Part Ⅱ Capitated Versus Fee-for-service Reimbursement And Quality Of Care For Chronic Disease: A US Cross-sectional Analysis
May 17, 2023
Results
1. Patient and practice characteristics
Between 2012 to 2016, there were 41,834 unweighted visits to 3766 unique physicians for patients with hypertension, diabetes, or CKD in our study population, representing 1,091,331,663 weighted visits. In weighted analyses, about 9% (95% confidence interval [CI] 6.3–11.1%) of visits were to practices with majority capitation revenue; 76% (72.9–78.5%) were to those with majority FFS revenue, and 16% (13.6–17.5%) to practices with another reimbursement mix. Patients in our study population visiting practices with the majority capitated revenue were more likely to be Black or Hispanic, have congestive heart failure, and have Medicare as their primary payment source (Table 1). Age and sex did not statistically differ by practice reimbursement type. Patients visiting practices with majority capitated reimbursement were seen fewer times in the past 12 months (3.7 vs. 5.2 vs. 5.2, p=0.006), compared with practices with majority FFS revenue or other reimbursement mix.

Click here to get Herb Cistanche
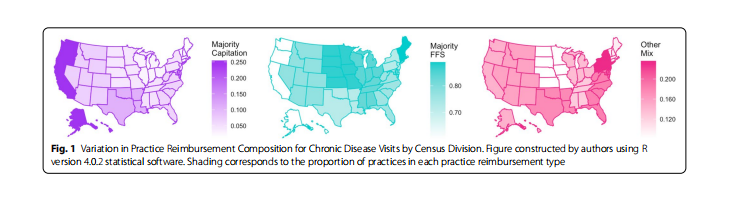
There was significant regional variation in reimbursement type for chronic disease visits (Fig. 1). Compared with FFS practices and other reimbursement practices, the majority of capitated practices were more likely to be in the West Census Region (55% vs. 18% vs. 17%, p < 0.001). Capitated practices were also less likely to be solo practices than FFS and other reimbursement mix practices (21% vs. 37% vs. 35%, p=0.005). Capitated practices were more likely to be paid with a fixed salary, rather than a share of billings (58% vs. 32% vs. 37%, p < 0.001), and more likely to be an employee or contractor (50% vs. 38% vs. 38%, p=0.004), compared with FFS and other practices. Capitated practices were more likely to be owned by an insurance company, health plan, or HMO, compared with FFS and other practices (24% vs. 13% vs. 13%, p=0.033). Capitated practices are more likely to have a majority of their practice’s patient care revenue coming from private insurance (43% vs. 25% vs. 19%, p=0.004) and managed care payments (69% vs. 23% vs. 26%, p < 0.001), compared with FFS and other practices. Patient and physician/practice characteristics did not otherwise differ across practice reimbursement types.
2. Hypertension quality indicators
The prevalence of controlled hypertension (BP < 140/90 mmHg) was similar across capitated, FFS, and other reimbursement types in unadjusted analyses (71% vs. 74% vs. 75%, Table 3). The odds of controlled hypertension in visits to capitated practices did not differ significantly from those to FFS practices in multivariable analyses adjusted for patient characteristics. In the fully adjusted model, the odds of controlled hypertension in capitated practices were not statistically significantly different than for FFS practices, adjusting for both patient and physician/practice characteristics.

3. Diabetes quality indicators
The prevalence of controlled diabetes (HbA1c <7%) was similar across capitated, FFS, and other practices in unadjusted analyses (57% vs. 59% vs. 63%, Table 3). ACEi/ ARB use among those with diabetes and hypertension was suboptimal across reimbursement types (54% vs. 50% vs. 46%). Recommended statin use was also low across capitated, FFS, and other practices (37% vs. 40% vs. 32%).
In either multivariable model, there were no statistically significant associations between reimbursement type and controlled diabetes or ACEi/ARB use, among visits for diabetes. In analyses adjusted for patient characteristics, other revenue mix practices had lower odds of statin use among visits for diabetes, compared with FFS practices (adjusted odds ratio [aOR] 0.68, 95% CI [0.50– 0.90]). When additionally adjusted for physician/practice characteristics, other revenue mix practices remained associated with lower statin use among visits for diabetes (aOR 0.69, 95% CI [0.52–0.93]), but this did not reach statistical significance when accounting for multiple comparisons.

