Prerequisites, Barriers And Opportunities in Care For Q-fever Patients: A Delphi Study Among Healthcare Workers Part 1
Aug 25, 2023
Abstract
Background Q-fever is a zoonotic disease that can lead to illness, disability, and death. This study aimed to provide insight into the perspectives of healthcare workers (HCWs) on prerequisites, barriers, and opportunities in care for Q-fever patients.
Cistanche can act as an anti-fatigue and stamina enhancer, and experimental studies have shown that the decoction of Cistanche tubulosa could effectively protect the liver hepatocytes and endothelial cells damaged in weight-bearing swimming mice, upregulate the expression of NOS3, and promote hepatic glycogen synthesis, thus exerting anti-fatigue efficacy. Phenylethanoid glycoside-rich Cistanche tubulosa extract could significantly reduce the serum creatine kinase, lactate dehydrogenase, and lactate levels, and increase the hemoglobin (HB) and glucose levels in ICR mice, and this could play an anti-fatigue role by decreasing the muscle damage and delaying the lactic acid enrichment for energy storage in mice. Compound Cistanche Tubulosa Tablets significantly prolonged the weight-bearing swimming time, increased the hepatic glycogen reserve, and decreased the serum urea level after exercise in mice, showing its anti-fatigue effect. The decoction of Cistanchis can improve endurance and accelerate the elimination of fatigue in exercising mice, and can also reduce the elevation of serum creatine kinase after load exercise and keep the ultrastructure of skeletal muscle of mice normal after exercise, which indicates that it has the effects of enhancing physical strength and anti-fatigue. Cistanchis also significantly prolonged the survival time of nitrite-poisoned mice and enhanced the tolerance against hypoxia and fatigue.

Click on Always Tired
【For more info:george.deng@wecistanche.com / WhatApp:8613632399501】
Methods A two-round online Delphi study was conducted among 94 Dutch HCWs involved in care for Q-fever patients. The questionnaires contained questions on prerequisites for high quality, barriers and facilitators in care, knowledge of Q-fever, and optimization of care. For multiple-choice, ranking, and Likert scale questions, frequencies were reported, while for rating and numerical questions, the median and interquartile range (IQR) were reported.
Results The panel rated the care for Q-fever patients at a median score of 6/10 (IQR=2). Sufficient knowledge of Q-fever among HCWs (36%), financial compensation of care (30%), and recognition of the disease by HCWs (26%) were considered the most important prerequisites for high-quality care. A lack of knowledge was identified as the most important barrier (76%) and continuing medical education was the primary method for improving HCWs’ knowledge (76%). HCWs rated their knowledge at a median score of 8/10 (IQR=1) and the general knowledge of other HCWs at a 5/10 (IQR=2). According to HCWs, a median of eight healthcare providers (IQR=4) should be involved in the care for Q-fever fatigue syndrome (QFS), and a median of seven (IQR=5) in chronic Q-fever care.
Conclusions Ten years after the Dutch Q-fever epidemic, HCWs indicate that long-term care for Q-fever patients leaves much room for improvement. Facilitation of reported prerequisites for high-quality care, improved knowledge among HCWs, clearly defined roles and responsibilities, and guidance on how to support patients could improve the quality of care. These prerequisites may also improve care for patients with persisting symptoms due to other infectious diseases, such as COVID-19.
Keywords Q-fever; Q-fever fatigue syndrome, Chronic Q-fever, Q-fever care, Quality of care
Background
Q-fever is a zoonotic disease that is prevalent worldwide and can lead to illness, hospitalization, disability, and death [1, 2]. Q-fever is transmitted to humans by inhaling aerosols containing the Coxiella burnettii bacteria from birth by-products of domestic animals [1, 3]. Approximately 40% of Q-fever patients experience symptoms. Half of them have mild flu-like symptoms, whereas the other half experience more severe symptoms, such as high fever, pneumonia, and hepatitis [4–6].
Between 2007 and 2010, the largest Q-fever outbreak ever reported worldwide occurred in the Netherlands; estimations indicate that over 50,000 individuals were infected with Q-fever [7–9]. After the first outbreak in 2007, the annual number of notified cases rapidly rose and increased tenfold between 2007 and 2009 [7]. Public health authorities were not prepared for a large Q-fever outbreak. Only limited knowledge and evidence on the impact, control measures, identification, treatment, and care were available at the time of the outbreak [7, 10, 11].
