Hypoxic Mesenchymal Stem Cell-derived Extracellular Vesicles Ameliorate Renal Fbrosis After Ischemia–reperfusion Injure By Restoring CPT1A Mediated Fatty Acid Oxidation
Jul 10, 2023
Abstract
1. Background
Renal fibrosis is a common pathological process of chronic kidney diseases induced by multiple factors. Hypoxic pretreatment of mesenchymal stem cells can enhance the efficacy of secreted extracellular vesicles (MSC-EVs) in various diseases, but it is not clear whether they can better improve renal fibrosis. The latest research showed that recovery of fatty acid oxidation (FAO) can reduce renal fibrosis. In this study, we aimed to examine whether hypoxic pretreatment with MSC extracellular vesicles (Hypo-EVs) can improve FAO to restore renal fibrosis and investigate the underlying mechanism.
2. Methods
Hypo-EVs were isolated from hypoxia-pretreated human placenta-derived MSC (hP-MSC), and Norm-EVs were isolated from hP-MSC cultured under normal conditions. We used the ischemia–reperfusion (I/R)-induced renal fibrosis model in vivo. The mice were injected with PBS, Hypo-EVs, or Norm-EVs immediately after the surgery and day 1 post-surgery. Renal function, kidney pathology, and renal fibrosis were assessed for kidney damage evaluation. For mechanistic exploration, fatty acid oxidation (FAO), mitochondrial morphological alterations, ATP production, and mitochondrial mass proteins were detected in vivo. Mitochondrial membrane potential and reactive oxygen species (ROS) production were investigated in vitro.
3. Results
We found that Hypo-EVs confer a superior therapeutic effect on the recovery of renal structure damage, restoration of renal function, and reduction in renal fibrosis. Meanwhile, Hypo-EVs enhanced mitochondrial FAO in the kidney by restoring the expression of an FAO key rate-limiting enzyme carnitine palmitoyl-transferase 1A (CPT1A). Mechanistically, the improvement of mitochondrial homeostasis, characterized by repaired mitochondrial structure, restoration of mitochondrial mass and ATP production, inhibition of oxidative stress, and increased mitochondrial membrane potential, partially explains the effect of Hypo-EVs on improving mitochondrial FAO and thus attenuating I/R damage.
4. Conclusions
Hypo-EVs suppress renal fibrosis by restoring CPT1A-mediated mitochondrial FAO, which effects may be achieved through the regulation of mitochondrial homeostasis. Our findings provide further mechanism support for the development of cell-free therapy for renal fibrosis.
5. Keywords
Mesenchymal stem cell, Hypoxic, Extracellular vesicles, Mitochondrial, Fatty acid oxidation, Renal fibrosis.

Click here to buy the Cistanche supplement
Introduction
Chronic kidney disease (CKD) is a severe disease threatening human health and is also an important global public issue. The global incidence, prevalence, and death of CKD are significant, and rising, and the prevalence is approximately 10% among adults worldwide [1, 2]. Renal ischemia-reperfusion (I/R) injury is associated with renal fibrosis and progressive CKD [3, 4]. Renal fibrosis is considered a common pathological process that leads to CKD and end-stage renal disease. However, there are currently no effective therapies that successfully prevent or reverse fibrosis [5].
Mesenchymal stem cell-derived extracellular vesicles (MSC-EVs) has been reported to play a regenerative and antifibrotic role in several preclinical models of CKD [6– 9]. However, the low yield of MSC-EVs is a limiting factor for the large-scale production of cell-free therapies [10]. Hypoxia preconditioning stimulates the paracrine activities of MSCs and increases the function and production of EVs and is considered an engineering approach to improve the therapeutic potential of EVs [11, 12]. A recent study indicated that hypoxia-preconditioned MSCs are more significant than untreated MSCs in preventing renal fibrosis and inflammation [13]. However, the role of hypoxia-preconditioned MSC-derived EVs in renal fibrosis has not yet been established.
The pathological mechanism of renal fibrosis has been reviewed in many recent studies [14–16], particularly in the field of metabolic regulation [17]. It is well known that proximal tubular cells (PTCs) are the most energy-demanding cells in the kidney and play a central role in tubulointerstitial fibrosis progression [18, 19]. Fatty acid oxidation (FAO) is the primary energy source of PTCs [19, 20]. The results of genome-wide transcriptome studies showed that the expression of FAO-related key metabolic enzymes and transcription regulators was markedly decreased in human and mouse models with tubulointerstitial fibrosis [20]. In addition, restoring fatty acid metabolism can protect mice from tubulointerstitial fibrosis [17, 20]. A recent study confirmed that overexpression of the key rate-limiting enzyme carnitine palmitoyl-transferase 1A (CPT1A) can enhance FAO in renal tubular epithelial cells, reduce the expression of inflammatory mediators, and lead to significant alleviation of fibrosis in three experimental models [21]. Therefore, FAO-targeted therapies may be a potentially effective therapeutic strategy for fibrosis reduction.
