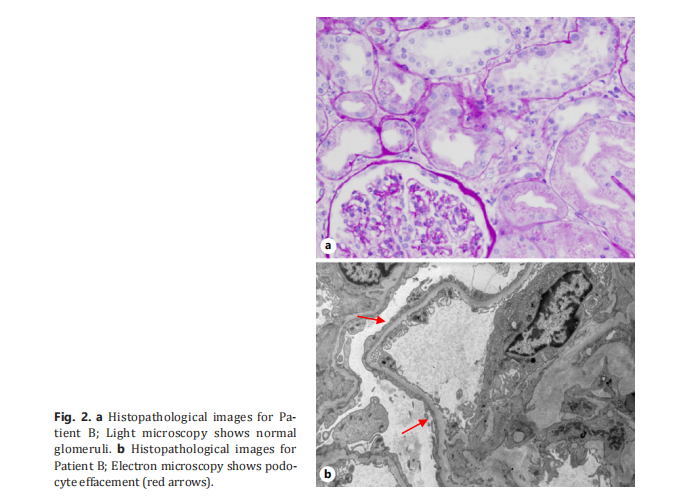
The patient underwent hemodialysis (HD) via a temporary HD catheter and was started on tacrolimus 0.5 mg twice daily and methylprednisolone 1 g/kg/day. Methylprednisolone was continued for 11 days, and tacrolimus was discontinued after 7 days due to concern for impaired kidney recovery in the acute setting due to drug-induced vasoconstriction. A tunneled dialysis catheter was placed in anticipation of long-term HD requirements. She was ultimately discharged home on prednisone 60 mg daily, with a plan to undergo HD 3 times a week. Within 1 week of discharge, the patient’s urine output and solute clearance had markedly improved, and dialysis was discontinued after a total of 6 sessions. A full prednisone taper was completed by 4 months post-discharge, with resolution of her nephrotic-range proteinuria. Approximately, 570 days posttransplant, she has not required further HD, and her serum creatinine is currently stable at 1.1 mg/dL.

Herba Cistanche
Discussion
The relationship between cGVHD and NS has significant implications for the management of post-HCT NS. The current mainstay of treatment for MCD is glucocorticoid monotherapy, which results in complete remission in 80–95 percent of cases of MCD in adults [10]. In contrast, post-HCT MCD is frequently glucocorticoid-resistant, with a response rate of approximately 22% [9]. The remaining patients require combination therapy with calcineurin inhibitors, mycophenolate mofetil, or rituximab [11–15]. Likewise, post-HCT MN tends to be resistant to glucocorticoids, with response rates comparable to those seen in idiopathic MGN, approximately 11% [9]. While the treatment regimens for MCD and MN in HCT recipients are similar, there are significant differences in the prognosis of these 2 entities. In a systematic review of 116 patients treated for post-HCT NS, patients with MCD recovered at a median of 1.75 months, while the median time to recovery for patients with MN was 7 months. Overall treatment outcomes also differed, with complete remission achieved in 81.3% of patients with MCD and 59.1% of patients with MN [9].
Considering these differences in treatment and prognosis, renal biopsy is instrumental to the management of HCT recipients who present with nephrotic-range proteinuria. However, HCT recipients are often medically complex, and renal biopsy may be underperformed in this population due to a high perceived risk of complications such as bleeding or infection. Renal biopsy should be considered in all patients in whom there is a concern for post-HCT NS and should ideally be performed before starting immunosuppressive therapy whenever possible. In patients with a clear contraindication to biopsy, an empiric trial of corticosteroids should be considered. However, given the high likelihood of corticosteroid-resistant disease, clinicians should maintain a low threshold for starting additional immunosuppressive agents. Beyar-Katz et al. [9] proposed empiric treatment with corticosteroids, close monitoring, and reassessment of proteinuria at 12–16 weeks to determine the necessity of additional immunosuppressants, although there have not been any studies investigating the efficacy of this approach. Furthermore, despite the role of long-term immunosuppression in solid organ rejection of the kidney, there is insufficient information in the literature detailing the most optimal prophylaxis for GVHD of the kidney or effective methods for the long-term treatment of cGVHD of the kidney.

Cistanche capsules
Here, we described 2 cases of post-HCT MCD favored to be caused by cGVHD of the kidney. In both cases, the onset of NS coincided with the tapering of calcineurin inhibitors, raising suspicion for GVHD as the underlying cause. Biopsy was obtained shortly after the onset of symptoms, allowing for a timely diagnosis of MCD. Both patients were started on corticosteroids and tacrolimus, although tacrolimus was discontinued after a week in patient 2, and both patients had an excellent response with sustained remission after treatment. These cases highlight the importance of the connection between cGVHD and NS, and its implications for patient care. Clinicians should be aware that cGVHD is present in most patients with post-HCT NS, the vast majority of whom will require additional immunosuppression beyond glucocorticoid monotherapy. Furthermore, renal biopsy should not be delayed unless necessary, as it is critical for ensuring an accurate diagnosis, appropriate treatment, and a more favorable outcome.