Q-fever can lead to long-term health consequences, namely Q-fever fatigue syndrome (QFS) and chronic Q-fever [2, 4]. Recent studies estimate that QFS occurs in approximately 20% of Q-fever patients [2]. The clinical manifestation of QFS consists of fatigue persisting for at least 6 months which can be accompanied by a wide range of other symptoms, such as headache, muscle and joint pain, and mental health problems [2, 12]. In addition, an estimated 1–2% of infected patients develop chronic Q-fever, which can occur months or years after the initial infection [1, 13]. Common clinical manifestations of chronic Q-fever are endocarditis and infection of aneurysms or vascular prostheses, although the presentation varies [13]. Untreated chronic Q-fever has a high mortality rate of 60% [14].
Both chronic Q-fever and QFS have a substantial impact on the lives of patients. Reuters et al. found that even 5–9 years after acute infection, the quality of life and social functioning of patients with chronic Q-fever and QFS is significantly lower than in the general population and also significantly lower compared to patients with another chronic illness [15]. Bronner et al. support these results and found that the vast majority of patients experienced health problems 10 years after infection. Furthermore, approximately 40% stopped working permanently, and over 25% experienced problems with social participation due to their illness [16].
Bronner et al. also found that patients with QFS and chronic Q-fever consulted a median number of 6 different healthcare providers [16]. In comparison, earlier research found that patients with chronic disease in the Netherlands consult a mean of 4.5 different healthcare providers [17]. The majority of patients (75%) were satisfied with the overall quality of care for Q-fever. According to patients, the most important barriers were the lack of knowledge of healthcare workers (HCWs), not feeling heard or understood, and the lack of availability of services [16].
Currently, there is no high-quality evidence or consensus regarding the optimal treatment for QFS [2, 18]. After the large Dutch epidemic, outpatient follow-up care was given to Q-fever patients experiencing prolonged symptoms. However, there was no standardization of the postinfection care provided [10].
To improve the quality of care, insight into barriers and facilitators for the care of Q-fever patients from the perspective of HCWs is necessary. HCWs have the most practical understanding of problems surrounding Q-fever care and are ultimately the ones directly involved in efforts to improve the quality of care. These insights are not only required for improving Q-fever care but are also relevant for the care of patients who experience long-term sequelae of other infectious diseases. The recent COVID-19 pandemic highlights the global threat infectious diseases pose to public health [19]. As with Q-fever, a significant proportion of COVID patients experience persisting symptoms months to years after initial infection usually labeled long COVID or post-COVID-19 condition [20]. Te care for long COVID appears to present similar challenges as Q-fever since the clinical manifestation varies considerably and consists of a wide range of symptoms [21, 22]. Thus, insights into the barriers and facilitators of care for Q-fever can also be valuable to improve care for patients with persisting post-infection symptoms as a result of other infectious diseases, such as COVID-19.
This study aimed to identify (1) prerequisites for high-quality care for Q-fever patients according to HCWs; (2) barriers and facilitators that HCWs experience in the care for Q-fever patients; (3) how these barriers can be overcome; and (4) how care for Q-fever patients should be organized according to HCWs.
Methods
Study design
Between February and May 2019, an online two-round Delphi study was conducted among a panel of HCWs in the field of Q-fever in the Netherlands. The Delphi technique is a group facilitation technique that consists of multiple rounds of questionnaires [23]. The purpose is to systematically collect and combine opinions and judgments from a panel of experts on issues on which there is contradictory or insufficient information. Responses of experts are summarized between rounds and used to compose subsequent questionnaires. By anonymously providing information on the answers of the panel participants can consider and compare their answers to other experts [23, 24]. To the best of our knowledge, there are currently no studies on the perspectives of HCWs on Q-fever care. Due to the scarcity of previous knowledge on this topic, the Delphi technique was considered the most appropriate method. Applying this method allows for the evaluation of complex issues on which there is scarce information, like Q-fever care, and is especially useful in the explorative phases [25].