Mitochondria play an indispensable role in regulating FAO. A previous study indicated that astragaloside IV can enhance FAO by regulating mitochondrial activity during aging [22]. The destruction of mitochondrial homeostasis plays an important role in the early injury of kidney disease, abnormal repair after injury, and the pathogenesis of CKD [23, 24]. Under physiological and pathological conditions, various mechanisms coordinate to maintain mitochondrial homeostasis, including antioxidant defense, mitochondrial DNA repair, mitochondrial fusion and fission, mitochondrial autophagy, and mitochondrial biogenesis [25]. Several studies have shown that MSC-EVs can attenuate mitochondrial damage by stabilizing mitochondrial DNA [26], inhibiting mitochondrial fission, and stimulating the mitochondrial antioxidant defense and adenosine triphosphate (ATP) production in acute kidney injury (AKI) models [27, 28]. Previous studies indicated that Hypo-EVs treatment had better effects on promoting angiogenesis, proliferation, and migration, and inhibiting inflammation and apoptosis than Norm-EVs treatment [29–31]. Nevertheless, researchers have not conclusively determined whether the therapeutic outcomes of Hypo-EVs in fibrosis depend on mitochondrial homeostasis.
The aims of this study were (1) to explore whether hypoxic pre-treatment of MSCs-derived extracellular vesicles(Hypo-EVs) has a better anti-fibrosis effect; (2) to determine whether Hypo-EVs alleviate ischemia reperfusion-induced fibrosis by enhancing CPT1A-mediated FAO; (3) to examine whether the protective effect of Hypo-EVs on FAO is related to the regulation of mitochondrial homeostasis.

Cistanche powder
Methods
1. Cell culture and hypoxia preconditioning
Human placenta-derived MSC (hP-MSC) were provided by the Institute of Foundation, Chinese Academy of Medical Sciences and cultured in Dulbecco’s Modified Eagle’s Medium/Nutrient Mixture F-12 (DMEM/F12, Gibco) medium with 10% fetal bovine serum (FBS, Corning) supplemented with 100 U/mL penicillin−streptomycin (Gibco) and maintained at 37 °C in a humidified 5% CO2 atmosphere. After the hP-MSC reached 60%–70% confluency, the culture media were replaced with exosome-depleted FBS (SBI, 50A-1) and were cultured at 37 °C, 5% CO2, 21% O2 or at 1% O2, 94% N2, and 5% CO2 for an additional 48 h. The medium was then collected for EVs isolation, and the EVs collected from the hypoxic pretreatment of MSC (1% O2) were called Hypo-EVs, and the normal MSC (21% O2) was called Norm-EVs. Only hP-MSC from passages 6–10 were used for further experiments.
2. Cell culture and treatment
Human renal proximal tubular epithelial (HK-2, ATCC, USA) cells were cultured in DMEM/F12 with 10% FBS and supplemented with 100 U/mL penicillin−streptomycin. The cells were maintained at 37 °C in a humidified atmosphere containing 5% CO2. We used two approaches to mimic CKD in vitro. The cell hypoxia/reoxygenation (H/R) model was performed as previously reported [32]. Briefly, HK-2 cells were exposed to a hypoxic condition (37℃, 1% O2, 94% N2, and 5% CO2) for 12 h in glucose and serum-free medium to induce hypoxic injury. Subsequently, the medium was replaced, and the cells were placed under the normal condition (21% O2) for reoxygenation 24 h. The control group was cultured under the normal condition (21% O2) according to the experimental design. Another method was to incubate HK-2 cells with transforming growth factor beta-1 (TGF-β1) at a final concentration of 10 ng/mL for 48 h as previously reported [13]. During reoxygenation or TGF-β1- stimulated time Norm-EVs or Hypo-EVs (100 μg/mL of nutrient medium) were added to the cells.
3. MSC‑EVs isolation and identification
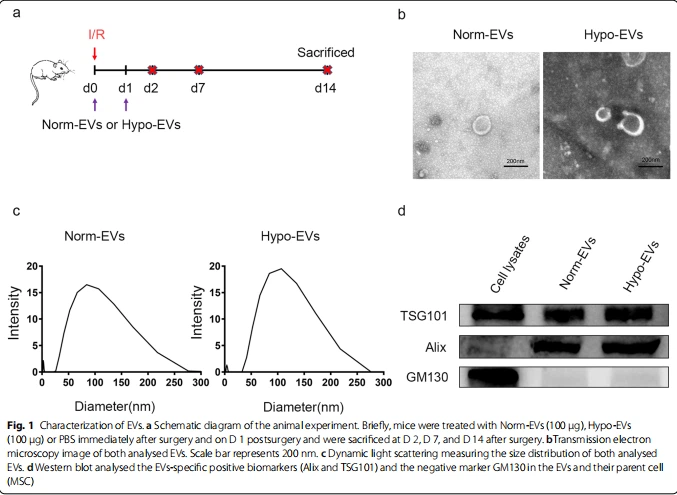
MSC-derived EVs were isolated using a differential ultracentrifugation method. Briefly, the culture medium was centrifuged at 4 °C as follows: 500×g for 10 min, at 2,000×g for 20 min, and 10,000×g for 30 min. The medium was filtered through a 0.22-μm filter before ultracentrifugation at 100,000×g for 2 h. Finally, the EV pellets were resuspended in PBS and ultracentrifuged for an additional 2 h to discard the contaminating proteins, and then the purified EVs were harvested in PBS and stored at−80 °C for further use. The protein concentrations of the Norm-EVs and Hypo-EVs were examined using a bicinchoninic acid protein assay (BCA, Thermo Fisher Scientific, Waltham, MA, USA). The typical sphere-shaped bilayer membrane structure of the EVs was observed using transmission electron microscopy (TEM). Western blotting was used to examine the quality of the EVs, and the size distribution of the EVs was examined by dynamic light scattering (DLS).

