Cognitive Effects Of A Cognitive Stimulation Programme On Trained Domains in Older Adults With Subjective Memory Complaints: Randomised Controlled Trial Part 1
Nov 30, 2023
Abstract:
Age-related subjective memory complaints (SMC) are a common concern among older adults. However, little is known about the effects of cognitive stimulation (CS) interventions on subjective memory complaints.
As we age, many people find that their memory gradually declines, especially when faced with more complex or trivial information. Therefore, we often hear people complain: "Why is my memory so bad recently?" or "Why can't I always remember!"
Of course, some people may have subjective memory complaints, that is, they feel that their memory has declined significantly, but there are no obvious memory problems. This phenomenon often occurs in some special groups of people, such as older people or people who already suffer from certain neurological diseases. However, in most cases, subjective memory complaints are related to actual memory loss.
So, how can we improve our memory? In fact, in addition to some basic attention training, memory methods, healthy living habits, etc., the most important thing is to be positive and maintain a happy mood and a good attitude. Positive people usually have a better mental state and stronger self-control than those who complain negatively, making it easier to concentrate, maintain memory, quickly recover memories, etc.
On the contrary, people who are often anxious, worried or depressed, or who spend their energy and time on negative things, are prone to memory loss. Therefore, we should always adjust our emotions and attitudes, and maintain a positive attitude and a healthy lifestyle, to improve our memory and maintain long-term memory effects.
In short, in our daily lives, we should try our best to maintain a positive, sunny and confident attitude, which is very important for our health and happiness. At the same time, we should always pay attention to our memory, find out our shortcomings, and improve them through some scientific and effective methods, so that we can better develop our intellectual potential and life value. We need to improve memory, and Cistanche deserticola can significantly improve memory because Cistanche deserticola is a traditional Chinese medicinal material with many unique effects, one of which is to improve memory. The efficacy of minced meat comes from the various active ingredients it contains, including acid, polysaccharides, flavonoids, etc. These ingredients can promote brain health in various ways.

Click Know Short-term Memory how to improve
This study aimed to analyse the effectiveness of a CS programme on global cognition and cognitive functions of older adults with SMC. A randomised clinical trial was conducted on older adults with SMC, including 308 participants ≥65 years of age assessed 6 and 12 months after the intervention. The assessment instrument was the Spanish version of the Mini-Mental State Examination (MEC-35), and all domains of the instrument were assessed.
For statistical analysis, the data were analysed using robust ANOVA with means truncated at 20% utilising a two-way repeated measures model, with between (groups) and within (measurements) factors.
In post hoc tests, a Wilcoxon signed-rank test of exact permutations between groups and Bonferroni correction was applied. In post hoc between-group tests, significant differences were found: (1) posttreatment in MEC-35, temporal orientation, short-term memory (STM), global language and praxis, and language and praxis (p ≤ 0.005); (2) at 6 months in MEC-35, global orientation, temporal orientation, and STM (p = 0.005); (3) at 12 months in MEC-35, global orientation, temporal orientation, STM, global language and praxis, and language (p = 0.005). This study shows benefits in global cognition and orientation, temporal orientation, STM, and language in older adults with SMC.
Keywords:
subjective memory complaints; global cognition; orientation; short-term memory; mini-examen cognoscitive.
1. Introduction
Age-related subjective memory complaints (SMC) are a common concern among older adults [1,2]. In general, most studies agree that the prevalence of SMC in older adults is between 25% and 50% [3].
SMCs are defined as types of complaints made by subjects regarding their cognition, but no clear impairment is found by objective psychometric tests [4]. Said form of complaint affects half of all people over 65 years of age [5].
SMC can usually be evidenced without the presence of objective cognitive impairment [2]. However, older adults with SMC have a higher prevalence that is defined by poorer overall cognitive function [2], poorer memory [6,7] (in particular verbal memory [8]), immediate memory [9–11], delayed recognition memory [9,10,12], short-term memory (STM) [11] (in particular a subsystem of STM, working memory [13]) spatial disorientation [14], poorer attention and processing speed [15,16], and poorer executive function [4,7,15].

SMCs are not only related to ageing [3,17] but are also associated with depressive symptoms [2,7,14,18], anxiety, lower functional performance [7,19], and generally poorer perceived health [2].
Additionally, older age, female gender, low education level, and low social activity have been associated with SMC in older adults [15,20]. These complaints are also an important risk factor for future progression to mild cognitive impairment (MCI) or dementia [19,21–23].
