Challenges in Establishing Vaccine Induced Herd Immunity Through Age Specific Community Vaccinations
Mar 02, 2023
ABSTRACT:
Presently, the second wave of the COVID-19 pandemic is driving the world toward a devastating total failure of the healthcare system. The purpose of the review is to search for studies reporting on the implication of herd immunity in a naïve population through age-specific mass vaccination. This review is based on selected publications on the effect of herd immunity on COVID-19 in communities. We searched published scientific articles, review articles, and reports, published in 2020 as well as read some basic, cult publications related to the establishment of indirect immunity to a population. We have focused on the use of the application of vaccine-induced herd immunity in the community to confer indirect immunity against COVID-19 and searched electronic databases.
Immunity, in layman's terms, is the body's ability to resist diseases and foreign pathogenic factors. Among the factors affecting immunity, in addition to uncontrollable factors such as genetics, age, and gender, we pay more attention to controllable factors such as nutrition and lifestyle. Generally speaking, malnourished people usually have poorer immunity and a higher risk of disease infection than normal people. Therefore, improving nutritional status is the basis and guarantee for enhancing immunity. Sufficient and balanced nutrition is necessary for immune function. It is recommended In our daily diet, we should choose more protein-rich foods with high absorption rates, such as fish and shrimp, eggs, poultry, soybeans, and their products, and lean meat should be the main choice when choosing livestock meat. Try to eat less or not to eat fatty meat, bacon, sausage, and other foods. In addition, you can also eat Cistanche deserticola. The extract of Cistanche deserticola contains a variety of alkaloid substances, which have a certain inhibitory effect on the pathogenic microorganisms encountered by the human body and can effectively treat diseases. Reduce the invasion of pathogens and improve the body's resistance.

Click cistanche tubulosa extract powder product
For more information:1950477648nn@gamil.com
Science Direct by using keywords such as Herd immunity, indirect or passive immunization, Coronavirus disease 2019 (COVID-19), severe acute respiratory syndrome, coronavirus 2 (SARS-CoV-2), and immune technique. This review proposes the implication of mass vaccination-induced herd immunity in a population to curb the infection, and to every individual in a given population irrespective of their age.
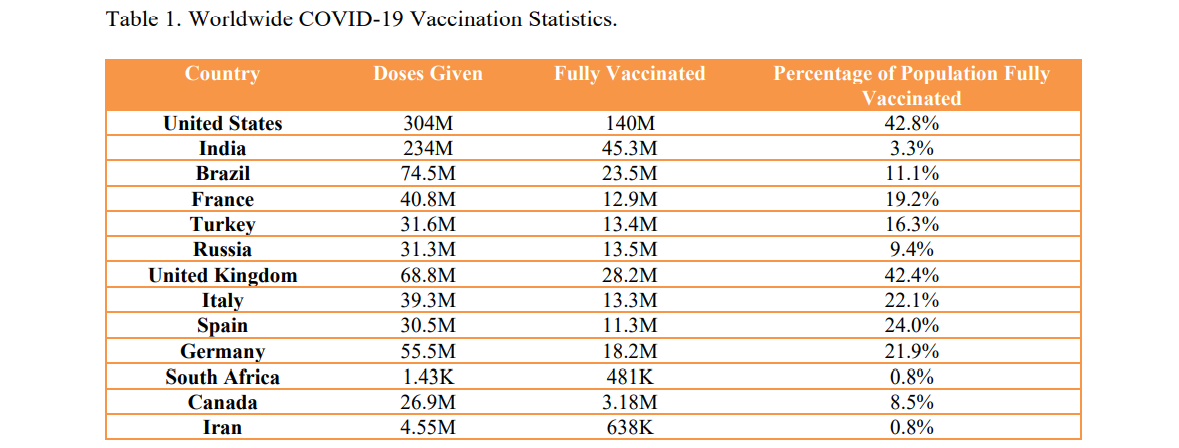
Currently, the world is faced with a new pandemic, COVID-19 disease, now together with all the ever-emerging variants of the coronavirus. The worldwide spiraling reported new cases (172,630,637 cases as of June 6, 2021) of COVID-19 posing direct challenges to public healthcare and infrastructures and is becoming a grave threat to the world's population. The situation is worsened, as the disease mode of transmission is now known to be through a vast number of asymptomatic and pre-symptomatic persons and including the emergence of new viral variants [1]. The COVID-19 disease is becoming one of the worst pandemics in the history of mankind. The worldwide overall mortality rate reached up to 4.5% as several deaths crossed 600,000 deaths out of 13 million COVID-19 cases [2]. For young adults without comorbidities, the death rate has been below 0.2% whereas, for the elderly population, the death rate due to COVID-19 is said to reach up to 15% [2]. The recovery rate varies with age, health as well as with the severity of the disease. Majority of infected patients with COVID-19 experience cough, fever, headache, loss of smell and taste, shortness of breath, and fatigue.