Cistanche tubulosa
4. Animal experiments
Male C57BL/6 SPF mice (7–9 weeks old) were supplied by the Sibeifu Experimental Animal Science and Technology (Beijing, China) and were fed adaptively for 4 d in the animal center at the Chinese PLA General Hospital before the experiment. The mice were randomly divided into four groups: the control, phosphate-buffered saline (PBS), Norm-EVs, and Hypo-EVs groups. Mice of PBS, Norm-EVs, and Hypo-EVs groups were subjected to renal ischemia-reperfusion as described previously [33, 34]. Briefly, mice were anesthetized with pentobarbital (50 mg/kg) through intraperitoneal injection. The dorsal hair above the mouse kidney was cleaned and then the bilateral renal pedicle vessels were exposed. To induce renal ischemia, the left renal artery was clamped with a nontraumatic vascular clamp for 30 min and the right kidney was removed simultaneously. Afterward, reperfusion was initiated by releasing the clamp. The kidneys were observed for 5 min to ensure reperfusion after the clamp was removed. The operating table and room temperature were maintained at 37 °C during surgery. In treatment models, 100 μg of Norm-EVs or Hypo-EVs in 0.15 mL of PBS solvent was administered by tail vein injection immediately after the surgery and day (D) 1 postsurgery in the Norm-EVs and Hypo-EVs groups, respectively. The same volume of PBS was administered by tail vein injection in the PBS group. The mice were killed at D 2, D 7, and D 14 after surgery (Fig. 1a).
5. MSC‑EVs internalization
To verify whether EVs could be internalized by injured kidneys. Dil (Yeasen) fluorescent staining was performed to label the EVs. Te Norm-EVs or Hypo-EVs (200 μg) that were dissolved in 100 μL of PBS were incubated with 4 μM of Dil at 37 °C for 1 h. The unbound dyes were then removed using an exosome spin column (Invitrogen). The Di/Norm-EVs and Dil/Hypo-EVs were suspended in PBS for subsequent use. Dil/Norm-EVs or Dil/HypoEVs(100 μg) were intravenously injected into an ischemia–reperfusion injury (I/R) model mice via the tail vein immediately after the surgery and on D 1 postsurgery as mentioned above. On days 1, 3, 5, and 7, the mice were imaged immediately using Living Image Software 4.4 (PerkinElmer). Moreover, the kidneys were collected and observed on an optical imaging system on D 7. All bioluminescence imaging (BLI) signals were measured by the average radiance from the regions of interest (ROIs).
6. Transmission electron microscope(TEM)
A total of 1 mm3 of kidney tissue was fixed in 2.5% glutaraldehyde (pH 7.4) at 4℃ for 24 h. Then, the tissue was fixed with 1% osmium acid for 2–3 h, dehydrated with acetone and ethanol, and embedded with epoxy resin. After that, an ultramicrotome was used to prepare ultrathin sections with a thickness of 60 nm, which were then stained with 3% uranyl acetate and lead citrate. Finally, the section was observed under a TEM (Japan).
7. Renal function analysis
A blood sample was collected from the tail vein on D 3, and the levels of blood urea nitrogen (BUN) in the mice were tested using an appropriate kit (Bioassay).
8. Renal histopathology assessment
Renal tissues were fixed in 10% formalin for 48 h, embedded in paraffin, sectioned at 3 μm thickness, stained with Masson staining reagents by a standard protocol, and observed using a microscope (Olympus, Tokyo, Japan). The percentage of collagen deposition area was calculated using ImageJ software. There were at least 10 random non-overlapping fields per animal for scoring.
9. Immunohistochemistry
The paraffin-embedded kidney sections were pretreated using heat-mediated antigen retrieval with sodium citrate buffer (pH 6, epitope retrieval solution 1) for 20 min, followed by incubation with primary antibodies overnight at 4 °C. The sections were then incubated with a biotinylated secondary antibody, and 3,3’-diaminobenzidine (DAB) was used as the chromogen. The sections were then counterstained with hematoxylin and observed with an optical microscope. The primary antibodies used were as follows: CPT1A (ab128568, Abcam), and Vimentin (ab92547, Abcam).