References
1 Fraile P, Pilar F, Vazquez L, Lourdes V, Caballero D, Dolores C, et al. Chronic graft-versus-host disease of the kidney in patients with allogeneic hematopoietic stem cell transplant. Eur J Haematol. 2013 Aug;91(2):129–34.
2 Kim JY, Lee MY, Kim B, Park CW, Chang YS, Chung S. Membranoproliferative glomerulonephritis following allogeneic hematopoietic stem cell transplantation. Clin Exp Nephrol. 2010 Dec;14(6):630–2.
3 Hu SL, Colvin GA, Rifai A, SuzukiH, Novak J, Esparza A, et al. Glomerulonephritis after hematopoietic cell transplantation: IgA nephropathy with increased excretion of galactose-deficient IgA1. Nephrol Dial Transplant. 2010 May;25(5):1708–13.
4 Hingorani S. Renal complications of hematopoietic-cell transplantation. N Engl J Med. 2016 Jun 9;374(23): 2256–67.
5 Brukamp K, Doyle AM, Bloom RD, Bunin N, Tomaszewski JE, Cizman B. Nephrotic syndrome after hematopoietic cell transplantation: do glomerular lesions represent renal graft-versus-host disease? Clin J Am Soc Nephrol. 2006 Jul;1(4):685–94.
6 Srinivasan R, Balow JE, Sabnis S, Lundqvist A, Igarashi T, Takahashi Y, et al. Nephrotic syndrome: an underrecognized immune-mediated complication of non-myeloablative allogeneic hematopoietic cell transplantation. Br J Haematol. 2005 Oct;131(1):74–9.
7 Padhi P, Muchayi T, Teske E, Kuperman M, Barrantes F. Minimal change disease after hematopoietic stem cell transplant: a manifestation of chronic graft-versus-host disease. J Onco-Nephrol. 2020 Feb 1;4(1–2):37–40.
8 Chu YW, Gress RE. Murine models of chronic graft-versus-host disease: insights and unresolved issues. Biol Blood Marrow Transplant. 2008 Apr;14(4):365–78.
9 Beyar-Katz O, Davila EK, Zuckerman T, Fineman R, Haddad N, Okasha D, et al. Adult nephrotic syndrome after hematopoietic stem cell transplantation: renal pathology is the best predictor of response to therapy. Biol Blood Marrow Transplant. 2016 Jun;22(6):975–81.
10 Colattur SN, Korbet SM. Long-term outcome of adult-onset idiopathic minimal change disease. Saudi J Kidney Dis Transpl. 2000 Sep;11(3):334–44.
11 Mak SK, Short CD, Mallick NP. Long-term outcome of adult-onset minimal-change nephropathy. Nephrol Dial Transplant. 1996 Nov;11(11):2192–201.
12 Black DA, Rose G, Brewer DB. Controlled trial of prednisone in adult patients with the nephrotic syndrome. Br Med J. 1970 Aug 22;3(5720):421–6.
13 Nolasco F, Cameron JS, Heywood EF, Hicks J, Ogg C, Williams DG. Adult-onset minimal change nephrotic syndrome: a long-term follow-up. Kidney Int. 1986 Jun;29(6):1215–23.
14 Rao PS. Nephrotic syndrome in patients with peripheral blood stem cell transplant. Am J Kidney Dis. 2005 Apr; 45(4):780–5.
15 Dhakal B, Singavi A, Cohen EP, Dangal M, Palmer J, Dall A, et al. Chronic GVHD and concurrent new-onset nephrotic syndrome in allogeneic transplant recipients. Incidence, pattern, and therapeutic outcomes. Bone Marrow Transplant. 2015 Mar;50(3):449–51.
Omar Elghawy 1, John S. Wang 1, Alexander C. Hafey 1, Amand 1, D. Renaghan 2 Rachel M. Whitehair 3, Tamila L. Kindwall-Keller 4,
1 School of Medicine, University of Virginia, Charlottesville, VA, USA;
2 Division of Nephrology, University of Virginia, Charlottesville, VA, USA;
3 Department of Pathology, University of Virginia, Charlottesville, VA, USA;
4 Division of Hematology and Oncology, University of Virginia, Charlottesville, VA, USA