Severely infected patients develop acute respiratory distress syndrome (ARDS) in association with a huge cytokine storm within 2- 14 days of post-viral infection [3]. The application of corticosteroids as well as low-dose dexamethasone drugs against COVID-19 has become controversial due to their delayed renal clearance [4]. The application of Remdesivir and Lopinavir/ ritonavir against COVID-19 has generated much controversy around their efficacy and hence the use of the said has not been generally supported [5]. The Discovery of vaccines against COVID-19 is a superior achievement by advanced molecular and biological science. As of 6 th June 2021, a total of 2,121,290,083 vaccine doses have been administered to patients worldwide This review will deal not only with the chances of eradication of the disease through vaccine-induced herd immunity in a population but also with the limitations of applications of the said.
Study Design and Methodology
This review mathematically establishes the rate of success in the application of “herd immunity” in a community against COVID-19. We have gathered information from Electronic databases which includes PubMed, and Scopus. We have used keywords such as herd immunity, passive immunization, Vaccine against Covid-19, coronavirus disease 2019 (COVID-19), as well as severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2).

Vaccine-Induced Herd Immunity: The Concept
Herd immunity is an ancient concept where immunity is said to confer indirect protection to a susceptible individual against a specific pathogen in a certain population. According to the concept of herd immunity, individuals become immune either by recovering from an earlier infection or by vaccination [6]. The concept of herd immunity can only be applied to the eradication of a contagious disease, which is transmitted from one individual to another [7]. For example, Tetanus is an infectious disease but not contagious, therefore herd immunity would not work in this instance.
In a given population, a novel pathogen propagates through vulnerable individuals in an uncontrolled manner and therefore increasing the number of infected individuals. On the other hand, if any fraction of the population gets immune to that same pathogen, the probability of being infected is reduced even after close contact between vulnerable and normal individuals. For many individuals, in a naive population, becoming immune to the pathogen reduces significantly the transmission rate of the pathogen. With the spread rate of the pathogen in a naive population being reduced, the prevalence rate will subsequently decline [8]. Therefore, herd immunity protects a given population or community by suppressing the transmission of the infectious pathogen and subsequently the spread of the disease [9].
The herd immunity threshold is defined as a particular point in each population when the percentage of susceptible individuals lies below the minimum percentage of individuals needed for the successful transmission of the pathogen [10]. The percentage of the population infected when it is above the herd immunity threshold value would only be beneficial with indirect protection from pathogens [10] (Fig. 1). For an eventual gradual disappearance of a disease in a population, the herd immunity threshold should be reached [7]. This form of elimination of disease, when there is a permanent reduction of the number of infections toward zero worldwide infections, is called eradication of the disease [11].
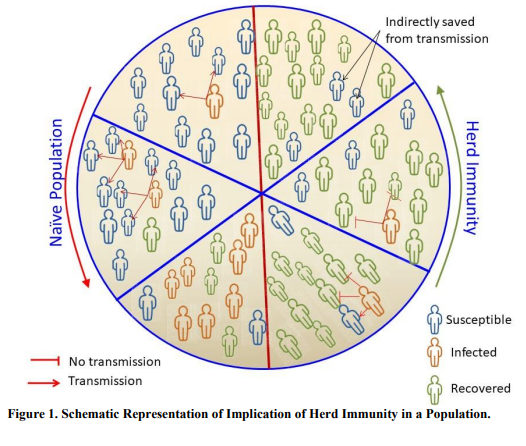
The easiest implementation of herd immunity in a population requires an adequate amount of vaccination. In the 1930s, it was first observed that children became immune to measles because of decreased infection rate even in an unvaccinated population [12]. Since this observation, long mass vaccination has been used to induce herd immunity in a population to reduce the spread of infectious diseases [13].