Cistanche supplements
4. CKD quality indicators
Patient visits for CKD to majority capitated practices were less likely to have controlled hypertension (BP <130/80mmHg) in unadjusted analyses, compared with FFS or other practices (43% vs. 56% vs. 57%, Table 4). Across practice reimbursement types, the prevalence of controlled diabetes (HbA1c <7%) among patients with CKD was higher but not statistically different in capitated practices (78% vs. 59% vs. 61%). Less than half of patients with CKD were prescribed ACEi/ARBs and less than one-third were prescribed statins across reimbursement types. Prevalence of ACEi/ARB use among CKD visits was similar across capitated, FFS, and other reimbursement types (45% vs. 45% vs. 40%), and statin use was lower but not statistically different in capitated practices (21% vs. 35% vs. 31%).
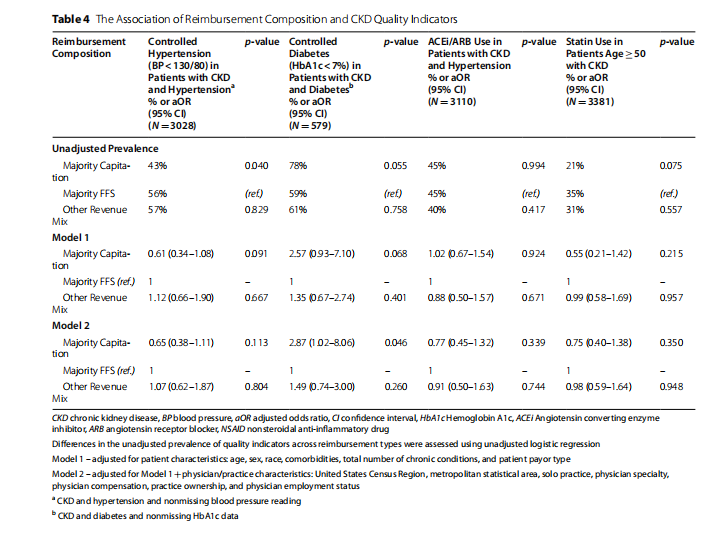
In multivariable analyses adjusted for patient characteristics, the odds of controlled hypertension, controlled diabetes, ACEi/ARB use, and statin use among patients with CKD were not statistically significantly different across practice reimbursement types. In analyses controlled for both patient and physician/practice characteristics, reimbursement type was also not associated with statistically significant differences in CKD quality indicators. In our sensitivity analyses, capitated reimbursement was not associated with statistically different odds of controlled hypertension or controlled diabetes (HbA1c <8%) in fully adjusted models.
Discussion
In this nationally representative sample of US outpatient visits, we found that about 9% of patients with chronic disease visited practices that receive the majority of their revenue from capitated payments. We also found that practices with majority capitated revenue differed significantly from FFS and other practices in patient characteristics, serving a more diverse patient population and having a reduced visit frequency (1.5 fewer visits in the past year), and in physician and practice characteristics, including their region, physician compensation, practice ownership, and payor mix. Lastly, we found that reimbursement type was not associated with consistent differences in hypertension, diabetes, or CKD quality indicators.
While the associations found in this study do not necessarily indicate causation, we found important differences in chronic disease quality of care by reimbursement type that complements prior literature. A Cochrane systematic review found only 4 studies meeting inclusion criteria with variable study settings and also found that FFS care was associated with increased visit frequency [13]. Analyses in the 1990s showed that capitation was associated with reduced utilization of laboratory tests and overall charges for patients with hypertension [27], and was not associated with adverse health status in an elderly Medicaid population [28]. On the other hand, a systematic review of 35 studies found that managed care plans, which frequently had capitation payment arrangements, had mixed effects on the quality of care, and several studies showed negative effects of managed care on enrollees with chronic conditions [29]. Another systematic review found that FFS care, compared with capitation, was associated with more patient visits and greater continuity; however, the review was limited by study heterogeneity and the low number of eligible studies [13]. More recent evidence from Canada showed that capitation compared with FFS was associated with similar quality of care for diabetes, congestive heart failure, and coronary artery disease [30], but better quality of care for hypertension [31], weight monitoring, and smoking cessation [32]. Contemporary evidence from a population-based primary care system in Hawaii demonstrated that capitated payments were associated with improvements in a Healthcare Effectiveness Data and Information Set (HEDIS) composite quality measure score, as well as a reduction in several visits [33]. Taken together, evidence from a variety of settings and disease entities does not point to an overall conclusion about the impact of capitated payments on chronic disease quality of care.
