The Upper Limit Of Ultrafiltration Rate: The Latest Research Shows That There Are Individual Standards!
Apr 28, 2023
It is well known that excessive ultrafiltration rates can lead to a range of adverse clinical outcomes, such as hypotension and increased risk of death. Therefore, the domestic and foreign expert consensus and hemodialysis guidance documents recommend that the ultrafiltration rate in dialysis should be controlled below 13ml/kg/h1-3.

Click to cistanche beneficial for kidney disease
However, recent studies have shown that, despite the same ultrafiltration rate, there are large differences in the risk of death among patients of different body weights. This indicates that the upper limit of the ultrafiltration rate should be an individualized indicator rather than the target value recommended by similar guidelines.
On April 19, 2023, CJASN released a study from the United States. The study showed that in clinical practice, 19% and 7.5% of patients had hyperfiltration, which increased their risk of death by 20% or 40%, respectively. At the same time, the researchers formulated a new individualized ultrafiltration rate formula based on the patient's age, gender, weight, and other factors, aiming to assist doctors in adjusting the patient's ultrafiltration rate3.
Methods
This is a retrospective observational cohort study of patients receiving hemodialysis between January 1, 2015, and May 30, 2020. The inclusion criteria for this study were: ① age > 18 years old; ② receiving hemodialysis 3 times a week; ③ survival of at least 12 months after receiving hemodialysis.

The endpoint of the study was all-cause death. Baseline information of patients was collected, and the risk of death was adjusted for the patients. Ultrafiltration rate and post-dialysis body weight were used as continuous independent variables to fit Cox proportional hazards models. The relationship between ultrafiltration rate and post-dialysis body weight was explored by a bivariate function, and the optimal ultrafiltration rate was recommended according to the risk of death.
Results
A total of 396,358 patients were enrolled, of which 58% were male, with an average age of 62±14 years, and 41% of patients had diabetes. The average ultrafiltration rate was 582±226 ml/h, the average Kt/V was 1.61±0.27, the average urea decline rate (URR) was 74±6%, and the average body weight before and after dialysis was 85.2±24kg and 83.2± 23kg, with an average body mass index (BMI) of 29.1±7.5kg/㎡.
During the 2-year follow-up period, 68,323 patients died, with mortality rates of 13.9 and 19.7 per 100 patient-years at 1 and 2 years, respectively. Figure 1 shows the effect of post-dialysis body weight and ultrafiltration rate on the risk of death. It is not difficult to find that after adjusting for race, age, sex, diabetes, blood pressure, albumin, and phosphate levels, there is a linear relationship between body weight, ultrafiltration rate, and risk of death. It is worth noting that the proportion of patients with a mortality hazard ratio (MHR) of 1.2 or 1.4 in this study was 19% and 7.5%, respectively.
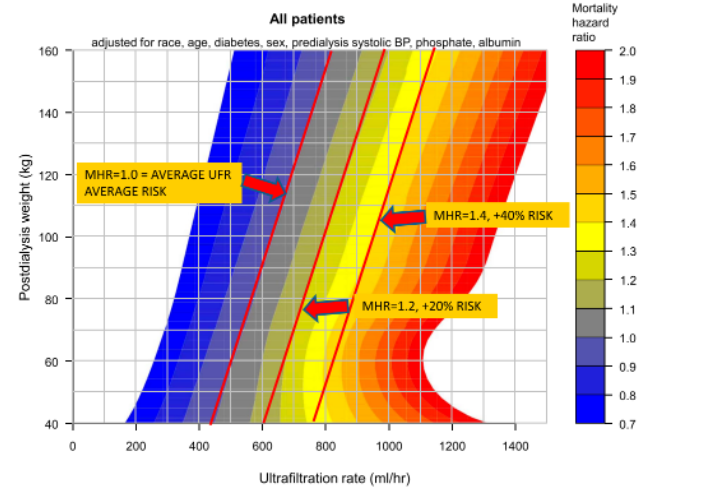
Figure 1 Discrete graph of death risk
Remarks: The redder the color, the higher the MHR. MHR is the hazard ratio for death
The relationship between ultrafiltration rate (ml/h) and body weight after dialysis was calculated when MHR was 1.0, 1.2, and 1.4.
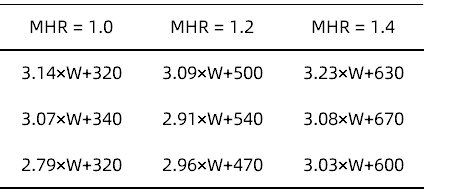
Table 1 Relationship between MHR and ultrafiltration rate and body weight after dialysis
Note: W is the average body weight after dialysis, in kg. For example, if the MHR of an 80kg male patient is to be 1.0, the upper limit of the ultrafiltration rate is 3.07×80+340 = 585.6ml/h.
In subgroup analyses, age and dialysis history were also important factors influencing ultrafiltration rates. According to age, patients were divided into the 19-40-year-old group, the 41-70-year-old group, and the≥71-year-old group. When MHR = 1.2, it was found that the ultrafiltration rates of the 19-40-year-old group and the 41-70-year-old group were linearly similar, but there was a certain difference with the ultrafiltration rate of the ≥71-year-old group (Figure 2).