Also, research reports from Kim et al., 2011, showed that vaccine-induced herd immunity from one age group may confer protection to other age groups as well [14]. According to several reports, community vaccination against pertussis in adults is also found able to confer immunity to young persons and infants [15, 16]. It has also been seen in the case of community vaccination against Pneumococcus disease and Rotavirus diseases where vaccinated individuals were able to confer immunity toward their unvaccinated siblings [17]. But, with the increased age and waning immune system, the efficacy of the vaccine is decreased [18].
Vaccine-induced Herd Immunity, a “Persona Grata” in COVID-19 Treatment
If a vaccine-induced herd immunity can be established in a naïve population against any specific pathogen for a sufficient time, the disease may be inevitably eliminated with zero rates of transmission and the disease may also be declared eradicated [7]. To date, diseases such as rinderpest and smallpox are successful examples of disease eradication from naïve populations through the establishment of vaccination-induced herd immunity [19]. Mandatory vaccination may be beneficial for the implementation of vaccine-induced herd immunity in naive populations [20].
According to the mathematical model for herd immunity as described by Anderson and May in 1985, the herd immunity threshold depends on the basic reproduction number of a population (R0). The basic reproduction number refers to the generation of secondary cases by a single infectious individual at the starting point of a novel outbreak when the rest of the population is susceptible [9]. Consequently, the larger the value of R0, the higher the risk of communicability of the pathogen into a general population [10].
In a naive population, for example, where the R0 is 4, means the novel pathogen may have the ability to infect at least 4 individuals from a single infected host throughout the infectious period. These 4 cases will spread the infection to 16 new individuals in the population during the infectious period. The herd immunity threshold may be depicted mathematically, as 1-1/R0 =1-1/4 =3/4
Therefore, the herd immunity threshold for the population against the novel outbreak is 0.75. This means only 3/4 of the population will be immune to the pathogen. According to Wu et al., 2020, the value of R0 for COVID-19 is 2.68 [2]. In a naïve population, from the value of R0, the minimum percentage of the population (Y) required to achieve herd immunity can be determined [7].Y= [(R0-1)/R0] X 100 = [(2.68-1)/2.68] X 100 =62.686
As a result, in a naïve population, for an R0 value of 2.68, a minimum of 62.686% of the population needs to be immune to gain herd immunity against COVID-19. With this R0 value of COVID-19 which lies between 2.5- 3.5, it will require 60%- 72% of the population to vaccinate to confer herd immunity to the whole population [21]. Therefore, to establish vaccine-induced herd immunity for purpose of suppression from a community about 63% of the population needs to be vaccinated. If any population with an R0 value of 2.68 get succeed to achieve the percentage, then the rate of the spreading of the disease will be zero. Therefore, the daily rate of vaccination should be increased. Apart from vaccination, to avoid getting new COVID cases, individuals in a population should abide by self-protection rules, maintain social distancing and restrict travel so that rate of spreading of the disease becomes slow.
To control this pandemic at its earliest, recovered individuals could contribute plasma to be used in infected persons to subsequently offer immunity to the population. Joseph et al, have further nullified the chance of reinfection by the novel Coronavirus. According to Joseph G, the detection of the Coronavirus may be the result of a diagnostic error or maybe just the reactivation of latent COVID-19 [22]. Herd immunity cannot act as the only long-term alternative option to provide immunity from a specific pathogen in a population.
Though herd immunity may act as an indirect way to provide immunity from a pathogen in a population, it can’t act as the only long-term option to confer immunity against COVID-19 in a population. In addition, the emergence of a new virus strain, due to mutation, may raise a challenge to this indirect population immunity. As one of the currently available options, in the absence of any vaccines or chemotherapeutics against COVID-19, the concept of herd immunity may be applicable to confer indirect immunity in a given population.

Obstacles to Implementation of Vaccine-Induced Herd Immunity against COVID-19
The implementation of vaccine-induced herd immunity may confer immediate indirect immunological protection in a given population by slowing or halting the spread of the disease in a community. Herd immunity is an age-old immune technique that may be an important alternative intervention to control the current covid-19 pandemic. Herd immunity as a method of providing immunity has always been under the radar because of conditions like immunodeficiency or immunosuppression that may not always confer immunity to the individual [23, 7].