Panel participants
The expert panel participants were selected based on their role in the care of Q-fever patients. They were either directly involved in care and treated Q-fever patients or they were indirectly involved, for example through healthcare policy or Q-fever research. We invited HCWs who were members of the network of Q-support, which is a national center of expertise for Q-fever that supports and advises patients and professionals. The network of Q-support consisted of HCWs who were directly involved in Q-fever care, and most of them were working in regions with high infection rates during the Q-fever epidemic. The Principal Investigator from the Erasmus MC contacted these HCWs via email to inform them and invite them to the Delphi study. In addition, the Principal Investigator contacted HCWs, policymakers, and researchers with experience with and/ or expertise in Q-fever care that were not part of the network of Q-support from hospitals, research institutes, and national working groups, including those tasked with the development of national Q-fever guidelines. Participants received written information regarding the purpose of the study and what it entailed. They were also encouraged to invite colleagues and their network to participate. Snowball sampling was thus used to reach additional participants [26]. Online informed consent was provided by all participants before participating in the Delphi study
Questionnaires
The Delphi study took place following a large-scale survey among Q-fever patients [16]. The results from this previous study, as well as other available literature, were used as a starting point for the topics of the questionnaires. Subsequently, input and feedback from experts were collected in two phases. First, input was gathered through a meeting with representatives from Q-support and Q-uestion, which is the patient organization for Q-fever patients in the Netherlands. Second, input was gathered through a meeting with two internists and a doctoral researcher from the Radboud UMC Q-fever Center of Expertise. The Radboud UMC Q-fever Center of Expertise is a collaboration between several departments within the Radboud University Medical Center that specializes in treating patients with Q-fever.
The first round online questionnaire contained information about the study's purpose and questions on participant characteristics and experience with care for Q-fever patients, knowledge of Q-fever, satisfaction with the provided care, the most optimal care, and collaboration in care. The first round consisted of open-ended questions and multiple-choice questions. Based on the answers of the first round, a questionnaire was developed for the second round, which allowed for more detailed questions on the topics that were identified in the first round. The answers to four open questions from the first round questionnaire on (1) prerequisites for high-quality care, (2) barriers in care, (3) facilitators in care and (4) methods for knowledge improvement were coded and categorized by two independent researchers to compose ranking questions for the second round. The second round questionnaire contained information about the study purpose and consisted of ranking questions (from least important to most important), multiple choice questions, and questions with 6-point Likert scales (ranging from 1=strongly agree to 6=strongly disagree), in addition to several open questions. After one month and a maximum of four reminders, the responses were summarized. This study was executed using open-source LimeSurvey software [27].
Data analysis
Participants who completed at least the first questionnaire round were included in this study. For multiple choice questions, ranking questions, and Likert scale questions, frequencies were reported. For rating questions and numerical questions, the median and interquartile range (IQR) were reported due to the non-normal distribution of the data. To determine the association between the assessment of personal knowledge and the assessment of general knowledge of HCWs, Spearman’s correlations were used [28]. Data analyses were conducted using SPSS version 25.0 (IBM Corp., Armonk, NY, USA).

Results
In this section, we first describe the panel characteristics. Second, the current state of Q-fever care is discussed. Third, the prerequisites, barriers, and facilitators for high-quality care are presented, and one of the main barriers is discussed in more detail. Lastly, we describe how HCWs believe care for Q-fever patients should be organized.
Panel characteristics
A total of 94 HCWs in the field of Q-fever care participated in the first Delphi round, of whom 86% (n=81) participated in the second round. About half were female (53%), and the median age was 52.0. The panel consisted of a wide range of professions (Table 1). The median number of years in their profession was 15.0. The majority of the panel (63%) was directly involved in care and had treated Q-fever patients, while the remaining 37% were indirectly involved in Q-fever care. Respectively 53% and 42% of the panel had treated patients with QFS and chronic Q-fever. Medical specialists were most often the treating physician of patients with QFS and chronic Q-fever patients (70%; 81%), followed by physio- and occupational therapists (40%; 55%) and general practitioners (38%; 20%) (Additional file 1: Supplementary Table S1).