10. Immunofluorescence
Cells or tissue were permeabilized with 0.2% Triton X-100 for 5 min, blocked with sheep serum for 30 min, and incubated with α-smooth muscle actin (α-SMA, 1:200, 55135, Proteintech) or collagen I (1:100, ab270993, Abcam) antibody for 16–18 h at 4 °C, followed by incubation with Cy3‐conjugated secondary antibody (red) at room temperature for 1 h. Nuclei were counterstained with DAPI. Fluorescent staining of the tissue sections was imaged by confocal fluorescence microscopy.
11. Western blotting analysis
The kidneys, cells, or EVs pellets were lysed in RadioImmune Precipitation Assay (RIPA) lysis buffer containing phenylmethylsulphonyl fluoride (PMSF), and the supernatant suspension obtained after centrifugation was measured using a BCA protein assay kit (Thermo Fisher Scientific). Protein samples of the same quality (20 μg/ lane) were added to a 10% or 12% sodium dodecyl sulfate–polyacrylamide gel (SDS-PAGE) and then transferred from the SDS-PAGE gels to the membranes. The membrane was blocked for 2 h at room temperature with a 1X casein solution and then incubated with primary antibodies at 4 °C against the following proteins: α-SMA (ab7817, Abcam), vimentin (ab92547, Abcam), glyceraldehyde 3-phosphate dehydrogenase (GAPDH, 60004-1- Ig, Proteintech), actin (20536-1-AP, Proteintech), PGC1α (ab191838, Abcam), CPT1A (ab128568, Abcam), succinate dehydrogenase complex iron sulfur subunit B (SDHB, 10620-1-AP, Proteintech), cytochrome c oxidase subunit IV (COXIV, ab202554, Abcam), and ATPB (17247-1-AP, Proteintech). The membrane was then incubated with the corresponding secondary antibody for 1.5 h at room temperature and washed three times. The images were analyzed using ImageJ software.
12. Quantitative real‑time polymerase chain reaction (RT‑qPCR)
First, RNA was extracted from the lysed cells or kidney tissue using Trizol reagent (Invitrogen), and then the RNA was synthesized to cDNA according to the manufacturer’s instructions using the ReverTra Ace qPCR RT kit (Toyobo). Quantitative real-time polymerase chain reaction was performed using SYBR Select Master Mix (Life Technologies) and an RT-qPCR detection system (ABI). The primers for the following genes were synthesized: PPARα forward TTTGCCAAGGCTATCCCAGG, reverse GTCACAGAACGGCTTCCTCA,
PGC1α forward AATGCAGCGGTCTTAGCACT, reverse CTGAGCAGGGACGTCTTTGT, ACOX2 TCATCCAACGTGACCCAGTG, reverse CAG CAAGGACTCTGTCAGCA, CPT2 forward CATCGT ACCCACCATGCACT, reverse CTCCTTCCCAATGCC GTTCT, 18S AGCTATCAATCTGTCAATCCT GTC, reverse GCTTAATTTGACTCAACACGGGA, and the expression of each target gene was normalized by the 18S gene and calculated by the 2−ΔΔCT method.
13. Measurement of mitochondrial membrane potential
The mitochondrial membrane potential (MMP) was detected using JC-1 (Beyotime). First, JC-1 staining working solution was obtained by adding 8 mL ultrapure water for every 50 μL of JC-1 (200X), which was vortexed violently to fully dissolve, and then 2 mL of JC-1 staining buffer (5X) was added. Second, cells in a six-pore plate were washed twice in PBS, and then 1 mL of JC-1 staining working solution was added and left for 20 min at 37° C. Finally, the cells were washed with PBS again, and 2 mL of the cell culture solution was added. Visualized images were acquired using fluorescence microscopy.
Cistanche capsules
14. Mitochondrial reactive oxygen species (ROS) detection
Mitochondrial ROS generation was measured by fluorescence microscopy using Mito-SOX Red (Thermo Fisher Scientific). MitoSOX reagent working solution (2.0 mL, 5 μM) was added to cover the cells in the six-pore plates, followed by staining with MitoSOX Red for 10 min at 37 °C. Then, the cells were washed with PBS three times, and the visualized images were acquired using fluorescence microscopy.
15. ATP detection
ATP production was determined through the Enhanced ATP Assay Kit (Beyotime, China, Cat. No: S0027) according to the manufacturer’s protocol.
16. Statistical analysis
The quantification and graphs were analyzed using GraphPad Prism 7 (La Jolla, CA, USA) and presented as mean±standard error of the mean. Differences between multiple groups were analyzed using analysis of variance (ANOVA), and statistical significance was set at P < 0.05.
Discussion
In this study, we focused on the FAO in renal fibrosis, and we identified metabolic enzymes(CPT1A) and transcription regulators (PGC1α, PPARα) of FAO, which indicated that Hypo-EVs can reverse fatty acid metabolism disorder in fibrotic kidney caused by I/R. Moreover, we found that Hypo-EVs exert a profound effect on CPT1A-mediated FAO, which is partly attributed to the regulation of mitochondrial homeostasis.