The application of herd immunity in a population may be found challenging if the number of free riders increases [24]. Free riders population are unvaccinated people in a population who benefit from immunity development because of those who have been vaccinated and probably paid for the vaccination. There is always a disproportionate relationship between free riders and the successful establishment of herd immunity. Individuals may choose to free riders for a variety of reasons including a belief that may be vaccines are not effective [25].
In addition, the risks associated with vaccines sometimes excludes individual and give rise to several free riders [25]. The main obstacle to establishing ring vaccination-induced herd immunity in a population is the increased number of free riders in the same population. An inadequate vaccination rate in a given population may lead to the return of the disease to the population. According to Rackel and Rackel, a proportion of a vaccinated population may also not develop long-term immunity against the pathogen [26].
It should be noted that vaccination methods for the implication of herd immunity should be country-specific. To eradicate the infection, it would be ideal for countries with enough resources and smaller populations (like; countries of European states) to target total vaccination. On the contrary, countries with large populations may not be able to achieve the whole population vaccination goal due to financial and logistic challenges. Developing countries with huge population burdens may face decreased health economies due to pandemics, resource crunch, and poor management systems to establish mass vaccination in a naive population. To overcome such factors countries with huge populations may choose “vaccination of vulnerable sections” (e.g.aged people, health workers, persons with comorbidities) first. Afterward, they may opt for “age-specific vaccination” (with different age groups) followed by ring vaccination as an alternative vaccination method [27].
Differences in population density, population age structure, comorbidity rates, behavioral patterns, and the implementation of a consistent R0 across the world may prove a challenge and make herd immunity, not a reliable treatment intervention [2]. Geographical variations, as well as cultural differences, may also contribute to different transmission rates of the disease across the world. With varying population densities across the world, the viral loads of the disease may differ. In addition, gaining immune power also differs between individuals in the same population. Furthermore, achieving herd immunity in a naïve population requires a large fraction of the population to be infected, which may lead to a devastating situation for any country. Despite all these challenges as presented, the potential benefit of trying and using herd immunity may be the option available to fight the pandemic.
Molecular Evolution as an Antagonist of Ring Vaccination-Induced Herd Immunity
According to the nature of evolution, evolutionary pressure provokes pathogens to undergo constant mutations. Herd immunity itself acts as a stimulatory factor for further mutation of the pathogen. This kind of evolutionary pressure encourages the microorganism to mutate and produce a novel strain [28]. Eventually, this mutant novel strain will be able to evade herd immunity and therefore proceed to infect people. The virus uses antigenic drift to produce novel strains to escape from vaccination-induced immunity and imposes selection pressure on the community. The recommended vaccines against SARA-COV-2 are currently based on a version of spike glycoprotein. Studies with genome sequencing of SARS-CoV-2 show a nucleotide substitution rate of roughly 1×10-3 substitutions per year which showed a similar rate of producing mutants of the Ebola virus (1.42×10-3 ) [29,30]. SARS-CoV-2 may use single-point mutation, recombination, insertions, and deletions to produce mutants [31]. The rapid rate of mutation may produce multiple genotypic variants but still, vaccines may successfully act, as an immune booster because old versions spike glycoproteins would generate protective antibodies against newer emerging variants [32].
Antibody-Dependent Enhancement (ADE) and Vaccine-induced Herd Immunity
One of the potential factors to account for is the risk of the development of Antibody-Dependent Enhancement (ADE) in individuals post-vaccination. Antibody-based vaccines while conferring immune-boosting activity may result in ADE. ADE may be triggered by excessive immune complex formation or by enhancing Fc-mediated effector functions, which enhances inflammation. These vaccines may result in enhanced antibody-mediated virus uptake which leads to increased replication of the viral body thus enhancing infection [33]. Studies showed that ADE may contribute to higher antibody titers which eventually enhances viral load [34]. Increased in vivo viral load may trigger cytokine storms further. During the development of immune-boosting COVID vaccines, ADE had been observed in animal studies but a clinical trial with humans did not show any pieces of evidence of ADE post-vaccination [35]. Though ADE is a theoretical possibility associated with antibody-based vaccines it may be avoidable (e.g. individuals are requested not to vaccinate themselves who didn’t pass three months after being COVID positive once).