Figure 2 Relationship between age and ultrafiltration rate
According to the history of dialysis, the patients were divided into three groups: <12 months, 12-36 months, and >12 months. When MHR = 1.2, it was found that the ultrafiltration rate was linearly similar in patients <12 months and 12-36 months, but there was a certain difference with the>12 months group (Fig. 3).
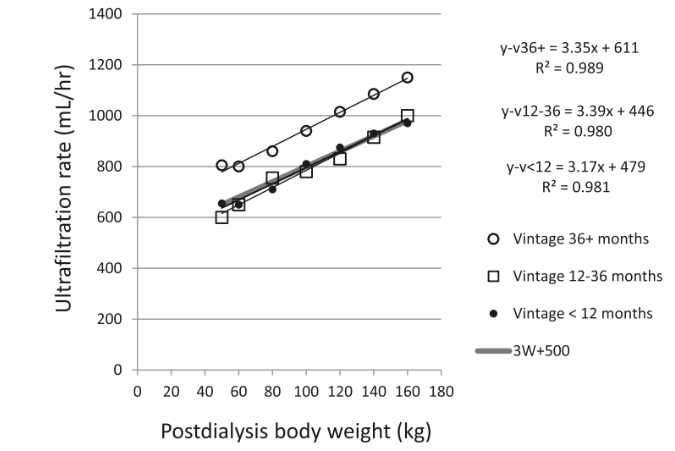
Figure 3 The relationship between dialysis history and ultrafiltration rate
In addition, other factors of the patient, such as height and blood pressure, did not affect the dialysis rate.
In general, the relationship between ultrafiltration rate and body weight is complex, and the patient's gender, age, and dialysis history also have an important impact on the ultrafiltration rate. Therefore, the setting of the ultrafiltration rate should be individualized, rather than simply sticking to the goal of <13ml/kg/h. While this metric may work for some patients, it may not work for others.

At the same time, the study also found that in clinical practice, 19% and 7.5% of patients had an excessively high ultrafiltration rate, which could lead to an increased risk of death in patients. The study suggests that more research on ultrafiltration rate should be carried out in the future, and more clinical characteristics should be included to develop an individualized ultrafiltration rate formula, to improve the safety of hemodialysis.
The Mechanism of Cistanche Treatment Kidney disease
Cistanche is a traditional Chinese herb that has been used for centuries to treat various health conditions, including kidney disease. The exact mechanism by which Cistanche treats kidney disease is not fully understood, but it is believed to have several beneficial effects on the kidneys. One way that Cistanche may help treat kidney disease is by increasing blood flow to the kidneys. This can help to improve overall kidney function and reduce the risk of kidney damage. Cistanche may also have a protective effect on the kidneys, helping to prevent damage from toxins or other harmful substances in the body.

Additionally, Cistanche is thought to have anti-inflammatory properties, which may help to reduce inflammation in the kidneys and improve kidney function. It may also have antioxidant effects, which can help to protect the kidneys from damage caused by free radicals. Overall, while the exact mechanism by which Cistanche treats kidney disease is not fully understood, it is believed to have a range of beneficial effects on kidney function and health.
References:
1. Standard Operating Procedures for Blood Purification 2021 Edition. National Medical Letter [2021] No. 552. Link: http://www.nhc.gov.cn/cms-search/xxgk/getManuscriptXxgk.htm?id=6e25b8260b214c55886d6f0512c1e53f
2. Hemodialysis Hypotension Prevention and Treatment Expert Group of Nephrology and Blood Purification Professional Committee of China Medical Education Association. Expert consensus on prevention and treatment of hypotension in hemodialysis (2022) [J]. Chinese Journal of Internal Medicine, 2022, 61(3): 269-281.
3. Mermelstein A, Raimann JG, Wang Y, et al. Ultrafiltration Rate Levels in Hemodialysis Patients Associated with Weight-Specific Mortality Risks. Clin J Am Soc Nephrol. 2023 Apr 19.