In recent years, an increasing number of studies have reported the renal protective effect of MSC-EVs in vivo models of CKD and a small amount of available data demonstrated that EVs were superior to or equally effective in renoprotection compared with their parent MSC [43]. The treatment of MSC-EVs in CKD is in its infancy, and the complex mechanism has not been fully demonstrated. AKI is one of the major factors of CKD, which leads to end-stage renal disease [44], and renal I/R injury is a major factor for AKI, so we select I/R induced fibrosis model to uncover potential molecular mechanism that how MSC-EVs prevents renal fibrosis.
The low yield of MSC-EVs is a limiting factor for the large-scale production of cell-free therapies. Thus, various potential approaches to increase the yield of EVs have been studied, including optimization of MSC culture conditions, three-dimensional extracellular matrix-based scaffolds, and regulation of EVs biogenesis [10]. Among them, hypoxic conditioning of MSC is a valid method to augment the effect of EV treatment in various diseases, such as bone fracture healing [30], diabetic wound healing [29], and myocardial repair [45]. Our study provides evidence for the hypoxia-enhanced action of EVs secreted by MSC. Moreover, we also show that hypoxic preconditioned MSC-derived EVs have a greater anti-fibrosis and renal protective effect than Norm-EVs in CKD induced by I/R. Data on miRNAs in Hypo-EVs compared to Norm-EVs have been well reported. Numerous studies have reported that miRNA content was responsible for the beneficial effects of Hypo-EVs in many diseases [30, 46]. Compared with Norm-EVs, 215 miRNAs were upregulated and 369 miRNAs downregulated in adipose-derived Hypo-EVs, which mainly regulate cell metabolism, differentiation, and TGF-β function [29]. However, the mechanism by which Hypo-EVs regulate metabolism function remains poorly understood in CKD. A large body of literature indicates that FAO is reduced in kidney fibrosis and contributes to its pathogenesis [47]. Consistent with the reports, our study showed that the gene expression of FAO-related key metabolic enzymes (CPT1A, CPT2, and ACOX2) and the FAO transcription regulatory factors (PPARα and PGC1α) were markedly decreased in renal fibrosis induced by I/R.
Moreover, restoration of lipid metabolism is a potential strategy for treating renal fibrosis [48]. The overexpression of CPT1A in kidney tubules is a significant contributor to the gain of function in FAO and results in the protection of renal function and fibrosis by preventing mitochondrial dysfunction, TEC differentiation, and inflammation in CKD animal models [21]. Our data showed that Hypo-EVs could well reverse damaged FAO in I/R-induced fibrosis, which suggests that the therapeutic effects of Hypo-EVs in renal fibrosis are partly the result of restoring FAO.
Impairment in renal PPARα signaling decreased activity of the FAO pathway and aggravated renal fibrosis development [49]. Administration of fenofibrate, a PPARα agonist, restored the fatty oxidation defect and tubulointerstitial fibrosis in CKD [50, 51]. PGC-1α is a coactivator of PPARα in the transcriptional control of mitochondrial FAO capacity [39]. We investigated whether HypoEVs can increase PPARα signaling and restore FAO in I/R injury. Our results showed that there were no obvious differences in the expression of PGC-1α and PPARa between Norm-EVs and Hypo-EVs. Therefore, there must be other factors that promote the occurrence of this process. Mitochondria are the powerhouse for FAO to generate energy for the cell [52]. Mitochondrial dysfunction is critical in the pathogenesis of kidney fibrosis [53]. Restoration of mitochondrial homeostasis has emerged as a promising therapeutic strategy to prevent kidney injury and accelerate kidney repair [25]. Recent studies have indicated that MSC-EVs have a protective effect on mitochondrial damage caused by AKI, which protects TECs against insult by reducing mitochondrial fragmentation, normalizing mitochondrial membrane potential, and reversing mtDNA deletion and mitochondrial OXPHOS defects [26, 27]. Our results showed that Hypo-EVs treatment recovered abnormal mitochondrial morphology shift, increased mitochondrial mass, and enhanced mitochondrial function in fibrotic kidneys. Our findings indicate that the effects of Hypo-EVs on FAO may be achieved by regulating mitochondrial homeostasis.
There are some limitations in our study. For example, our data demonstrate that Hypo-EVs have better antifibrotic effects in I/R injury mice than Norm-EVs. However, we did not determine the differential expression of contents between Norm-EVs and Hypo-EVs and also not evaluated the specific manner by which Hypo-EVs affect mitochondrial homeostasis in this study.

The Cistanche benefits
Conclusions
In summary, our data indicate that Hypo-EVs significantly inhibit renal fibrosis by restoring CPT1Amediated FAO, and these effects may be achieved by regulating mitochondrial homeostasis. Our findings provide further mechanical support for the development of cell-free therapy for renal fibrosis.