Immunosenescence and Vaccination
The term immunosenescence refers to the gradual deterioration of the immune system with the advancement of age. A systemic meta-data analytic study in 2020 showed significant differences in COVID-19 infection fatality rate (IFR) among different age groups. Meta-regression estimate of IFR has been found low for children and young adults (e.g., 0.002% at age of 10, 0.01% at the age of 25) whereas a progressively increased pattern for IFR with age has been noted (Table 2.) [36]. Also, older adults are found to be at greater risk of requiring hospitalization or death.
Age complications like acute respiratory distress, septic shock, multi-organ failure, cardiac arrest, arrhythmias, and heart inflammation increased [37]. Increased age contributes to decreased antibody production. The time taken by the elderly for the neutralization of viruses is longer compared to young individuals, which leads to an increase in vivo viral load. With age, the functional capacity of T cells is mostly influenced. Due to Immunosenescence, older people face a reduction in the number of naïve T cells available to respond to a vaccine. With age, CD4+ T cell development gets impaired. Impaired development of CD4+ T follicular helper cells hampers the maturation of B cells, which eventually lowers antibody production [38]. Senescence reduces the expression of specific proteins thus antibodies functions get restricted [39].
Additionally, a significant decrease in CD8 T cells with age and alteration of the normal ratio of CD4:CD8 have also been found in the elderly. Which eventually leads to hampered immune defenses against viral pathogens especially cytotoxic CD8+ T cells [40].
Furthermore, in vivo cytokine storm had been pointed out as a prime factor for elderly people to combat with. Due o an increase in serum levels of Interleukin-1 (specifically IL-1B), Interleukin-2 (IL-2), Interleukin-6 (IL-6), Interleukin-10 (IL-10), tumor necrosis factor- α (TNF- α), Interferon- γ (IFN- γ) complications like respiratory distress syndrome, several blood clotting events, vasculitis, acute kidney injury got associated with COVID-19 [41].
Moreover, increased proinflammatory cytokines may affect microglia, neurons as well as astrocytes [41]. Due to the weakening of the immune system older people are taking more time to neutralize the virus and by this time viral load has increased. The older population across the world becoming vulnerable to COVID-19. For this reason, the older population has become a priority to be vaccinated against COVID-19. But, the efficacy of the vaccine may vary according to specific in vivo repercussions.
Therefore, the older community may become able to vaccines earlier than other age groups, but its immune-boosting function remains questionable. The vaccine may become less effective to boost cellular immune responses compared to other age groups. Furthermore, the consequences and side effects of an immune-boosting vaccine on older people may also be even more uncertain.

Conclusion
The application of several sanitization habits, maintaining social distancing, quarantine, complete lockdown of societies, and wearing personal protection equipment, all seem not to have produced the desired and intended effects to control the COVID-19 pandemic as no eminent flattening of the curve is seen. For many developing countries, the implication of ring vaccination-induced herd immunity has been found as a cost-effective measure for the eradication of the contagious disease from a naive population. Though vaccines are the best solution available worldwide to develop immunity against COVID-19, the immune-boosting capacity of vaccines doesn’t last for a lifetime and their effectiveness may change with each mutated strain of the virus.
To overcome such fallacies repeated vaccination within a maximum duration of six months might be effective. Age-specific vaccination may provide some boost to an individual’s immune responses, which can cease the rapid and devastating spread of the disease. But for the speedy eradication of the worldwide pandemic situation vaccination must opt for every single individual in a population irrespective of their age. Vaccination should be for all. This type of indirect immunization, may, for now, act as one of the possible ways to confer immunity to naïve populations in the absence of vaccines and pharmaceuticals against COVID-19.
Acknowledgments
The authors express gratitude to the Department of Pharmacology, University of the Free State, Bloemfontein, Republic of South Africa. Dr. Dassarma and Dr. Tripathy are further thankful to the Department of Research Directorate (DRD) at the University of Free State for providing them with the opportunity to do their postdoctoral fellowships in the Department of Pharmacology at the same University.
Conflict of Interest
The authors declare no conflict of interest.
References
[1] Wei WE, Li Z, Chiew CJ, Yong SE, Toh MP, Lee VJ (2020). Presymptomatic transmission of SARS-CoV2—Singapore, January 23–March 16, 2020. Morb Mortal Wkly Rep, 69: 411.