The current state of Q‑fever care
The panel rated the care for Q-fever patients in general at a median score of 6/10 (IQR=2). Researchers and policymakers rated the care highest at a 7/10 (IQR=1), medical specialists gave a median score of 6.5/10 (IQR=2), and general practitioners, physio- and occupational therapists, and other HCWs all rated the care at a 6/10 (IQR=2).

HCWs who treated patients with QFS or chronic Q-fever were also asked how satisfied they were with the care they could provide for these two patient groups. Overall, they rated their satisfaction with care at a 7/10 (IQR=2) for QFS and an 8/10 (IQR=1) for chronic Q-fever. General practitioners were least satisfied, rating it at a 5/10 (IQR=3) for QFS and a 6/10 (IQR=2) for chronic Q-fever. Medical specialists were most satisfied with their care for chronic Q-fever (8/10, IQR=1), however, they were less satisfied with their care for QFS (median=6/10, IQR=3). Physio- and occupational therapists rated their satisfaction at a 7/10 (IQR=1–2) for both QFS and chronic Q-fever.
HCWs collaborated with a median of 4 (IQR=4) healthcare providers in the care of Q-fever patients. Most of them collaborated with general practitioners (60%) and Q-support (50%). HCWs rated the collaboration with healthcare providers in the care of Q-fever patients at a median score of 7/10 (IQR=2). Across professions, medical specialists rated the collaboration highest (median=8/10 (IQR=2)), while all others rated the collaboration at a median score of 6/10 (IQR=1–2).
Prerequisites, Facilitators, and Barriers for High-quality Care for Q‑fever Patients
HCWs reported many prerequisites for high-quality care (Table 2). The most frequently mentioned were: sufficient knowledge of Q-fever among HCWs (36%), financial compensation of care (30%), and recognition of the disease by HCWs (26%).

Furthermore, five other aspects were also considered to be important by at least 20% of HCWs, including up-to-date information for HCWs, an accessible consultation structure with centers of expertise, and a multidisciplinary approach to treatment.
HCWs considered Q-support, the national center of expertise for Q-fever, and contact with other Q-fever patients the best-organized aspects of Q-fever care (62%), followed by the care delivered by centers of expertise and specialists (44%) and the Dutch QFS guideline (25%) (Additional file 1: Supplementary Table S2). The majority of HCWs (76%) who treated QFS patients were familiar with the QFS guideline that was published by the National Institute for Public Health and the Environment. However, 20% of them had not yet applied the guideline in practice. The usefulness of the guideline was rated at a median score of 8/10 (IQR=2). Although most HCWs were positive about the guideline, several mentioned that the recommendations are targeted at supporting patients, not at curing the disease. As a result, they believed current treatment recommendations for QFS to be insufficient.
According to the panel, a lack of knowledge among HCWs/the disease is not recognized (76%) was the most important barrier to high-quality care, followed by unclear/limited scientific evidence for effective treatment (55%) and diagnosis is complex/not always adequate (50%) (Table 3). The majority of the panel (76%) stated that these barriers were different for chronic Q-fever and QFS, mainly because QFS was considered to be more complex and not as defined. In addition, HCWs mentioned that treatment for chronic Q-fever is considered crucial in preventing mortality, while treatment for QFS is targeted at morbidity, resulting in different barriers.

The panel was asked whether reported barriers were easy to solve. The most important barrier, lack of knowledge among HCWs/the disease is not recognized, was considered one of the easier barriers to tackle (65%) (Fig. 1). A lack of high-quality guidelines/protocols (69%) and a lack of collaboration and consultation (66%) were also considered relatively easy to tackle. The complexity of the treatment (28%) and lack of financial compensation for care (46%) were considered the hardest barriers to tackle.

Within the Dutch healthcare system, care for a specific condition is usually paid through a diagnosis-treatment combination (DBC), meaning that health insurers pay one standard price for the entire care path, not separately for each treatment [29]. Multiple HCWs mentioned that there is not a specific DBC code for Q-fever fatigue syndrome, leading to insufficient reimbursement of care for Q-fever patients through basic insurance.