References
1. Kalantar-Zadeh K, Jafar TH, Nitsch D, Neuen BL, Perkovic V. Chronic kidney disease. Lancet. 2021;398(10302):786–802.
2. Xie Y, Bowe B, Mokdad AH, Xian H, Yan Y, Li T, Maddukuri G, Tsai CY, Floyd T, Al-Aly Z. Analysis of the Global Burden of Disease study highlights the global, regional, and national trends of chronic kidney disease epidemiology from 1990 to 2016. Kidney Int. 2018;94(3):567–81.
3. Ronco C, Bellomo R, Kellum JA. Acute kidney injury. Lancet. 2019;394(10212):1949–64.
4. Zheng Z, Li C, Shao G, Li J, Xu K, Zhao Z, Zhang Z, Liu J, Wu H. Hippo-YAP/ MCP-1 mediated tubular maladaptive repair promote inflammation in renal failed recovery after ischemic AKI. Cell Death Dis. 2021;12(8):754.
5. Yan H, Xu J, Xu Z, Yang B, Luo P, He Q. Defining therapeutic targets for renal fibrosis: exploiting the biology of pathogenesis. Biomed Pharmacother. 2021;143:112115.
6. Shi Z, Wang Q, Zhang Y, Jiang D. Extracellular vesicles produced by bone marrow mesenchymal stem cells attenuate renal fibrosis, in part by inhibiting the RhoA/ROCK pathway, in a UUO rat model. Stem Cell Res Ther. 2020;11(1):253.
7. Kholia S, Herrera Sanchez MB, Cedrino M, Papadimitriou E, Tapparo M, Deregibus MC, Bruno S, Antico F, Brizzi MF, Quesenberry PJ, Camussi G. Mesenchymal stem cell-derived extracellular vesicles ameliorate kidney injury in aristolochic acid nephropathy. Front Cell Dev Biol. 2020;8:188.
8. Birtwistle L, Chen XM, Pollock C. Mesenchymal stem cell-derived extracellular vesicles to the rescue of renal injury. Int J Mol Sci. 2021;22(12):6596.
9. Huang Y, Yang L. Mesenchymal stem cells and extracellular vesicles in therapy against kidney diseases. Stem Cell Res Ther. 2021;12(1):219.
10. Phan J, Kumar P, Hao D, Gao K, Farmer D, Wang A. Engineering mesenchymal stem cells to improve their exosome efficacy and yield for cell-free therapy. J Extracell Vesicles. 2018;7(1):1522236.
11. Bister N, Pistono C, Huremagic B, Jolkkonen J, Giugno R, Malm T. Hypoxia and extracellular vesicles: a review on methods, vesicular cargo, and functions. J Extracell Vesicles. 2020;10(1): e12002.
12. Yang Y, Lee EH, Yang Z. Hypoxia conditioned mesenchymal stem cells in tissue regeneration application. Tissue Eng Part B Rev 2021.
13. Ishiuchi N, Nakashima A, Doi S, Yoshida K, Maeda S, Kanai R, Yamada Y, Ike T, Doi T, Kato Y, Masaki T. Hypoxia-preconditioned mesenchymal stem cells prevent renal fibrosis and inflammation in ischemia-reperfusion rats. Stem Cell Res Ther. 2020;11(1):130.
14. Panizo S, Martinez-Arias L, Alonso-Montes C, Cannata P, Martin-Carro B, Fernandez-Martin JL, Naves-Diaz M, Carrillo-Lopez N, Cannata-Andia JB. Fibrosis in chronic kidney disease: pathogenesis and consequences. Int J Mol Sci. 2021;22(1):408.
15. Humphreys BD. Mechanisms of renal fibrosis. Annu Rev Physiol. 2018;80:309–26.
16. Nastase MV, Zeng-Brouwers J, Wygrecka M, Schaefer L. Targeting renal fibrosis: mechanisms and drug delivery systems. Adv Drug Deliv Rev. 2018;129:295–307.
17. Zhao X, Kwan JYY, Yip K, Liu PP, Liu FF. Targeting metabolic dysregulation for fibrosis therapy. Nat Rev Drug Discov. 2020;19(1):57–75.
18. Qi R, Yang C. Renal tubular epithelial cells: the neglected mediator of tubulointerstitial fibrosis after injury. Cell Death Dis. 2018;9(11):1126.
19. Gewin LS. Renal fibrosis: the primacy of the proximal tubule. Matrix Biol. 2018;68:248–62.
20. Kang HM, Ahn SH, Choi P, Ko YA, Han SH, Chinga F, Park AS, Tao J, Sharma K, Pullman J, Bottinger EP, Goldberg IJ, Susztak K. Defective fatty acid oxidation in renal tubular epithelial cells has a key role in kidney fibrosis development. Nat Med. 2015;21(1):37–46.
21. Miguel V, Tituana J, Herrero JI, Herrero L, Serra D, Cuevas P, Barbas C, Puyol DR, Marquez-Exposito L, Ruiz-Ortega M, Castillo C, Sheng X, Susztak K, Ruiz-Canela M, Salas-Salvado J, Gonzalez MAM, Ortega S, Ramos R, Lamas S. Renal tubule Cpt1a overexpression protects from kidney fibrosis by restoring mitochondrial homeostasis. J Clin Invest. 2021;131(5):e140695.