[2] Wu JT, Leung K, Leung GM (2020). Nowcasting and forecasting the potential domestic and international spread of the 2019-nCoV outbreak originating in Wuhan, China: a modeling study. Lancet, 395: 689- 697.
[3] Lauer SA, Grantz KH, Bi Q, Jones FK, Zheng Q, Meredith HR, et al. (2020). The incubation period of coronavirus disease 2019 (COVID-19) from publicly reported confirmed cases: estimation and application. Ann Intern Med, 172: 577-582.
[4] Russell CD, Millar JE, Baillie JK (2020). Clinical evidence does not support corticosteroid treatment for 2019-nCoV lung injury. Lancet, 395: 473-475.
[5] Wang M, Cao R, Zhang L, Yang X, Liu J, Xu M, et al. (2020). Remdesivir and chloroquine effectively inhibit the recently emerged novel coronavirus (2019-nCoV) in vitro. Cell Res, 30: 269-271.
[6] Merrill RM (2013). Introduction to Epidemiology. Jones & Bartlett Publishers, 68–71.
[7] Somerville M, Kumaran K, Anderson R (2012). Public Health and Epidemiology at a Glance. John Wiley & Sons, 58–59.
[8] Anderson RM, May RM (1985). Vaccination and herd immunity to infectious diseases. Nature, 318(6044): 323-329.
[9] Fine P, Eames K, Heymann DL (2011). “Herd immunity”: a rough guide. Clin Infect Dis, 52(7): 911- 916.
[10] Randolph HE, Barreiro LB (2020). Herd immunity: understanding COVID-19. Immunity, 52(5): 737-741.
[11] Cliff A, Smallman-Raynor M (2013). Oxford Textbook of Infectious Disease Control: A Geographical Analysis from Medieval Quarantine to Global Eradication. Oxford University Press. 125–36.
[12] Orenstein WA, Hinman AR, Papania MJ (Eds.). (2004). Evolution of measles elimination strategies in the United States. J Infect Dis, 189(Supplement_1): S17-S22.
[13] Garnett GP (2005). Role of herd immunity in determining the effect of vaccines against sexually transmitted disease. J Infect Dis, 191(Supplement_1): S97-S106.
[14] Kim TH, Johnstone J, Loeb M (2011). Vaccine herd effect. Scand J Infect Dis, 43(9):683-9.
[15] McGirr A, Fisman DN (2015). Duration of pertussis immunity after DTaP immunization: a meta-analysis. Pediatrics, 135(2): 331-343.
[16] Zepp F, Heininger U, Mertsola J, Bernatowska E, Guiso N, Roord J, et al. (2011). The rationale for pertussis booster vaccination throughout life in Europe. Lancet Infect Dis, 11(7): 557-570.
[17] Pittet LF, Posfay‐Barbe KM (2012). Pneumococcal vaccines for children: a global public health priority. Clin Microbiol Infec, 18: 25-36.
[18] Kim TH (2014). Seasonal influenza and vaccine herd effect. Clin Exp Vaccine Res, 3(2): 128.
[19] Njeumi F, Taylor W, Diallo A, Miyagishima K, Pastoret PP, et al. (2012). The long journey: a brief review of the eradication of rinderpest. Rev Sci Tech, 31(3): 729-746.
[20] Fukuda E, Tanimoto J (2015). Impact of stubborn individuals on the spread of infectious disease under voluntary vaccination policy. In Proceedings of the 18th Asia Pacific Symposium on Intelligent and Evolutionary Systems, 1:1-10.
[21] Anderson RM, Heesterbeek H, Klinkenberg D, Hollingsworth TD (2020). How will country-based mitigation measures influence the course of the COVID-19 epidemic? Lancet, 395(10228): 931-934.
[22] Clark A, Jit M, Warren-Gash C, Guthrie B, Wang HH, Mercer SW, et al. (2020). Global, regional, and national estimates of the population at increased risk of severe COVID-19 due to underlying health conditions in 2020: a modeling study. Lancet Glob, 8(8), e1003-e1017.
[23] Guerra FM, Bolotin S, Lim G, Heffernan J, Deeks SL, Li Y, et al. (2017). The basic reproduction number (R0) of measles: a systematic review. Lancet Infect Dis, 17(12): 420-e428.