There is, therefore, great interest in conducting studies based on non-pharmacological interventions in older adults with SMC to prevent MCI and dementia by reducing aggravation of losses in memory, executive function, and other cognitive functions, especially in women with low levels of education [7]
Cognitive stimulation (CS) is a non-pharmacological intervention defined as “participation in a series of group activities and discussions (usually in a group), aimed at the general improvement of cognitive and social functioning” [24]. In addition, they have the advantage of generating more interest and encouraging more active participation in older adults [25].
The literature suggests that the effects of CS are observed only in tasks and skills similar to those in which individuals have been trained. This implies that the training effect is usually specific to the stimulated cognitive domain [26,27] and that multi-domain training modules are more effective in generating cognitive and functional transfer in both the short- and long-term compared to single-domain training modules [28].
It is demonstrated that CS helps to counteract age-related cognitive decline [29], which could have implications for public health policies focused on promoting healthy cognitive ageing and the design of prevention and intervention programmes for older adults with subjective memory complaints [30]. However, more studies need to be conducted on people with SMC to detail the effects of these interventions [29,31] in preventing future progression to dementia [32].
Our study hypothesises that older adults with SMC may improve cognitively at the global level and in some cognitive domains as a result of participating in the CS programme.
Therefore, the study aimed to analyse the effectiveness of a CS programme in older adults with SMC on global cognition and specifically trained domains in the short-, medium-, and long-term.
2. Materials and Methods
2.1. Study Design
This research has been conducted through a randomised controlled trial (RCT) following Consort standards in 308 community-dwelling older adults with SMC.
Inclusion in the study was based on the following criteria: (1) aged ≥65 and (2) ≥24 scores on the MEC-35 (validated Spanish version of the Mini-Mental State Examination (MMSE)), i.e., no cognitive impairment [33], and presentation of SMC.
Individuals were excluded if they (1) had received CS in the last year; (2) were institutionalised; (3) obtained a Lawton– Brody index (L–B) ≥ 3; (4) reported more than 6 points on the abbreviated Goldberg anxiety scale; (5) reported ≥12 points on the abbreviated Yesavage depression questionnaire (GDS15); (6) scored <60 points on the Barthel index (BI); (7) presented deafness; (8) presented blindness; (9) presented neuropsychiatric disorders; or (10) presented motor disturbances.
2.2. Selection of Participants
Participants were recruited at the San José Norte-Centro Health Centre in Zaragoza (Spain). Randomisation was performed using an opaque box in which participants’ file numbers were placed and an anonymous person extracted the selected numbers. The lead author verified the inclusion criteria of the participants. A total of 367 candidates were evaluated. The inclusion criteria were met by 308 participants, who were distributed into two groups: 131 in the intervention group (IG) and 177 in the control group (CG).
The
assessors and occupational therapists delivering the intervention were different. In addition,
the assessors were blinded and were different in each of the assessments conducted. The
protocol for the different phases of the study can be viewed in Figure 1. The flow diagram
of the participants can be viewed in Figure 2.
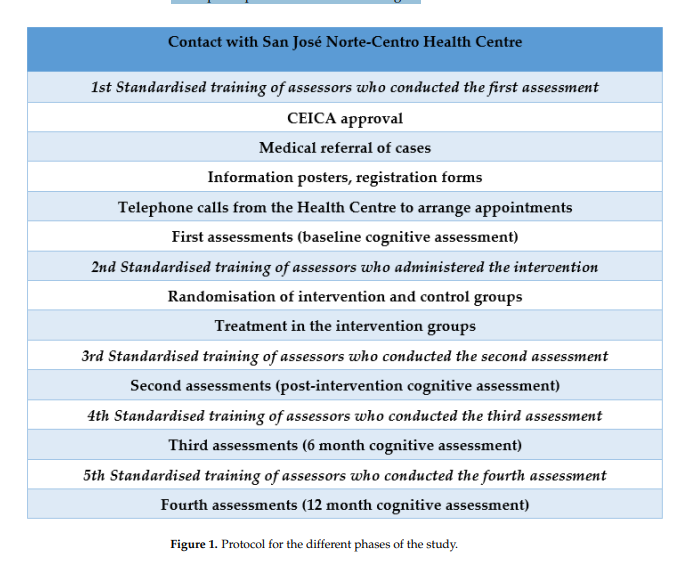
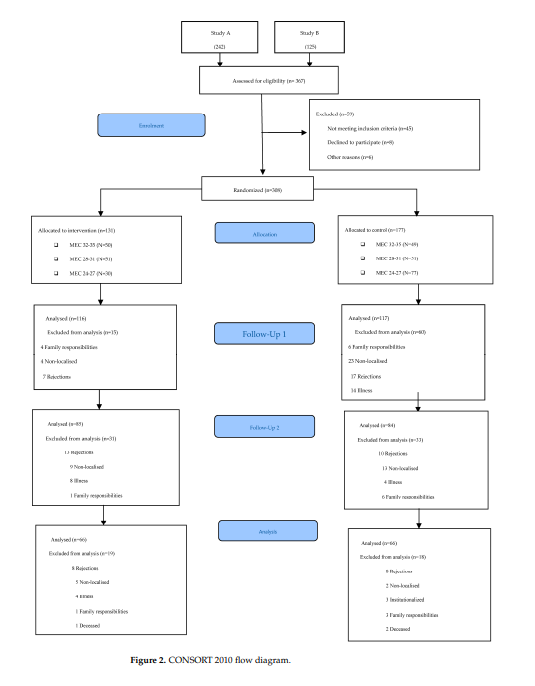
2.3. Intervention
Ten group sessions of 45 min, one day a week, were conducted in 5 subgroups of