22. Luo Z, Wang Y, Xue M, Xia F, Zhu L, Li Y, Jia D, Chen S, Xu G, Lei Y. Astragaloside IV ameliorates fat metabolism in the liver of aging mice through targeting mitochondrial activity. J Cell Mol Med. 2021;25(18):8863–76.
23. Bhargava P, Schnellmann RG. Mitochondrial energetics in the kidney. Nat Rev Nephrol. 2017;13(10):629–46.
24. Jiang M, Bai M, Lei J, Xie Y, Xu S, Jia Z, Zhang A. Mitochondrial dysfunction and the AKI-to-CKD transition. Am J Physiol Renal Physiol. 2020;319(6): F1105–16.
25. Tang C, Cai J, Yin XM, Weinberg JM, Venkatachalam MA, Dong Z. Mitochondrial quality control in kidney injury and repair. Nat Rev Nephrol. 2021;17(5):299–318.
26. Zhao M, Liu S, Wang C, Wang Y, Wan M, Liu F, Gong M, Yuan Y, Chen Y, Cheng J, Lu Y, Liu J. Mesenchymal stem cell-derived extracellular vesicles attenuate mitochondrial damage and inflammation by stabilizing mitochondrial DNA. ACS Nano. 2021;15(1):1519–38.
27. Cao H, Cheng Y, Gao H, Zhuang J, Zhang W, Bian Q, Wang F, Du Y, Li Z, Kong D, Ding D, Wang Y. In vivo tracking of mesenchymal stem cell-derived extracellular vesicles improving mitochondrial function in renal ischemia-reperfusion injury. ACS Nano. 2020;14(4):4014–26.
28. Gu D, Zou X, Ju G, Zhang G, Bao E, Zhu Y. Mesenchymal stromal cells derived extracellular vesicles ameliorate acute renal ischemia-reperfusion injury by inhibition of mitochondrial fission through miR-30. Stem Cells Int. 2016;2016:2093940.
29. Wang J, Wu H, Peng Y, Zhao Y, Qin Y, Zhang Y, Xiao Z. Hypoxia adipose stem cell-derived exosomes promote high-quality healing of diabetic wound involves activation of PI3K/Akt pathways. J Nanobiotechnology. 2021;19(1):202.
30. Liu W, Li L, Rong Y, Qian D, Chen J, Zhou Z, Luo Y, Jiang D, Cheng L, Zhao S, Kong F, Wang J, Zhou Z, Xu T, Gong F, Huang Y, Gu C, Zhao X, Bai J, Wang F, Zhao W, Zhang L, Li X, Yin G, Fan J, Cai W. Hypoxic mesenchymal stem cell-derived exosomes promote bone fracture healing by the transfer of miR-126. Acta Biomater. 2020;103:196–212.
31. Rong Y, Zhang J, Jiang D, Ji C, Liu W, Wang J, Ge X, Tang P, Yu S, Cui W, Cai W. Hypoxic pretreatment of small extracellular vesicles mediate cartilage repair in osteoarthritis by delivering miR-216a-5p. Acta Biomater. 2021;122:325–42.
32. Yang C, Chen Z, Yu H, Liu X. Inhibition of Disruptor of Telomeric Silencing 1-Like Alleviated Renal Ischemia and Reperfusion Injury-Induced Fibrosis by Blocking PI3K/AKT-Mediated Oxidative Stress. Drug Des Devel Ther. 2019;13:4375–87.
33. Qian Y, Qian C, Xie K, Fan Q, Yan Y, Lu R, Wang L, Zhang M, Wang Q, Mou S, Dai H, Ni Z, Pang H, Gu L. P2X7 receptor signaling promotes inflammation in renal parenchymal cells suffering from ischemia-reperfusion injury. Cell Death Dis. 2021;12(1):132.
34. Hu MC, Shi M, Gillings N, Flores B, Takahashi M, Kuro OM, Moe OW. Recombinant alpha-Klotho may be prophylactic and therapeutic for acute to chronic kidney disease progression and uremic cardiomyopathy. Kidney Int. 2017;91(5):1104–14.
35. Dubois V, Eeckhoute J, Lefebvre P, Staels B. Distinct but complementary contributions of PPAR isotypes to energy homeostasis. J Clin Investig. 2017;127(4):1202–14.
36. Desvergne B, Wahli W. Peroxisome proliferator-activated receptors: nuclear control of metabolism. Endocr Rev. 1999;20(5):649–88.
37. Libby AE, Jones B, Lopez-Santiago I, Rowland E, Levi M. Nuclear receptors in the kidney during health and disease. Mol Aspects Med. 2021;78:100935.
38. Bougarne N, Weyers B, Desmet SJ, Deckers J, Ray DW, Staels B, De Bosscher K. Molecular actions of PPARalpha in lipid metabolism and inflammation. Endocr Rev. 2018;39(5):760–802.