Several factors may explain these mixed findings. First, the capitation payment amount should also be considered, which may differ substantially across Medicare, Medicaid, and commercial managed care settings [34]. Second, practices are subject to different quality metrics and pay-for-performance initiatives depending on the payor arrangement, which incentivize quality of care improvements [35, 36]. Thus, the impact of not only capitation vs. FFS reimbursement type but also quality metrics and other regulatory requirements impacts the quality of care delivery and must be considered in evaluating new capitation models [37, 38].

Standardized Cistanche and Cistanche pills
A key strength of our study is that our analysis leveraged a data source with practice revenue information integrated with patient and clinical encounter information. Our results have policy implications for the upcoming new capitation models, PCF and KCC. First, our findings provide a detailed picture of patient and practice characteristics where capitation is currently implemented. Practices already familiar with capitated arrangements may more readily elect into the PCF and KCC models, and have the infrastructure in place to support practice changes. Our finding that practices with majority capitation reimbursement served more Black and Hispanic patients likely represents a greater enrollment of these patients in managed Medicaid plans. Given racial and ethnic disparities in chronic disease management, the racial/ethnic composition of majority capitation practices may influence chronic disease care, and we adjusted for this in our analyses [39, 40]. Second, our results provide baseline estimates of quality of care performance by practice reimbursement composition. The outcomes we analyzed align with hypertension and diabetes quality measures incentivized in PCF and the hypertension control measure in KCC. Notably, we found that ACEi/ ARB use and statin use were suboptimal across practice reimbursement types, and dedicated quality measures for these medications tied to financial incentives should be considered in PCF and KCC.
Future analyses should evaluate the effect of PCF and KCC model implementation on the quality and utilization of care, using quasi-experimental research designs such as differences-in-differences methods. Several important considerations for these analyses deserve mention. First, practice reimbursement is separate from physician compensation. Although PCF and KCC practices will be reimbursed with capitated payments, physicians may still be incentivized toward in-person visits if they face relative value unit (RVU) targets in tiered compensation systems. Thus, a key component of PCF and KCC evaluations will be understanding the relationships between capitated reimbursements, physician compensation structures, and care delivery [41]. Second, many population health management strategies incentivized under PCF and KCC, such as panel management or care coordination activities, will not be readily measurable from claims data. Therefore, qualitative and quantitative methodologies will be crucial to evaluate the effectiveness of care delivery changes under PCF and KCC. Third, in addition to capitated payments, PCF and KCC introduce other simultaneous co-interventions, including a focused set of quality metrics, a learning collaborative, and performance incentives, so changes in quality and utilization will not be attributable solely to capitated payments. Lastly, KCC is a Medicare-only model, and lack of participation from other payors may limit care delivery changes [11], particularly in practices with predominantly commercially insured or Medicaid populations.
There are several limitations to consider in interpreting our results. First, our assessment of hypertension control was limited to a single office BP reading, as home BP readings were not available in the dataset. We did not include more expansive measures of quality of care, such as patient-reported outcomes and healthy behaviors. Second, we identified CKD using ICD-9 and ICD-10 diagnosis codes which are insensitive for CKD [42]. Further, CKD coding sensitivity may differ by practice setting, which could bias our results. Third, our study is observational and does not exploit exogenous variation in reimbursement type, so our results may be more subject to residual confounding. Our results may have had limited power to detect statistically significant differences in chronic disease care by practice reimbursement type. Furthermore, socioeconomic status, education, and employment variables were not available in our data source, which are key determinants of chronic disease care. Also, we included free-standing office-based practices and not hospital-based outpatient practices because the National Hospital Ambulatory Medical Care Survey (NHAMCS) data releases were not available after 2011, which somewhat limits the generalizability of our findings. Lastly, we used reimbursement information at the practice-level, rather than the visit level, so were unable to know if a particular visit was paid for with capitation or FFS [7].

Cistanche extract
Conclusions
In summary, we found that a substantial subset of patients with chronic disease receive care in capitation-based settings. Capitated practices had distinctively different patient and practice characteristics when compared with FFS practices, but capitated reimbursement was not associated with consistent differences in hypertension, diabetes, and CKD quality indicators. Amidst the COVID-19 pandemic and as the US enters into demonstration projects that introduce capitated payments for primary care and CKD, it will be crucial to rigorously examine the impact of reimbursement changes on chronic disease quality of care.