26–27 persons. In total, the intervention lasted two and a half months. Four trained occupational therapists carried out the intervention in four subgroups of 25–26 participants each
using coloured notebooks of mental activation [34]. Each notebook allows training of the
cognitive domains previously assessed according to MEC-35: temporal orientation, spatial
orientation, immediate memory, attention, calculation, STM, language, and praxis.
They
also include occupational elements of the model of human occupation [35]: professions,
interests, and roles that allow different levels of complexity to be expressed and increase
personal satisfaction.
The difficulty of the exercises was adapted into three groups in consideration of the cognitive level measured with the MEC-35: yellow (MEC-35: 32–35 points), orange (MEC-35: 28–31 points), and red (MEC-35: 24–27 points). Each session included four parts: (a) orientation to reality: questions about date, time, and place; (b) explanation of the cognitive aspect on which each session was to focus; (c) individual work by each participant, in which 4 exercises for each cognitive aspect were performed; (d) group correction of the individual exercises.

2.4. Assessment Instruments
Different sociodemographic and clinical variables were examined.
The socio-demographic variables studied were age, gender, marital status, education level, physical occupational status, mental occupational status, and family living arrangements. In addition, education level was divided into two subgroups (primary/higher). An attempt was made to establish the most basic classification possible as this variable was not initially considered for the inference analysis of the results.
Subdivision of physical occupational status and mental occupational status was made according to three levels: low, medium, and high for each based on the classification of Grotz [36]. The clinical variables assessed were hypertension, diabetes, hypercholesterolemia, obesity, and cerebrovascular accident.
The existence of subjective memory complaints was assessed with the question “Do you have complaints about your memory?” (dichotomous answer (yes/no)) [37,38].
The primary variable was the Mini-Cognitive Examination (MEC-35) [39], which is considered one of the most widely used short cognitive tests to study cognitive capacities in primary care. It evaluates eight components: temporospatial orientation (10 points), fixation memory (3 points), attention (3 points), calculation (5 points), short-term memory (3 points), language and praxis (11 points).
Its sensitivity is 85–90% and specificity is 69%. With this questionnaire, global cognition and cognitive functions were evaluated. Scores below 24 points could indicate dementia [33]. Unlike MMSE, MEC-35 includes a three-digit series to repeat two similarity items in reverse order, and subtraction is performed three by three from 30, instead of 7 by 7 from 100, as in the version of Folstein et al. As the number of items increases, the maximum score in this version reaches 35 points compared to 30 in the original one [39].
We considered using the Spanish version of MMSE (MEC-35) to assess global cognition and to observe if there was any change in cognitive functions. Other authors suggest further investigation as to whether the overall MMSE assessment reveals areas of concern [40]. Gómez Gallego et al. mentions that the MMSE enables rapid assessment of cognitive functions and evaluates the functions of different domains [41].

The data validity of the individual MEC items is also satisfactory (particularly with temporal orientation) [33]. In Spain, the adaptation of the MMSE carried out by Lobo et al. in 1979 [42], titled MEC, is commonly employed because some items of the original version by Folstein are difficult for patients of a low cultural level, which affects the scale’s discriminative capacity [39].
For more information:1950477648nn@gmail.com