39. Vega RB, Huss JM, Kelly DP. The coactivator PGC-1 cooperates with peroxisome proliferator-activated receptor alpha in transcriptional control of nuclear genes encoding mitochondrial fatty acid oxidation enzymes. Mol Cell Biol. 2000;20(5):1868–76.
40. Li SY, Susztak K. The role of peroxisome proliferator-activated receptor gamma coactivator 1alpha (PGC-1alpha) in kidney disease. Semin Nephrol. 2018;38(2):121–6.
41. Fransen M, Lismont C, Walton P. The peroxisome-mitochondria connection: How and why? Int J Mol Sci. 2017;18(6):1126.
42. Aparicio-Trejo OE, Avila-Rojas SH, Tapia E, Rojas-Morales P, Leon-Contreras JC, Martinez-Klimova E, Hernandez-Pando R, Sanchez-Lozada LG, PedrazaChaverri J. Chronic impairment of mitochondrial bioenergetics and beta-oxidation promotes experimental AKI-to-CKD transition induced by folic acid. Free Radic Biol Med. 2020;154:18–32.
43. Eirin A, Lerman LO. Mesenchymal stem/stromal cell-derived extracellular vesicles for chronic kidney disease: Are We there yet? Hypertension. 2021;78(2):261–9.
44. Kurzhagen JT, Dellepiane S, Cantaluppi V, Rabb H. AKI: an increasingly recognized risk factor for CKD development and progression. J Nephrol. 2020;33(6):1171–87.
45. Zhu J, Lu K, Zhang N, Zhao Y, Ma Q, Shen J, Lin Y, Xiang P, Tang Y, Hu X, Chen J, Zhu W, Webster KA, Wang J, Yu H. Myocardial reparative functions of exosomes from mesenchymal stem cells are enhanced by hypoxia treatment of the cells via transferring microRNA-210 in a nSMase2- dependent way. Artif Cells Nanomed Biotechnol. 2018;46(8):1659–70.
46. Zhu LP, Tian T, Wang JY, He JN, Chen T, Pan M, Xu L, Zhang HX, Qiu XT, Li CC, Wang KK, Shen H, Zhang GG, Bai YP. Hypoxia-elicited mesenchymal stem cell-derived exosomes facilitate cardiac repair through miR-125b-mediated prevention of cell death in myocardial infarction. Theranostics. 2018;8(22):6163–77.
47. Xie YH, Xiao Y, Huang Q, Hu XF, Gong ZC, Du J. Role of the CTRP6/AMPK pathway in kidney fibrosis through the promotion of fatty acid oxidation. Eur J Pharmacol. 2021;892:173755.
48. Chen YY, Chen XG, Zhang S. Druggability of lipid metabolism modulation against renal fibrosis. Acta Pharmacol Sin. 2021.
49. Chung KW, Lee EK, Lee MK, Oh GT, Yu BP, Chung HY. Impairment of PPARalpha and the fatty acid oxidation pathway aggravates renal fibrosis during aging. J Am Soc Nephrol. 2018;29(4):1223–37.
50. Han SH, Malaga-Dieguez L, Chinga F, Kang HM, Tao J, Reidy K, Susztak K. Deletion of Lkb1 in renal tubular epithelial cells leads to CKD by altering metabolism. J Am Soc Nephrol. 2016;27(2):439–53.
51. Jao TM, Nangaku M, Wu CH, Sugahara M, Saito H, Maekawa H, Ishimoto Y, Aoe M, Inoue T, Tanaka T, Staels B, Mori K, Inagi R. ATF6alpha downregulation of PPARalpha promotes lipotoxicity-induced tubulointerstitial fibrosis. Kidney Int. 2019;95(3):577–89.
52. Spinelli JB, Haigis MC. The multifaceted contributions of mitochondria to cellular metabolism. Nat Cell Biol. 2018;20(7):745–54.
53. Chung KW, Dhillon P, Huang S, Sheng X, Shrestha R, Qiu C, Kaufman BA, Park J, Pei L, Baur J, Palmer M, Susztak K. Mitochondrial damage and activation of the STING pathway lead to renal inflammation and fibrosis. Cell Metab. 2019;30(4):784–99.
Zhumei Gao1,2, Chuyue Zhang1,3, Fei Peng1 , Qianqian Chen1 , Yinghua Zhao4 , Liangmei Chen5 , Xu Wang1 and Xiangmei Chen1,2
1 Department of Nephrology, First Medical Center of Chinese PLA General Hospital, Nephrology Institute of the Chinese People’s Liberation Army, State Key Laboratory of Kidney Diseases, National Clinical Research Center for Kidney Diseases, Beijing Key Laboratory of Kidney Disease Research, Beijing, China.
2 Department of Nephropathy, The Second Hospital of Jilin University, Changchun, China.
3 Kidney Research Institute, National Clinical Research Center for Geriatrics and Division of Nephrology, West China Hospital of Sichuan University, Chengdu, China.
4 School of Clinical Medicine, Tsinghua University, Beijing, China.
5 Department of Nephrology, The First Affiliated Hospital of Jinan University, Guangzhou, China.