[24] Barrett, S. (2014). Global public goods and international development. In Directions in Development-Environment and Sustainable Development,13-51.
[25] Gowda C, Dempsey AF (2013). The rise (and fall?) of parental vaccine hesitancy. Hum Vaccin Immunother, 9(8): 1755-1762.
[26] Rakel D, Rakel RE (2015). Textbook of Family Medicine. Elsevier Health Sciences. 99, 187. ISBN 978-0323313087
[27] Chakrabarti SS, Kaur U, Singh A, Chakrabarti S, Krishnatreya M, Agrawal BK, et al. (2020). Of cross-immunity, herd immunity and country-specific plans: Experiences from COVID-19 in India. Aging Disease, 11(6):1339.
[28] Rodpothong P, Auewarakul P (2012). Viral evolution and transmission effectiveness. World J Virol, 1(5): 131.
[29] Duchene S, Featherstone L, Haritopoulou-Sinanidou M, Rambaut A, Lemey P, Baele G (2020). Temporal signal and the phylodynamic threshold of SARS-CoV2. Virus Evol, 6:a061.
[30] Carroll MW, Matthews DA, Hiscox JA, Elmore MJ, Pollakis G, Rambaut A, et al. (2015). Temporal and spatial analysis of the 2014-2015 Ebola virus outbreak in West Africa. Nature, 524:97 -101.
[31] Davidson AD, Williamson MK, Lewis S, Shoemark D, Carroll MW, Heesom KJ, et al. (2020). Characterization of the transcriptome and proteome of SARS-CoV-2 reveals a cell passage-induced in-frame deletion of the furin-like cleavage site from the spike glycoprotein. Genome Med,12:68.
[32] Darby AC, Hiscox JA. (2021). Covid-19: variants and vaccination. BMJ, 372:n771
[33] Lee WS, Wheatley AK, Kent SJ, DeKosky BJ (2020). Antibody-dependent enhancement and SARS-CoV-2 vaccines and therapies. Nat Microbiol, 5: 1185-1191.
[34] Liu Y, Yan LM, Wan L, Xiang TX, Le A, Liu JM, et al. (2020). Viral dynamics in mild and severe cases of COVID-19. Lancet Infect Dis, 20, 656–657.
[35] Haynes BF, Corey L, Fernandes P, Gilbert PB, Hotez PJ, Rao S, et al. (2020). Prospects for a safe COVID-19 vaccine. Sci Transl Med, 4:12(568).
[36] Levin AT, Hanage WP, Owusu-Boaitey N, Cochran KB, Walsh SP, Meyerowitz-Katz G (2020). Assessing the age specificity of infection fatality rates for COVID-19: systematic review, meta-analysis, and public policy implications. Eur J Epidemiol, 8:1-16.
[37] Soy M, Keser G, Atagündüz P, Tabak F, Atagündüz I, Kayhan S (2020). Cytokine storm in COVID-19: pathogenesis and overview of anti-inflammatory agents used in treatment. J Clin Rheumatol, 39 (7): 2085–2094.
[38] Lefebvre JS, Maue AC, Eaton SM, Lanthier PA, Tighe M, Haynes L (2012). The aged microenvironment contributes to the age‐related functional defects of CD4 T cells in mice. Aging cell, 11(5):732-740.
[39] Soiza RL, Scicluna C, Thomson EC (2021). Efficacy and safety of COVID-19 vaccines in older people. Age Ageing, 50(2):279-283.
[40] Ouyang Q, Wagner WM, Voehringer D, Wikby A, Klatt T, Walter S, et al. (2003). Age-associated accumulation of CMV-specific CD8+ T cells expressing the inhibitory killer cell lectin-like receptor G1 (KLRG1). Exp Gerontol, 38(8): 911-920.
[41] Bhaskar S, Sinha A, Banach M, Mittoo S, Weissert R, Kass JS, et al. (2020). Cytokine Storm in COVID-19- Immunopathological Mechanisms, Clinical Considerations, and Therapeutic Approaches: The REPROGRAM Consortium Position Paper. Front Immunol, 11: 1648.
Barsha Dassarma, Satyajit Tripathy* , Matimbha Chabalala, Motlalepula Gilbert Matsabisa*
Department of Pharmacology, School of Clinical Medicine, Faculty of Health Sciences, University of the Free State,
Bloemfontein9300, SA.