References
27. Murray JP, Greenfeld S, Kaplan SH, Yano EM. Ambulatory testing for capitation and fee-for-service patients in the same practice setting: relationship to outcomes. Med Care. 1992;30(3):252-61.
28. Lurie N, Christianson J, Finch M, Moscovice I. The effects of capitation on health and functional status of the Medicaid elderly: a randomized trial. Ann Intern Med. 1994;120:506–11.
29. Miller RH, Luft HS. Does managed care lead to better or worse quality of care? Health Af. 1997;16:7–25.
30. Russell GM, Dahrouge S, Hogg W, Geneau R, Muldoon L, Tuna M. Managing chronic disease in Ontario primary care: the impact of organizational factors. Ann Fam Med. 2009;7:309–18.
31. Tu K, Cauch-Dudek K, Chen Z. Comparison of primary care physician payment models in the management of hypertension. Can Fam Physician. 2009;55:719–27.
32. Liddy C, Singh J, Hogg W, Dahrouge S, Taljaard M. Comparison of primary care models in the prevention of cardiovascular disease-a cross-sectional study. BMC Fam Pract. 2011;12:114.
33. Navathe AS, Emanuel EJ, Bond A, et al. Association between the implementation of a population-based primary care payment system and achievement of quality measures in Hawaii. Jama. 2019;322:57–68.
34. Medicare Payment Advisory Commission. MaCPaA. Managed care’s effect on outcomes.
35. Landon BE, Rosenthal MB, Normand S, Frank RG, Epstein AM. Quality monitoring and management in commercial health plans. Am J Manag Care. 2008;14:377.
36. Robinson JC, Shortell SM, Rittenhouse DR, Fernandes-Taylor S, Gillies RR, Casalino LP. Quality-based payment for medical groups and individual physicians. Inquiry. 2009;46:172–81.
37. Rundall TG, Shortell SM, Wang MC, et al. As good as it gets? Chronic care management in nine leading US physician organizations. BMJ. 2002;325:958–61.
38. Casalino L, Gillies RR, Shortell SM, et al. External incentives, information technology, and organized processes to improve health care quality for patients with chronic diseases. Jama. 2003;289:434–41.
39. Gu A, Yue Y, Desai RP, Argulian E. Racial and ethnic differences in antihypertensive medication use and blood pressure control among US adults with hypertension: the National Health and nutrition examination survey, 2003 to 2012. Circ Cardiovasc Qual Outcomes. 2017;10:e003166.
40. Smalls BL, Ritchwood TD, Bishu KG, Egede LE. Racial/ethnic differences in glycemic control in older adults with type 2 diabetes: United States 2003–2014. Int J Environ Res Public Health. 2020;17:950.
41. Quinn AE, Hemmelgarn BR, Tonelli M, et al. Association of specialist physician payment model with visit frequency, quality, and costs of care for people with chronic disease. JAMA Netw Open. 2019;2:e1914861.
42. Grams ME, Plantinga LC, Hedgeman E, et al. Validation of CKD and related conditions in existing data sets: a systematic review. Am J Kidney Dis. 2011;57:44–54.
Sri Lekha Tummalapalli 1,2,3, Michelle M. Estrella 3,4, Deanna P. Jannat‑Khah 5,6, Salomeh Keyhani 7 and Said Ibrahim 1
1. Division of Healthcare Delivery Science & Innovation, Department of Population Health Sciences, Weill Cornell Medicine, 402 East 67th Street, New York, NY 10065, USA.
2. Division of Nephrology & Hypertension, Department of Medicine, Weill Cornell Medicine, New York, NY, USA.
3. Kidney Health Research Collaborative, Department of Medicine, San Francisco Veterans Affairs Medical Center and the University of California, San Francisco, CA, USA.
4. Division of Nephrology, Department of Medicine, San Francisco Veterans Affairs Medical Center, San Francisco, CA, USA.
5. Department of Medicine, Weill Cornell Medicine, New York, NY, USA.
6. Division of Rheumatology, Hospital for Special Surgery, New York, NY, USA.
7. Division of General Internal Medicine, San Francisco Veterans Affairs Medical Center, San Francisco, CA, USA.