HCWs’ knowledge of Q‑fever
Sufficient knowledge of Q-fever was considered the most important prerequisite and a lack of knowledge was the most important barrier for high-quality care. The panel rated their knowledge at a median score of 8/10 (IQR=1). However, they rated the general knowledge level of other HCWs much lower (median=5/10; IQR=2) (Additional file 1: Supplementary Table S3). Although the assessment of personal knowledge did not differ between HCWs with and without experience in treating Q-fever patients, HCWs who treated Q-fever patients rated the general knowledge slightly lower than other HCWs: at a median of 5/10 (IQR=2) and 6/10 (IQR=2), respectively. The assessment of knowledge appeared to be similar across professions. All professions rated the individual knowledge level at a 7/10 or 8/10 and the general knowledge level at a 5/10 or 6/10, except physio- and occupational therapists, who rated the general knowledge level at a 4/10 (IQR=2). No observable pattern or correlation was found between the personal knowledge level and the general knowledge level of other HCWs (r=0.015; p=0.887).

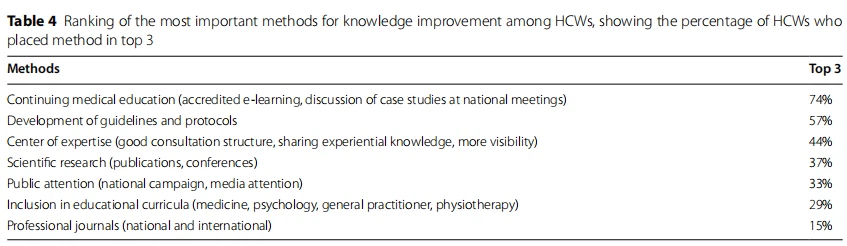
Continuing medical education (e.g. accredited e-learning, discussion of case studies) was considered the most important method for improving knowledge level (74%), followed by the development of guidelines and protocols (57%) and a good consultation structure and visibility of centers of expertise (44%) (Table 4).
Several HCWs indicated that knowledge improvement should primarily focus on creating more awareness of the long-term effects of Q-fever to achieve early diagnosis, as well as on the difference between chronic Q-fever and QFS, also in regions with lower infection rates during the epidemic, as this could lead to more timely and accurate referral of patients. As such, the majority of HCWs (82%) believed that knowledge improvement should mainly focus on primary care. HCWs mentioned that patients are usually first seen in primary care, that the lack of knowledge is most prevalent in primary care, and that many patients experience a wide variety of problems. However, others said that extensive education of primary care professionals is not useful as Q-fever is rare and that recognition of the disease is most important. In addition, several HCWs pointed out that knowledge improvement in primary care is particularly relevant for QFS, while knowledge improvement in secondary care is more important for chronic Q-fever, as diagnosis and treatment for the latter condition usually take place in secondary care.
How to care for Q‑fever should be organized
According to HCWs, care for Q-fever patients should be provided in a multidisciplinary setting. The median number of healthcare providers needed for optimal Q-fever care was 8 (IQR=4) for QFS and 7 (IQR=5) for chronic Q-fever. Most HCWs considered a general practitioner (88%), occupational physician (74%), psychologist (70%), physiotherapist (68%), Radboud UMC Q-fever Center of Expertise (61%), and Q-support (59%) needed in the care for QFS patients. In contrast, a general practitioner (78%), occupational physician (67%), internist (66%), Radboud UMC Q-fever Center of Expertise (60%), and cardiologist (51%) were deemed to be needed in the care for chronic Q-fever. HCWs advised to improve the collaboration between primary and secondary care (42%) and the collaboration between medical care and occupational care/organizations (36%) (Additional file 1: Supplementary Table S4).
HCWs mentioned the importance of having one healthcare professional who coordinates multidisciplinary care. Most of them indicated that a general practitioner (53%) or a medical specialist working in a center of expertise (30%) should have the ultimate responsibility for QFS care. For chronic Q-fever care, 45% believed a medical specialist working in a center of expertise should have this responsibility, followed by a general practitioner (28%) and a medical specialist (27%). When asked who should be in charge of the care for QFS and chronic Q-fever in an open format, several HCWs (16% for QFS; 9% for chronic Q-fever) stated that patients should be in charge of their care.
【For more info:george.deng@wecistanche.com / WhatApp:8613632399501】






